Abstract
Background
Despite substantial increases in dental benefits and improvements in the use of dental services among children and adolescents in the United States, oral health disparities according to dental insurance payer type persist.
Methods
The authors used an all-payer claims (2013-2017) database to perform a comparative analysis of the provision and treatment outcomes of an endodontic procedure (root canal therapy) in the permanent teeth of a pediatric population aged 6 through 18 years, according to dental insurance payer type. Statistical analyses, including logistic regression, Cox proportional hazards regression, and the Kaplan-Meier method, were performed at person and tooth levels.
Results
Compared with privately insured children and adolescents, public-payer children and adolescent beneficiaries were more likely to have had root canal therapy (adjusted odds ratio, 1.91; 95% CI, 1.73 to 2.11) and had poorer treatment outcomes associated with the procedure (adjusted hazard ratio, 2.19; 95% CI, 1.53 to 3.14; P < .0001) during the study period. Those enrolled in private insurance were more likely to receive treatment from an endodontist (specialist in providing root canal therapy) (P < .0001). Amounts allowed and paid by the insurer were significantly higher for private payers (P < .001).
Conclusions
There were significant differences in the provision and outcomes of endodontic treatment between privately and publicly insured children and adolescents.
Practical Implications
Despite ostensibly equal access to care, differences in the provision of oral health care exist between privately and publicly insured patients. These differences may be contributing to persisting oral health disparities.
- Yu S.M.
- Bellamy H.A.
- Kogan M.D.
- Dunbar J.L.
- Schwalberg R.H.
- Schuster M.A.
,
- Yu Z.J.
- Elyasi M.
- Amin M.
The rate of dental coverage for all children in the United States has increased from approximately 70% in 1996 to approximately 90% in 2015.
- Edelstein B.L.
- Manski R.J.
- Moeller J.E.
,
The rate of pediatric dental coverage increase has been driven primarily by means of the expansions of publicly funded insurance programs.
, An estimated 51% of children in the United States have private dental benefits, and 39% are recipients of public-payer dental benefits (that is, Medicaid or Children’s Health Insurance Program [CHIP]).
Beyond dental insurance enrollment, as states have refined their dental benefits for children over time, public-payer coverage for children’s oral health care has become similar to private coverage, and oral health care use among public-payer beneficiaries has increased.
- Eklund S.A.
- Pittman J.L.
- Clark S.J.
,
- Hom J.M.
- Lee J.Y.
- Silverman J.
- Casamassimo P.S.
,
- Shariff J.A.
- Edelstein B.L.
- Shariff J.A.
- Edelstein B.L.
,
- Bhagavatula P.
- Xiang Q.
- Szabo A.
- Eichmiller F.
- Okunseri C.
,
- Nasseh K.
- Fosse C.
- Vujicic M.
,
- Dye B.A.
- Mitnik G.L.
- Iafolla T.J.
- Vargas C.M.
One of the most common chronic diseases of childhood is caries. In the United States, the prevalence and disease severity of caries differ according to race and family income level.
- Dye B.A.
- Mitnik G.L.
- Iafolla T.J.
- Vargas C.M.
If left untreated, caries can cause pain, infection, and even tooth loss. Endodontic treatment, including root canal therapy, can be performed in an attempt to maintain the natural dentition and prevent negative lifelong consequences that can result from pain, infection, and premature tooth loss. Few investigators have explored comparative dental procedure use or dental procedure mix between public-payer beneficiaries and private-payer dental insurance enrollees, particularly for endodontic treatment. In previous studies with both pediatric and adult populations, investigators found that public-payer beneficiaries were more likely to receive endodontic treatment than those who were privately insured.
- Bhagavatula P.
- Xiang Q.
- Szabo A.
- Eichmiller F.
- Okunseri C.
,
- Nasseh K.
- Fosse C.
- Vujicic M.
,
- Sweet M.
- Damiano P.
- Rivera E.
- Kuthy R.
- Heller K.
To our knowledge, no researchers have explored the differences in endodontic treatment outcomes according to insurance type. Differences in treatment outcomes may be worth exploring in light of existing disparities in oral health status, despite the increased access to oral health care that expansions of publicly funded insurance programs have afforded.
In this study, we investigated the differences in provision, treatment outcomes, and cost of initial root canal therapy according to dental benefit payer type.
Methods
Data sources
includes dental claims and information on member eligibility, provider, and insurance type, which are collected from health insurance payers licensed to operate in the Commonwealth of Massachusetts. Release Version 7.0 was inclusive for years 2013 through 2017 and contained records for 1,516,624 children aged 6 through 18 years; 539,966 (36%) were Medicaid beneficiaries, and 976,658 (64%) were enrolled in private insurance plans. This research is part of a data use agreement approved by the Center for Health Information and Analysis (1491238-1). This study was approved by New York University School of Medicine’s Institutional Review Board (i19-01436).
Variables
The analytic data set contained the following information for each patient: unique identification number, dates of enrollment and disenrollment, dental insurance payer type (private vs public or Medicaid), age at date of treatment, sex, ZIP Code of residence, date of treatment, procedure code for the treatment provided, tooth number treated, provider’s specialty code, and payment information for the procedures (that is, the maximum amount contractually allowed and that an insurer will pay for the procedure or the amount paid by the insurer).
Current Dental Terminology.
(CDT) were used to identify the endodontic treatment procedures for analysis (D3310, D3320, D3330). Furthermore, CDT codes were used to identify an adverse event after initial root canal therapy. Adverse events were defined as nonsurgical endodontic retreatment (D3346, D3347, D3348), surgical endodontic retreatment or apicoectomy (D3410, D3421, D3425), or tooth extraction (D7140, D7210), and indicated failure of the initial root canal therapy. Provider specialty codes were used to determine the provider type, either individual providers or facilities. Individual providers included general (nonspecialist) dentists and specialist dentists. Dental specialists included endodontists (specialists in performing root canal therapy), pediatric dentists, prosthodontists, periodontists, orthodontists, and oral surgeons. Individual providers were dichotomized into endodontist and other individual providers for the analyses. Facilities included provider specialty codes identified as clinic or center and hospitals.
Statistical analyses
Data analysis was completed using SAS software, Version 9.4 (SAS Institute) and R, Version 4.0 (R Core Team). Provision of initial root canal therapy was analyzed at the person level. Patients who received initial root canal therapy within the study period of 2013 through 2017 and who had complete payer-type data were included in the final data set. Treatment outcomes of initial root canal therapy were measured at the tooth level. For tooth-level analysis, patients were excluded if they had less than 1 year of insurance enrollment after treatment or records of treatment were missing the associated tooth number. To ensure external validity, χ2 tests and t tests were used to compare characteristics between those excluded due to missing tooth number and those included in the sample.
Multiple logistic regression was used to measure the association between payer-type and initial root canal therapy at the person level, with adjustments for age, sex, tooth type (anterior, premolar, molar), and provider type.
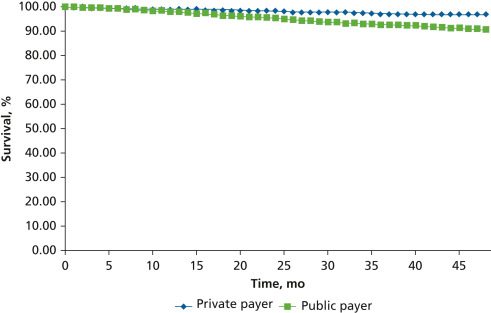
For the evaluation of procedural outcomes at the tooth level, initial root canal therapies were considered successful unless there was an adverse event (tooth extraction, endodontic retreatment, apicoectomy) or they were censored at an identified lapse in the patient’s insurance enrollment. The Kaplan-Meier method was used to estimate procedural survival according to payer type. Cox proportional hazard regression was used to evaluate the hazard of adverse event occurrence after initial root canal therapy, according to payer type (public or private), using a model that adjusted for the following covariates: age, sex, tooth type, and provider type. Member identification was also included in this model to account for person-level clustering and to generate estimates with robust SEs. In addition, this methodology was used to assess procedural survival according to provider type in a subset of the sample limited to procedures completed by an individual provider, with the adjusted Cox proportional hazard model controlling for age, sex, tooth type, and payer type.
The payment data (amounts allowed and paid via the insurer) for initial root canal therapy were summarized according to both payer and tooth type. Wilcoxon rank-sum tests were used to test for the statistical significance of differences in paid and allowed amounts according to payer type for each tooth type (that is, anterior, premolar, and molar). Statistical significance level (α) of .05 was used for all analyses.
Results
Source: Center for Health Information and Analysis.14
Source: Center for Health Information and Analysis.14
For initial root canal therapies that failed during the study period (n = 1,295 [6.4%]), the first identified adverse event was tooth extraction in 78% of cases (n = 1,016) and surgical or nonsurgical retreatment in 21.5% of cases (n = 279). No statistically significant difference was detected for type of adverse events according to payer type (P = .721).
Current Dental Terminology.
(D3310 for anterior, D3320 for premolar, D3330 for molar) for the first treatment each patient received are reported in Table 3. Amounts allowed and paid by the insurer were significantly higher for those privately insured, regardless of tooth type (P
Source: Center for Health Information and Analysis.14
Discussion
,
, ,
- Shariff J.A.
- Edelstein B.L.
,
CMS Oral Health Initiative and Dental Technical Support Opportunity.
However, differences in the dental procedure mix for children and adolescents are prevalent; public-payer beneficiaries are more likely to undergo a higher share of therapeutic dental services, including endodontic treatment.
- Bhagavatula P.
- Xiang Q.
- Szabo A.
- Eichmiller F.
- Okunseri C.
,
- Nasseh K.
- Fosse C.
- Vujicic M.
,
- Sweet M.
- Damiano P.
- Rivera E.
- Kuthy R.
- Heller K.
Our findings support those of investigators reporting that pediatric public-payer beneficiaries receive more endodontic treatment, including root canal therapy, than their counterparts with private dental coverage.
- Bhagavatula P.
- Xiang Q.
- Szabo A.
- Eichmiller F.
- Okunseri C.
,
- Nasseh K.
- Fosse C.
- Vujicic M.
,
- Sweet M.
- Damiano P.
- Rivera E.
- Kuthy R.
- Heller K.
Although the survival rates of initial root canal therapy performed on the permanent teeth of children and adolescents were high for both groups at 1 and 3 years postoperatively, our findings indicate potential disparities in treatment outcomes, as beneficiaries of public dental insurance were more likely to experience procedural failures after root canal therapy than those with private-payer insurance.
Current Dental Terminology.
code that identifies this procedure does not include tooth type (that is, anterior, premolar, or molar), as is done for endodontic treatments. Without the tooth number, there was too high a risk that a downstream, unrelated tooth extraction may be incorrectly associated with the initial root canal therapy. Another factor potentially limiting the generalizability of our findings is that we have included data from only 1 state, Massachusetts. However, the findings for public-payer (Medicaid, CHIP) beneficiaries in our study were comparable with findings from a cohort of pediatric Medicaid beneficiaries from New York.
- Burns L.E.
- Terlizzi K.
- Solis-Roman C.
- Wu Y.
- Sigurdsson A.
- Gold H.T.
To our knowledge, a comparable study does not yet exist for a cohort of privately insured children. Second, as in all studies using dental claims data, the initial diagnosis for the treated teeth could not be determined due to the nonclinical nature of the administrative data and the absence of diagnostic codes in dentistry. This is particularly relevant to our study, as endodontic diagnosis is known to be associated with endodontic treatment outcomes.
- Ng Y.L.
- Mann V.
- Rahbaran S.
- Lewsey J.
- Gulabivala K.
,
- Burns L.E.
- Kim J.
- Wu Y.
- Alzwaideh R.
- McGowan R.
- Sigurdsson A.
Despite these limitations, our study results provide insights regarding access to oral health care for children with public or private dental insurance in the Commonwealth of Massachusetts related to the prevalence of endodontic treatment and access to dental care providers and treatment settings.
- Shariff J.A.
- Edelstein B.L.
,
- Dye B.A.
- Mitnik G.L.
- Iafolla T.J.
- Vargas C.M.
Realized disparities in procedural outcomes of root canal therapy according to payer type may also be attributable to differences in treatment setting or dentist provider types. In previous studies using similar methodology, root canal therapies performed by endodontists have been associated with improved outcomes.
American Dental Association Survey Center: 2005-2006 Survey of Dental Services Rendered.
,
It was difficult to make this distinction in our study, as payer type and treatment setting or provider type were so closely associated (P
American Dental Association Survey Center: 2005-2006 Survey of Dental Services Rendered.
Our findings, therefore, suggest that endodontists may be more likely to treat children requiring root canal therapy than other dental care providers. Nationally, 43% of all dentists, 73% of pediatric dentists, and only 28% of endodontists, participate in Medicaid for child dental services.
American Dental Association Survey Center: 2005-2006 Survey of Dental Services Rendered.
In our study, none of the root canal therapy procedure claims for publicly insured children were associated with a provider specialty code for an endodontist as an individual dental care provider; however, it is possible that when treated in a facility setting, an endodontist was the provider. Facilities (clinics, centers, hospitals) are likely to be dental schools or federally qualified health centers and may employ endodontists or have postgraduate trainees specializing in endodontics as providers. When these facts are considered, one could question whether access to endodontic treatment is limited for pediatric patients enrolled in public insurance.
,
- Buchmueller T.C.
- Orzol S.
- Shore-Sheppard L.D.
,
,
,
- Chalmers N.I.
- Compton R.D.
,
- Ku L.
- Han X.
- Chen C.
- Vujicic M.
The findings of our study highlighted differences in both allowed and paid amounts for root canal therapy procedure claims billed by insurers, with the amounts allowed and paid by private payers higher than those by public payers. In Massachusetts in 2017, Medicaid reimbursement as a percentage of private insurance reimbursements for diagnostic and preventative dental services was 74%.
We found that the reimbursement percentage was higher for the specific endodontic procedure of root canal therapy on premolars and molars. This may be due to the fact that endodontic treatment performed on premolars and molars generally have higher levels of case difficulty. In the same year (2017) in Massachusetts, 51% of dentists were enrolled as Medicaid providers, but only 26% of Massachusetts dentists had seen Medicaid patients in the past year.
Future research aiming to increase understanding of dentists’ Medicaid participation, particularly for the provision of endodontic services to pediatric populations, will help inform strategies for increasing access to endodontic care for Medicaid enrollees.
,
Article Info
Publication History
Published online: December 16, 2022
Publication stage
In Press Corrected Proof
Footnotes
Disclosures. None of the authors reported any disclosures.
Research reported in this article was supported by grant K01DE028591 to Dr. Burns, principal investigator, from the National Institutes of Health National Institute of Dental and Craniofacial Research. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Identification
DOI: https://doi.org/10.1016/j.adaj.2022.10.011
Copyright
© 2022 American Dental Association.
User License
Creative Commons Attribution – NonCommercial – NoDerivs (CC BY-NC-ND 4.0) |

Permitted
For non-commercial purposes:
- Read, print & download
- Redistribute or republish the final article
- Text & data mine
- Translate the article (private use only, not for distribution)
- Reuse portions or extracts from the article in other works
Not Permitted
- Sell or re-use for commercial purposes
- Distribute translations or adaptations of the article
Elsevier’s open access license policy
ScienceDirect
Access this article on ScienceDirect