INTRODUCTION
Since their introduction, dental implant treatments, and the materials and technologies associated with their placement procedures, have expanded significantly. Digital radiography and cone-beam computed tomography (CBCT) have been incorporated into the planning process. Computer-assisted design and manufacturing (CAD/CAM) and 3D printing help streamline the protocols executed during scheduled treatment appointments.1 Combined, these technologies also help to realize advanced and comprehensive approaches to prosthetically driven implant treatment planning, resulting in more predictable outcomes for patients and greater efficiency for clinicians and the treatment team overall.
One of the ways in which these advancements have contributed to greater implant accuracy and precision is by aiding in the fabrication, manufacturing, and/or operation of dental implant surgical guides.2 As a result, today there is a plethora of different surgical guide options available to assist doctors in performing various aspects of the implant placement procedure (eg, osteotomies and implant placement).3 The primary goal of these devices or aids is to increase the placement precision and positional accuracy of the inserted implant(s).
Ensuring successful treatment outcomes when a dental implant placement surgical guide is to be used is predicated not only on the use of the guide itself, but also on selecting the right guide. This is based on its demonstrated success in contributing to predictable and accurate dental implant placement, how it will be used in the context of the patient’s oral anatomical environment, and the type or extent of guidance it provides.4
Without question, understanding the likelihood of success when using dental implant placement surgical guides is paramount when selecting from the available guide options.5 Fortunately, numerous research reports document the success of various dental implant surgical guides and/or systems to assist clinicians in selecting among predictable and accurate options.
Some accounts are based on observations of one specific type of surgical guide,6 while others provide a comparative analysis of the success rates of different kinds of guides fabricated from different materials and designed using different technologies and methods.1,7
The problem for clinicians when basing their decisions on published research and/or anecdotal reports is that the observations are based on too broad a range of guide types rather than more specific and descriptive surgical guide classifications. These are better indicators of their manner of use in various clinical scenarios.
For example, a recent (and admittedly not exhaustive) literature search can produce a list of studies that includes—but is not limited to—comparisons of implant placements using a navigation system, a laboratory guide, a laboratory guide with a navigation system, and freehand osteotomy.8 This search shows comparisons of fully guided, pilot guided, and freehand guided implant placement but focuses on clinicians new to implant dentistry,9 and an evaluation of the accuracy of different CAD/CAM dental implant surgical guides.10
Although the quality and/or level of detail with which these research studies were conducted may be beyond reproach, the conclusions drawn by these reports may confuse the clinicians who consult them for information on which to base their guide selection decisions.
Over the years, several authors have attempted to classify and categorize dental implant placement surgical guides according to various factors to facilitate their differentiation, evaluation, and selection. These have included, but are not limited to, the method and material of guide fabrication and whether or not the guide is used for a fully edentulous, partially edentulous, or partially edentulous and tooth-supported design.10
This includes the limiting and non-limiting nature of the guide and its abilities (or lack thereof) to direct and/or restrict osteotomy drills and implant drivers4,11 and the type of guide support, access fixation, and precision instrument guidance provided.3,10 Although helpful and informative, these may not fully enable dentists to compare various implant guide systems with a narrowed focus on the actual value proposition that each provides.12
Therefore, it is suggested that clinicians would benefit from a comprehensive dental implant surgical guide classification system that enables the use of a table identification tool to facilitate the selection of the most appropriate guide type for a given clinical scenario.
Such a classification system and accompanying decision table tool may potentially advance the standard of implant dental care by defining key attributes of dental implant surgical guides, facilitating guide selection among members of the treatment planning team, and enabling relevant outcome comparisons in future research endeavors.
DEFINING CLASSIFICATION GUIDE CATEGORIES
There are 3 key attributes of dental implant surgical guides that facilitate effective classification based on their capabilities and manner of use: constraint, reference frame, and timing.3,10Constraint refers to how the guide ensures proper implant placement, particularly in terms of controlling the osteotomy drills and implant drivers.3,10Reference frame describes how the guide functions (and/or is supported) within the oral cavity.3,10Timing refers to the guide’s ability to facilitate control of the implant’s rotational positioning when placed.
Classifying dental implant surgical guides in terms of these attributes helps to identify and understand their respective benefits and limitations, which can be beneficial when treatment planning cases and determining which type of guide is most appropriate for a given case. The proposed classification system presented here is intended to facilitate communication and decision-making; it is not intended as a commentary on the merits or shortcomings of any surgical guide type.
Constraints
The physical constraint mechanism or attribute of a dental implant surgical guide system helps ensure proper and ideal implant placement (ie, positioning the implant in a specific location that optimizes the form and function of the tooth replacement therapy). Ideal implant placement is best achieved by reducing positional error, which has colloquially been termed “knockout error,” and occurs when the osteotomy drill and/or implant is “knocked out” of the desired position.
This typically occurs when the drill or implant strikes regions of dense bone, causing migration into areas of softer bone.
Understandably, because it facilitates alignment and depth of the pilot drill, subsequent osteotomy, and implant placement, the physical constraint is usually the most discussed attribute of dental implant surgical guides. There are 5 potential types of physical constraints in this proposed classification system and selection table, as outlined and defined below.
Type 0: No Guide (Freehand Placement)
A Type 0 physical constraint classification refers to the use of no dental implant surgical guides and, therefore, the absence of any constraints on the osteotomy drills or implants during placement. It is colloquially referred to as “freehand” implant placement (Figure 1).3,10 Prior to the advent of dental implant surgical guide fabrication techniques and their associated technologies, Type 0 (freehand) placement was the approach undertaken by most clinicians.
Figure 1. Colloquially referred to as “freehand” implant placement, the absence of any constraints on the osteotomy drill or implant during placement is classified as a Type 0 physical constraint.
Type 1: Alignment (Visual) Aid
The Type 1 constraint classification refers to an alignment aid for an osteotomy drill and/or implant driver limited in scope to visual guidance (Figure 2).3,10 Although this type of dental implant placement guide provides real-time visual feedback during the osteotomy procedure and implant placement (ie, driving), it lacks any actual physical constraint of the osteotomy drills or implant driver. Examples of Type 1 guides include suck-down vacuforms placed over denture teeth and the Triad Lingual Drill Guide (Dentsply Sirona).
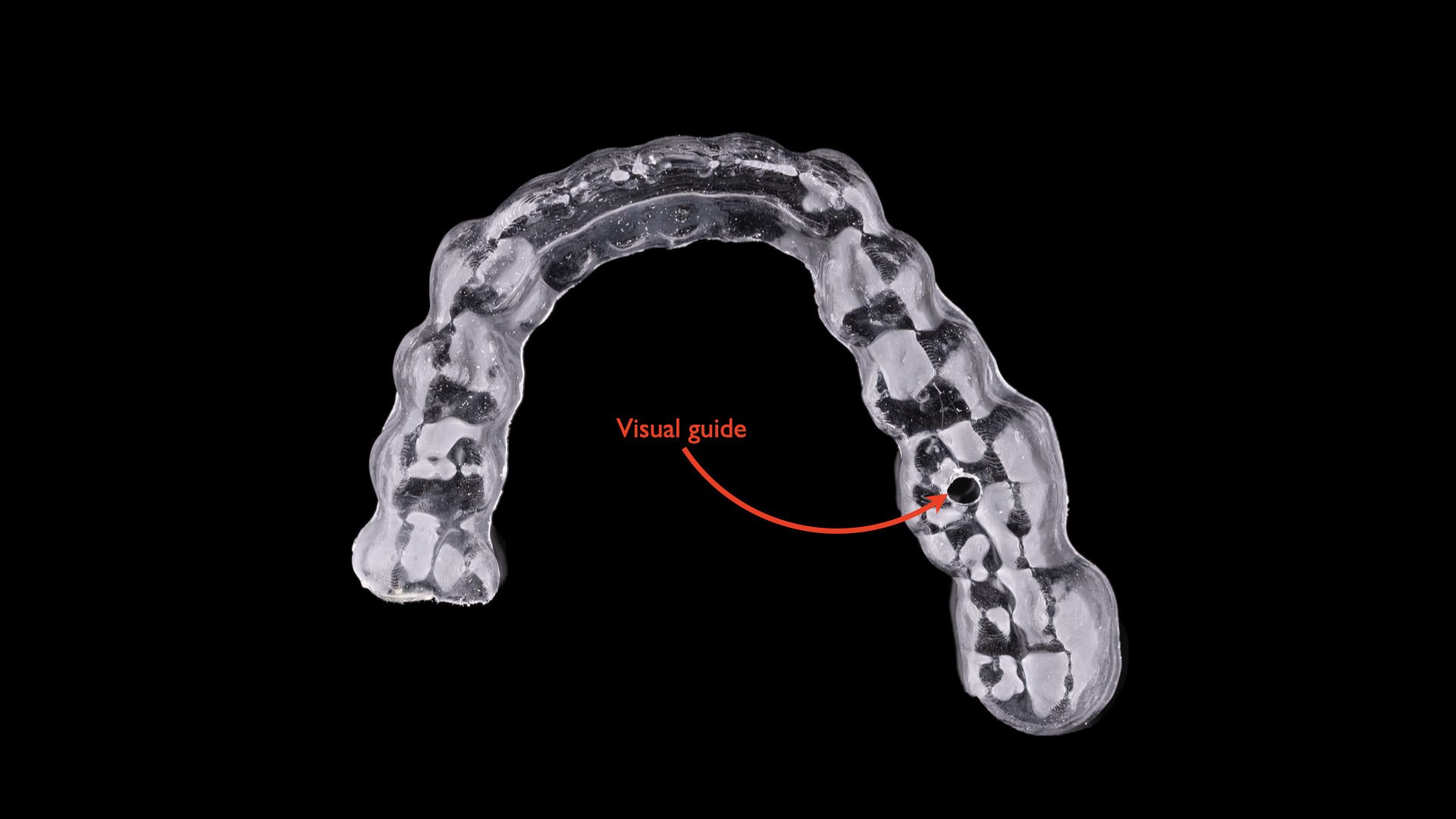
Figure 2. An example of a guide classified as Type 1 is a suck-down vacuform, which is limited in scope to visual guidance because it lacks any actual physical constraint of the osteotomy drill or implant driver.
Type 2: Pilot Drill Guide
Typically referred to as pilot drill guides, dental implant surgical guides classified as Type 2 only constrain the pilot drill, not the subsequent osteotomy.3,10 Since the most common starter pilot drills in dental implantology are 2.0 mm, this classification is easy to remember because it only refers to pilot drill guides. Type 2 guides are typically printed or milled and feature a master cylinder guide sleeve that accepts the 2.0-mm starter drill (Figure 3). Subsequent osteotomy drilling and implant placement then occur freehand. The primary clinical indication for a Type 2 dental implant surgical guide is a tight interproximal space, such as between the mandibular incisors, where the master cylinder needs only to accommodate the 2.0-mm pilot drill.
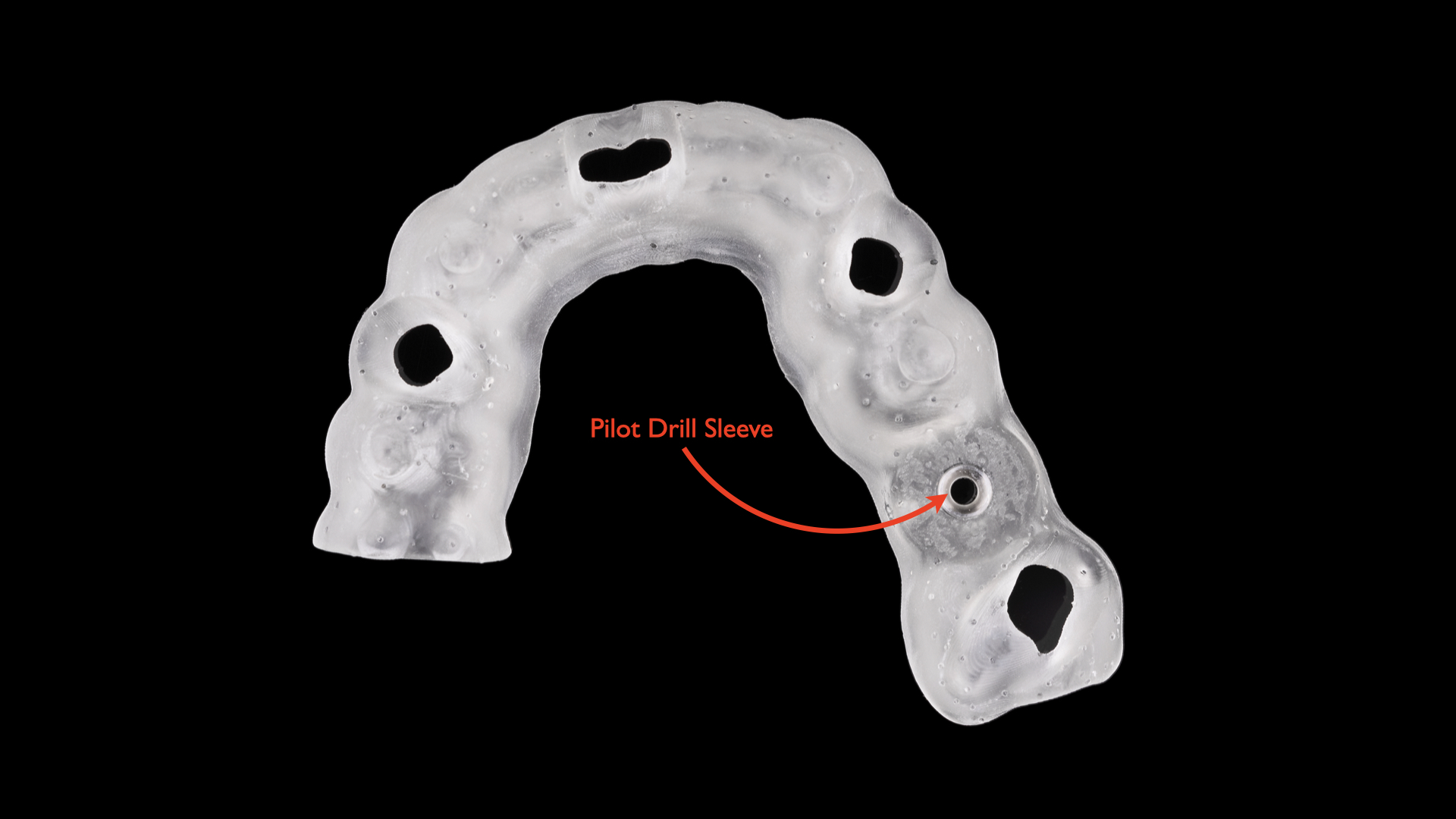
Figure 3. Type 2 guides only constrain the pilot drill, are typically printed or milled, and feature a pilot guide sleeve that accepts the 2.0-mm pilot drill.
Type 3: All Osteotomy Drills
Whereas a Type 2 guide facilitates pilot drilling, a Type 3 guide constrains the osteotomy drills.3,10 Typically manufactured using milling or 3D printing technologies, Type 3 dental implant surgical guides require digital planning software for their design (eg, CEREC2 [Dentsply Sirona] and the Zimmer Guided Surgery Kit [Zimmer Dental]) (Figure 4). Once the osteotomy is complete, implant placement proceeds freehand since the master cylinder is not designed to accommodate the subsequent implant placement.
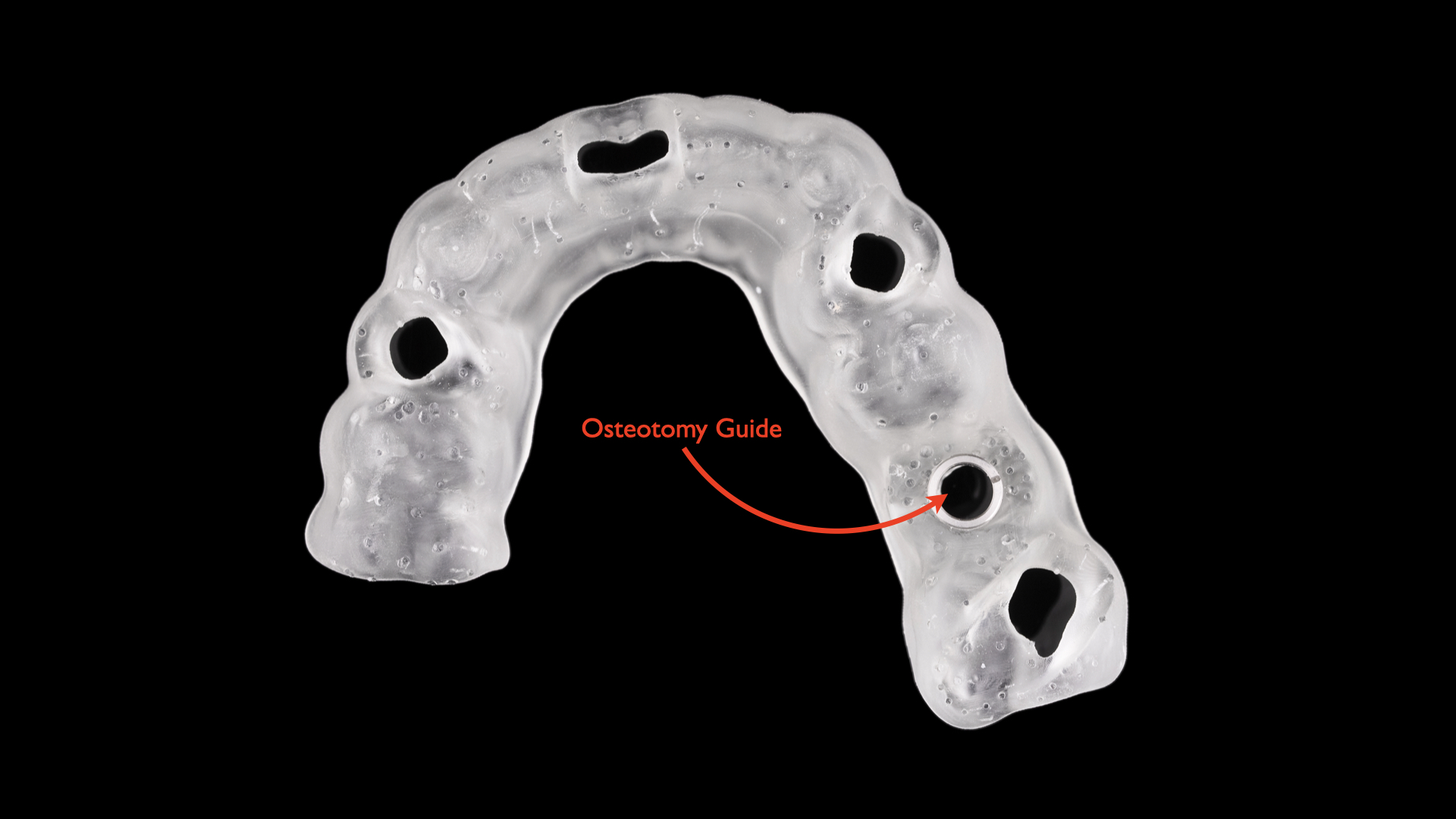
Figure 4. Type 3 guides constrain the osteotomy drills that are typically manufactured using milling or 3D printing technologies and therefore require digital planning software for their designs.
Type 4: Fully Guided (Osteotomy Drills and Implant Placement)
Type 4 dental implant surgical guides are often incorporated in fully guided dental implant placement procedures because they constrain the pilot drill, osteotomy drills, implant placement, and depth (Figure 5).3,10 Type 4 dental implant surgical guides (eg, Guided Surgery Kit [BioHorizons] and Safe System) often present the least risk of knockout errors or implants shifting during placement due to the redundancy of physical constraints they provide throughout the entire placement procedure.
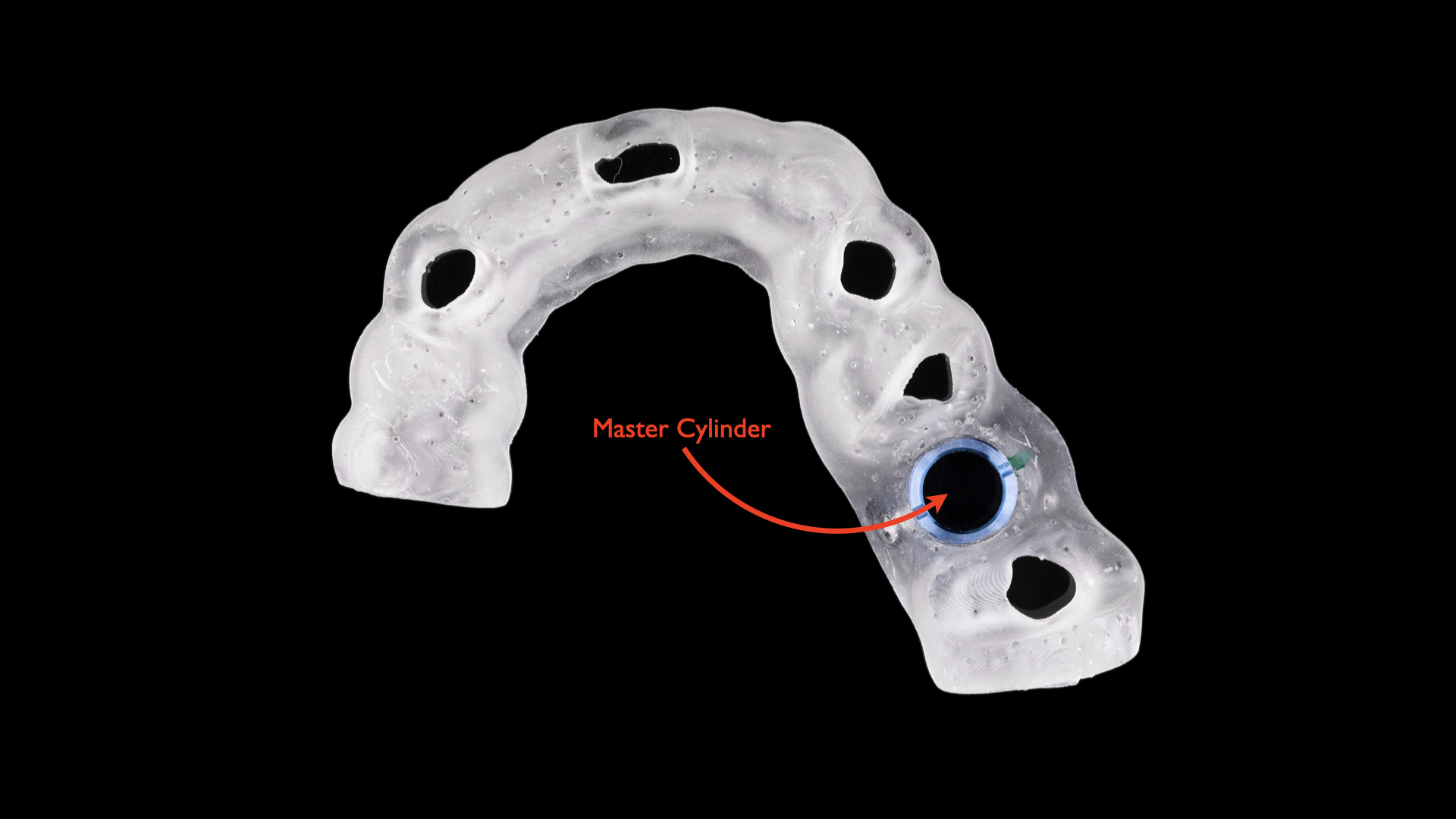
Figure 5. Type 4 dental implant surgical guides constrain the pilot drill, osteotomy drills, and implant placement, as well as control the depth of implant placement; they are therefore incorporated into fully guided dental implant placement.
Reference Frames and Support
The reference frame attribute refers to how the dental implant surgical guide relates to and functions within the patient’s mouth and/or how the physical constraints it provides will function and be supported. The more accurately the guide relates to the patient’s anatomy, the more precise the resulting implant placement will be.
While the physical constraint attribute classifies how the osteotomy drills, pilot drills, and implants will be directed, the reference frame attribute classifies how the guide translates the surgical plan to the patient’s mouth.3,10 In an ideal implant placement, the more accurate the translation of the desired treatment plan to the reference frame, the more optimal the placement outcome will be. Therefore, in this proposed classification system and selection table, there are 7 potential types of reference frames, as outlined and defined below.
Attached Gingiva/Mucosa
An example of an attached gingiva/mucosa reference frame is the case of an edentulous patient where the dental implant surgical guide will rest on the patient’s attached gingiva (Figure 6). Unfortunately, when gingival tissues are subjected to persistent mechanical stress, they deform as a function of stress over time and, therefore, can present unpredictably.
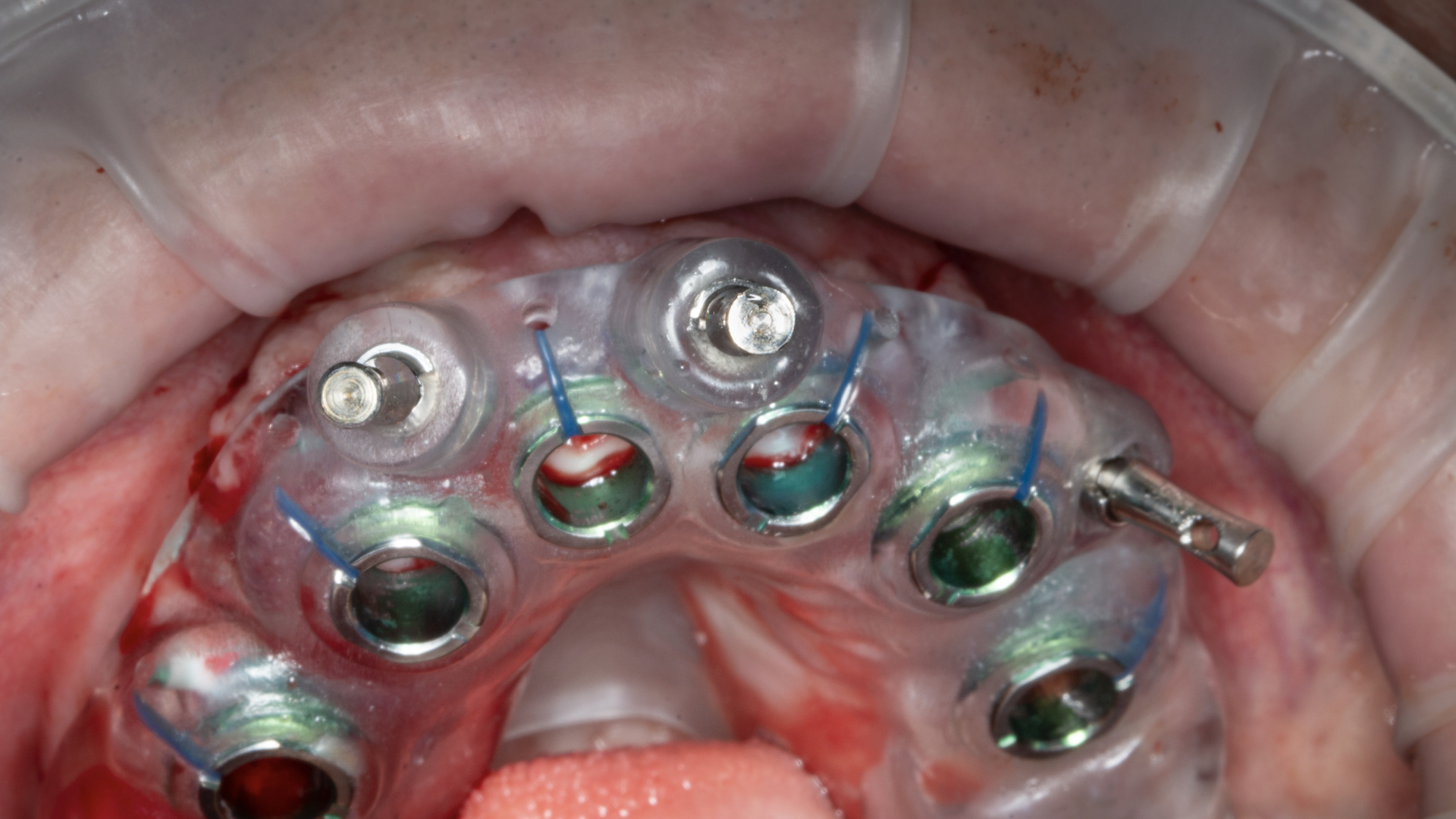
Figure 6. An example of Reference Frame A (attached gingiva/mucosa) is the case of an edentulous patient where the dental implant surgical guide rests on the patient’s attached gingiva.
This resembles the stress-induced tissue movement clinicians encounter when attempting to procure a passive, unstrained impression for a denture workup (ie, the soft tissue moves under stress). With the dental implant surgical guides classified as an attached gingiva/mucosa reference frame, there is a possibility of implant placement at a location that deviates from the plan if the reference frame moves and, subsequently, the guide also moves.
Bone
Another reference frame to support dental implant surgical guides is bone. A bone level reference frame and supported guide may facilitate more accurate and precise implant placement comparable to an attached gingiva-supported guide due to the viscoelastic nature of the gingiva (Figure 7).3 With dental implant surgical guides classified as a bone reference frame, a full thickness mucoperiosteal flap is elevated to enable the dental implant surgical guide to be seated on the bone.

Figure 7. In Reference Frame B (bone), a bone level supported guide may facilitate more accurate and precise implant placement.
Combination (Attached Mucosa and Dentition; Bone and Dentition)
The reference frame and support for dental implant surgical guides may also incorporate a combination of attached mucosa and dentition and/or a combination of underlying bone and adjacent dentition to facilitate ideal placement (Figure 8). Alternatively, the reference frame and support may include non-anatomical structures, such as integrated implants that often provide an excellent reference frame for additional implant placement.
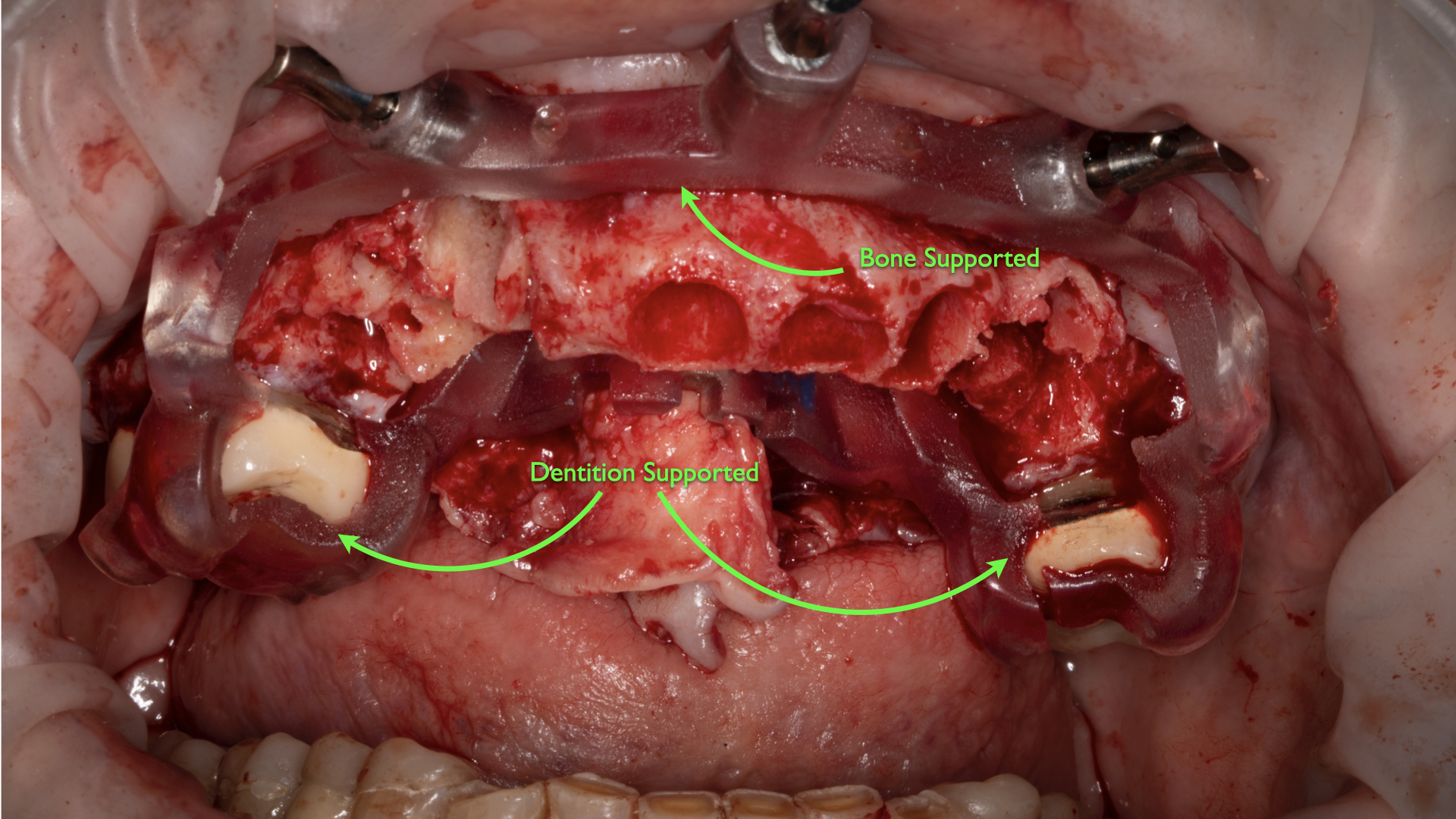
Figure 8. A combination of underlying bone and adjacent dentition may facilitate ideal placement in dental implant surgical guides classified as Reference Frame C.
Dentition
Adjacent and other remaining dentition represent another reference frame and support for dental implant surgical guides (Figure 9). Many guides characterized by their placement onto the patient’s existing and/or remaining dentition can be seated securely in this manner.
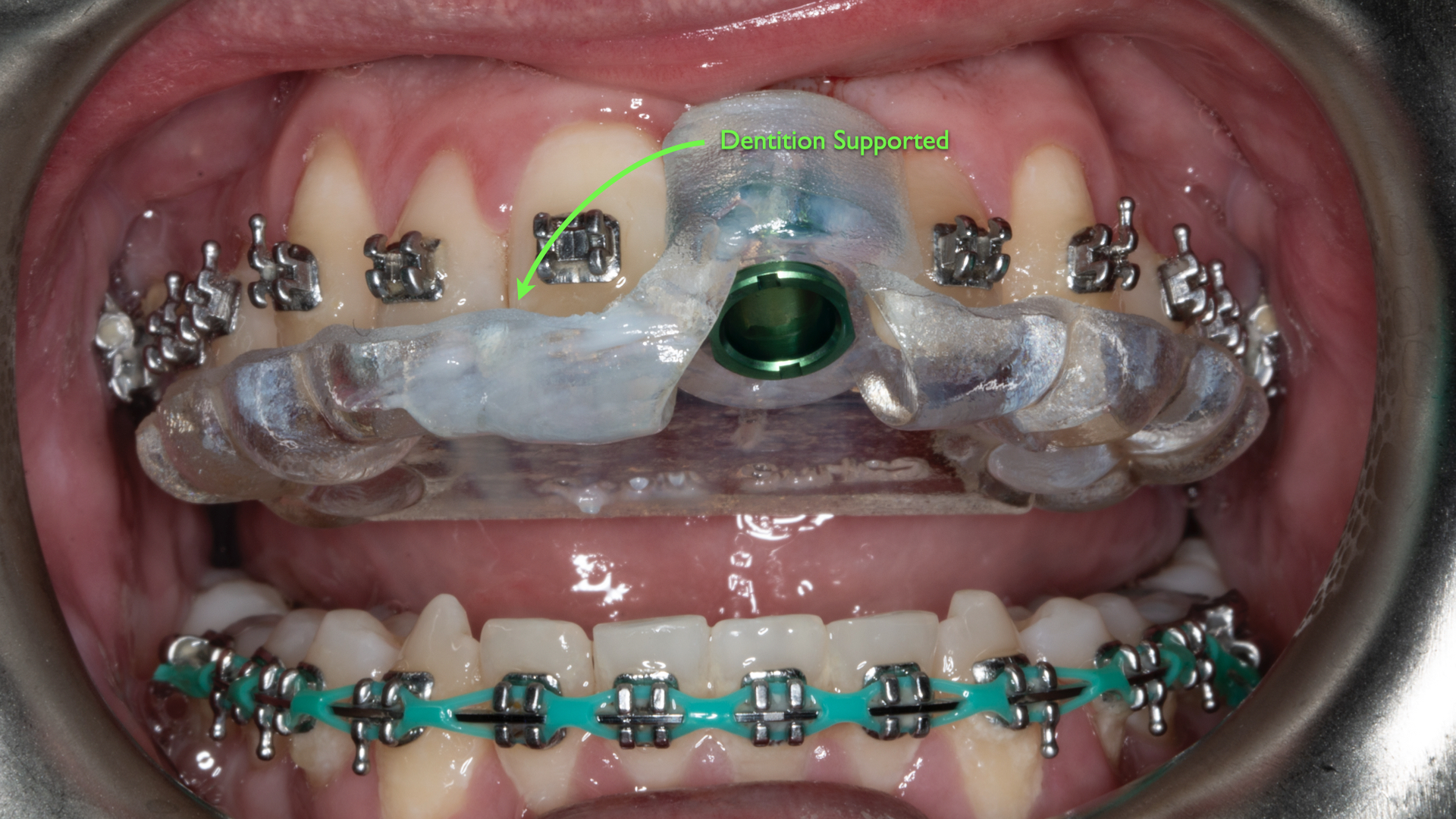
Figure 9. Many dental implant surgical guides are characterized by Reference Frame D (dentition) and their placement onto the patient’s existing and/or remaining dentition.
Electronic Vision Systems
Dental technological advances have ushered in an era of electronic vision system reference frames that incorporate real-time positional feedback based on fiducial markers secured to the patient in combination with sensing cameras (Figure 10).13
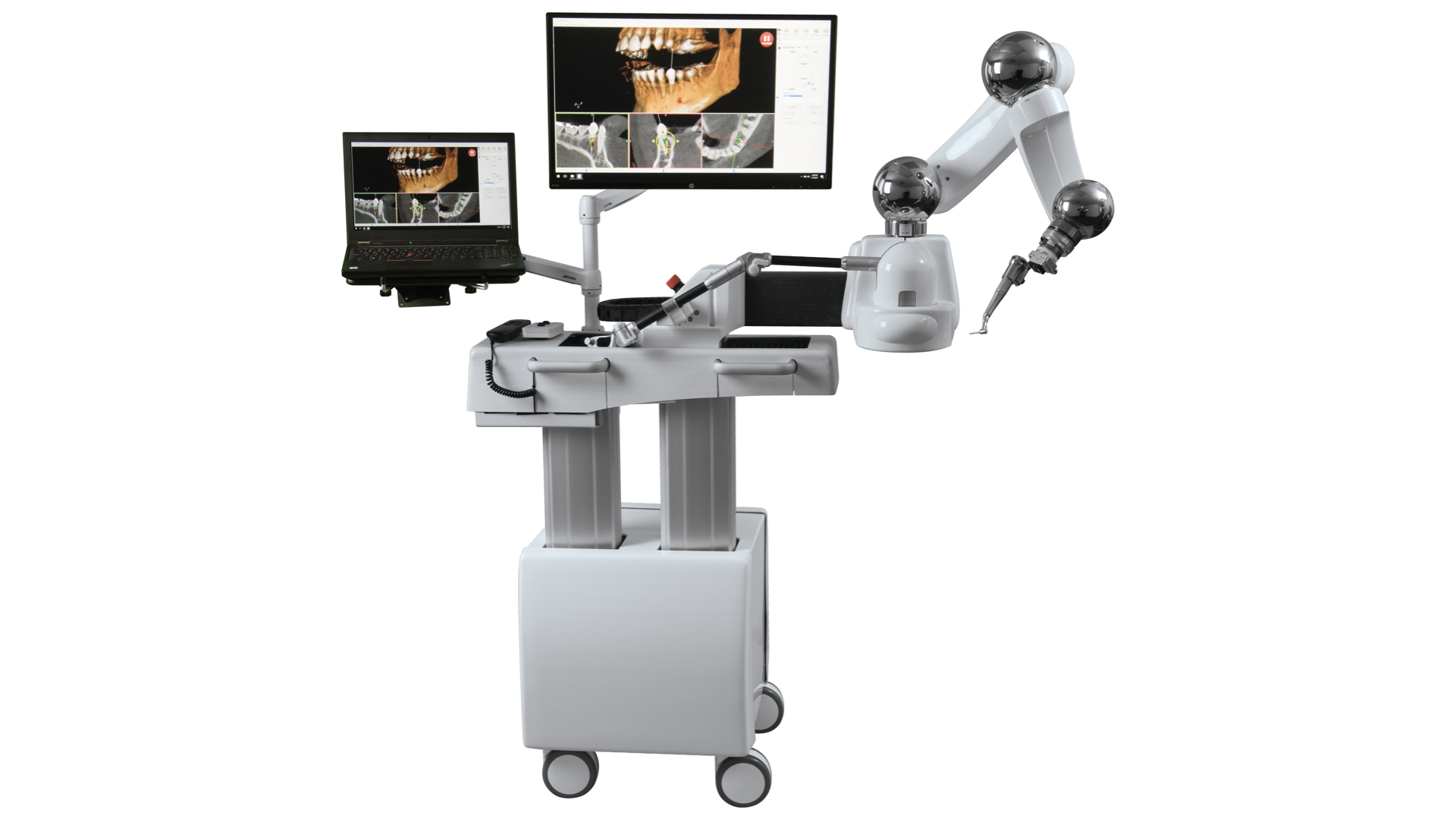
Figure 10. Reference Frame E refers to electronic vision systems that incorporate real-time positional feedback based on fiducial markers secured to the patient, in combination with sensing cameras. Some provide either Type 1 or Type 4 constraints.
These virtually defined reference frames may also carry the classifications of Type 1 (ie, vision only) or Type 4 (ie, fully guided) constraint types.
Type 1 electronic vision systems provide camera navigation without physical constraints on the osteotomy drills or implant driver. However, they provide real-time feedback loops that enable dentists to implement freehand corrections for any positional errors observed (eg, x-Nav, Navident).
Electronic vision systems classified with Type 4 constraints are considered robot-assisted-surgery systems (eg, Yomi, Neocis); these devices utilize a computer control algorithm and associated actuators to physically constrain the osteotomy drills and implant placement in a dynamic setting via a robotic arm. However, robot-assisted cases may also be adjusted in real time by the surgeon by pausing the drilling, refining the desired implant location on the computer, and subsequently resuming the drilling with the new implant location locked into the robot. The robot would immediately comply with the new desired implant location and keep the surgeon on the locked-in target, thereby reducing knockout errors.
Field of View (Doctor’s Eyes)
When only the clinician’s vision is directing implant placement (eg, freehand placement), the reference frame is classified as field of view (Figure 11). The reference frame is predicated only on the doctor’s visual perception.3,10
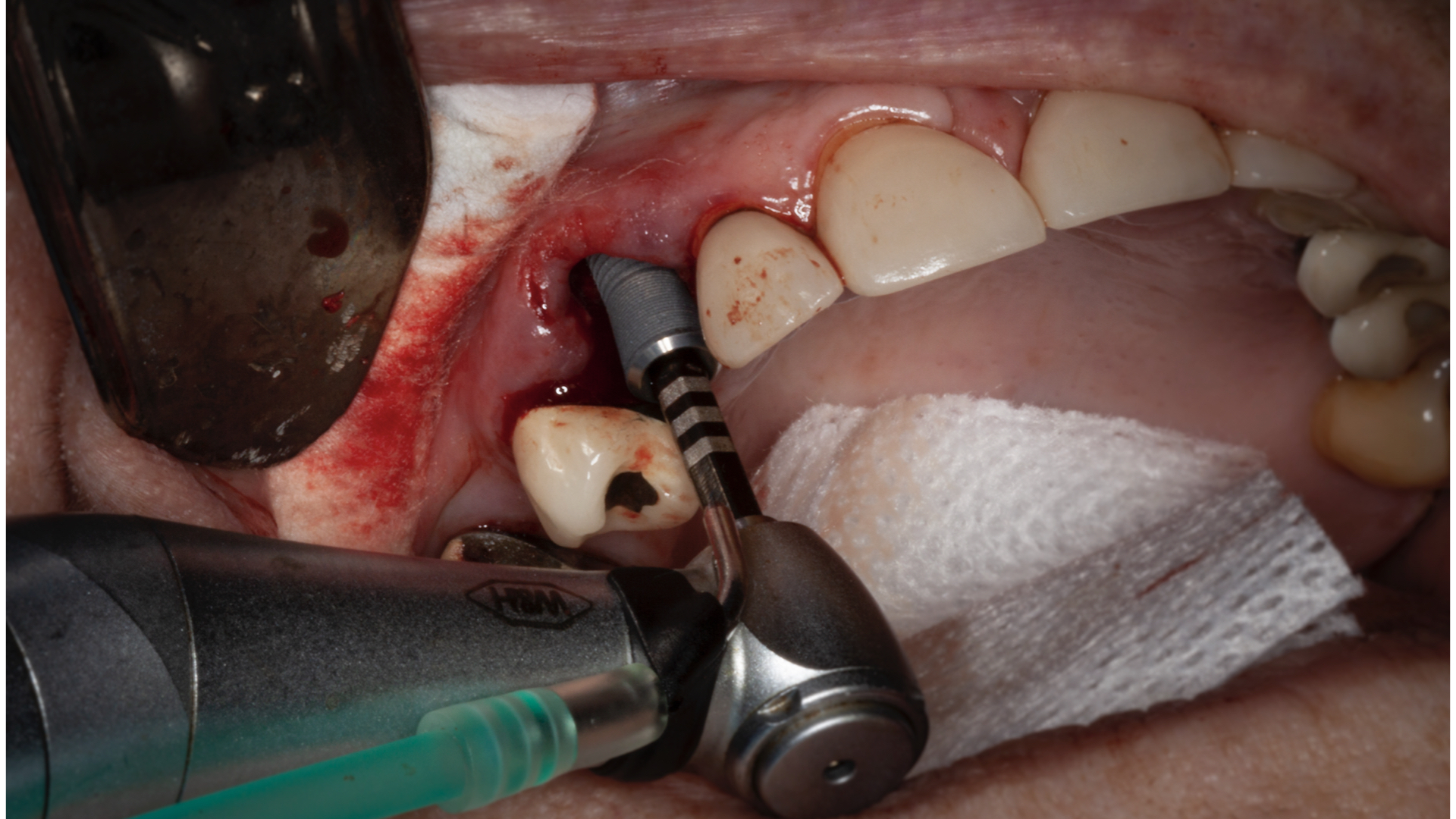
Figure 11. Reference Frame F refers to the doctor’s field of view or freehand placement classification.
Grounded Via Implants (Implant-Supported)
When a dental implant surgical guide is rigidly and accurately secured to previously integrated implants, its reference frame is classified as grounded (Figure 12).
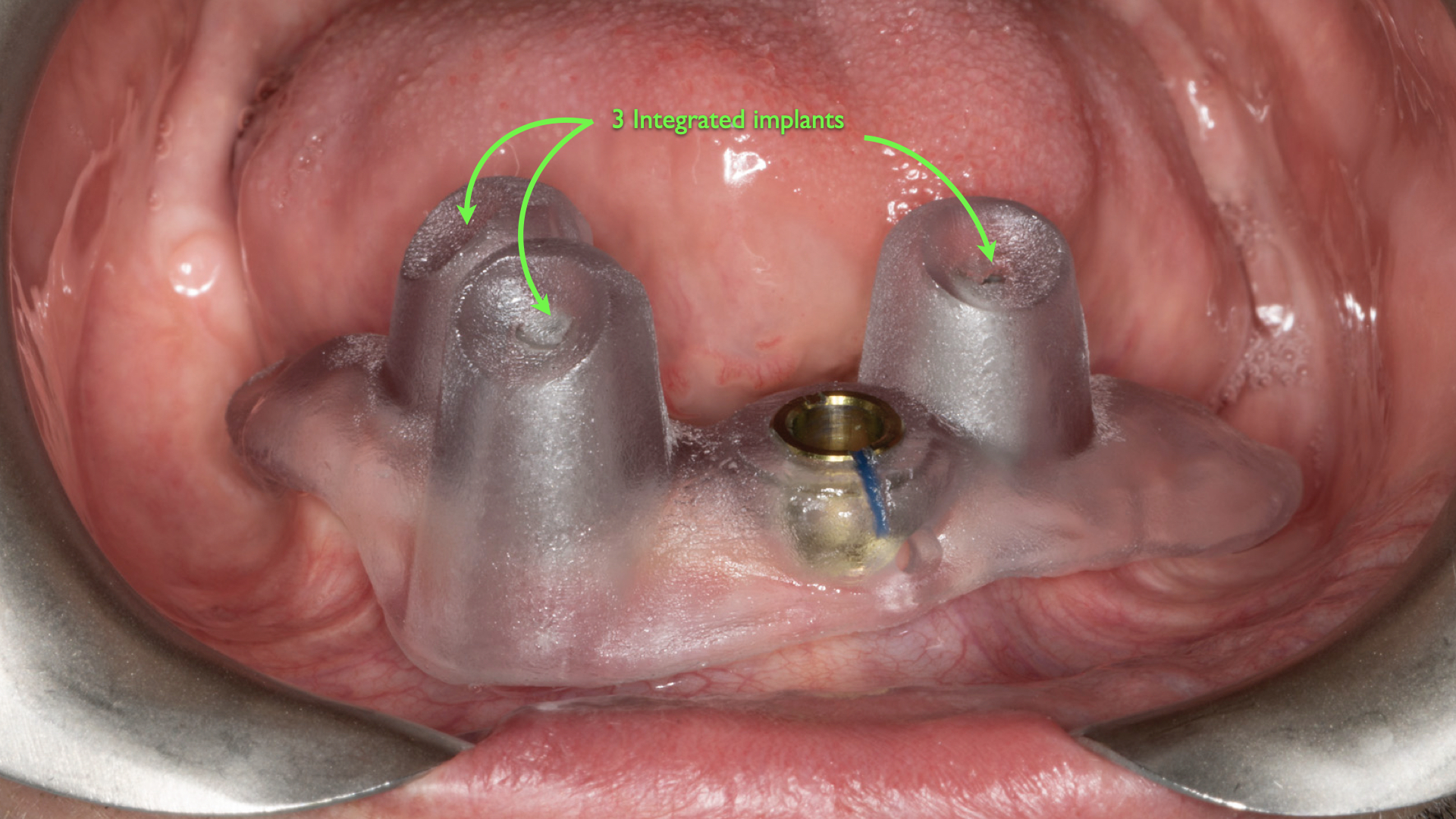
Figure 12. When a dental implant surgical guide is rigidly and accurately secured to existing integrated implants, it is classified as Reference Frame G (grounded).
Timing
The third attribute useful for classifying dental implant surgical guides refers to implant “timing,” otherwise known as an implant’s rotational position. Particularly in prosthodontically driven treatment plans and multi-implant protocols (eg, full-mouth reconstruction with one or more angled, multi-unit abutments or cases requiring off-axis screw channels), an implant’s rotational position must be exact during placement to ensure that the hex flat (or other macrogeometric parameter) is in a specific position or direction.
Aligning an implant’s features with such rotational control is referred to as implant timing.
Some dental implant surgical guides possess the ability to assist the doctor in placing an implant such that a particular implant design feature is oriented in the desired direction (timing). Other guides do not control for rotational position (no timing).
Typically, only Type 1 and most Type 4 guides are currently capable of timing control since other guides are not present in the patient’s mouth during implant placement. Type 4 printed or milled static guides enable timing to be easily accomplished since, during guide fabrication, a timing index line can be marked on the surgical guide (Figure 13).
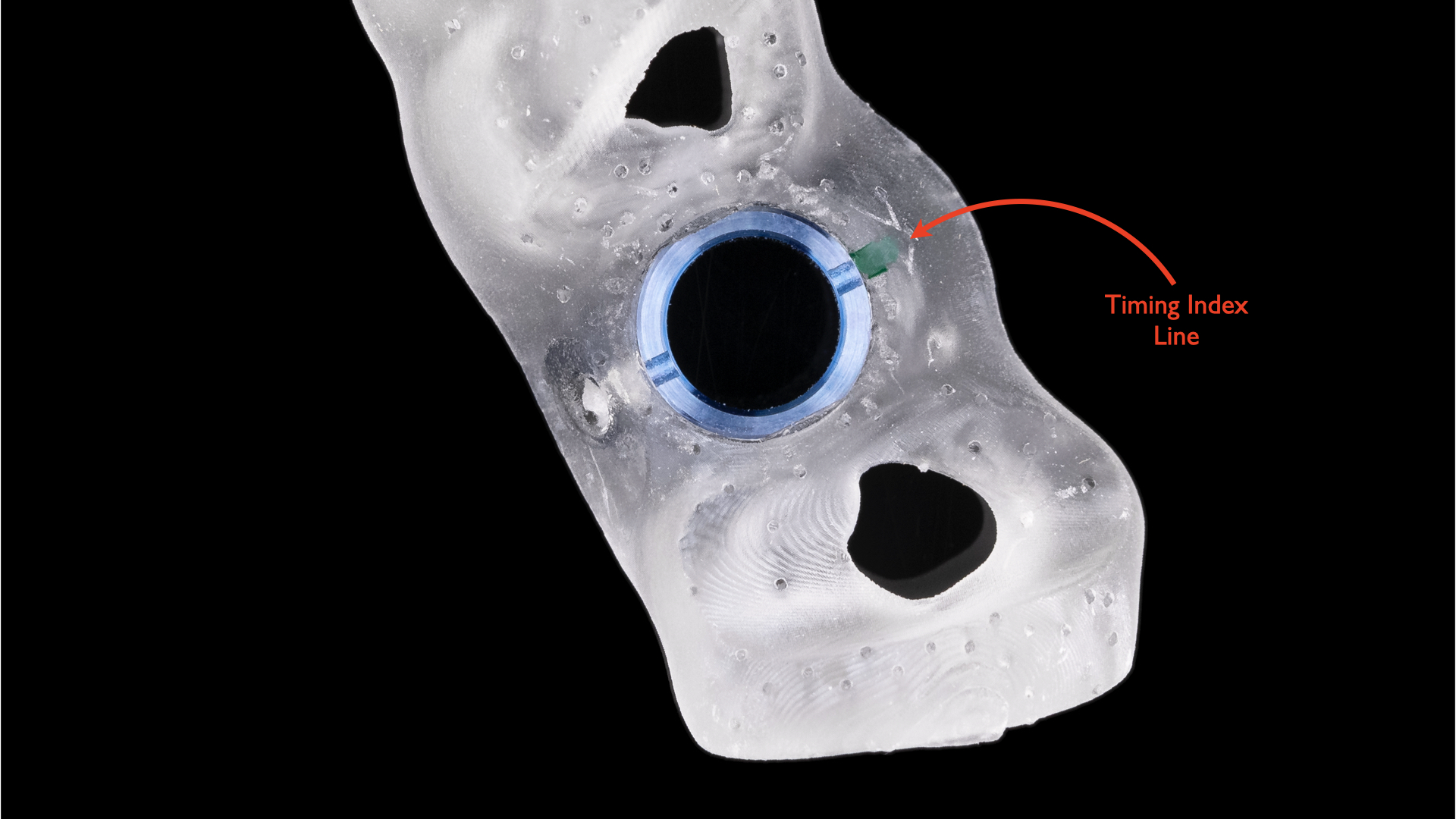
Figure 13. Precise timing, which may be of paramount importance for successful and efficient implementation of presurgical fabricated provisional restorations, can be accomplished with a Type 4 printed or milled static guide with a provided timing index line.
Practical Implications
Based on the attributes described above (eg, physical constraint, reference frame, timing), a classification table has been developed to help clinicians in classifying and selecting from available dental implant surgical guide options (Table 1).
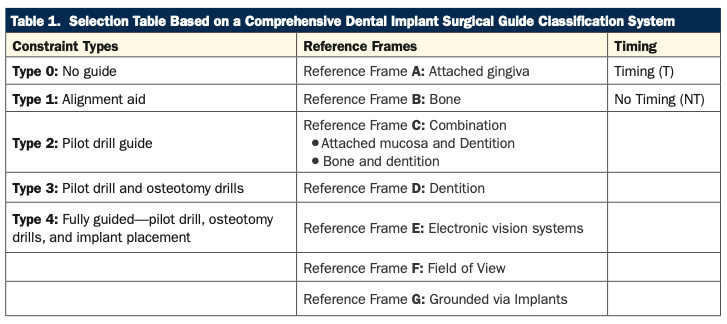
To determine the type of guide that will be best suited for his or her case, the clinician should first determine the one type of constraint he or she will need (ie, Type 0 through Type 4) from the first column. Then the clinician can identify the single reference frame that will be used and/or needed from the second column.
The last guide criteria is timing and is selected from the third column.
For example, a dental implant surgical guide with a Type 4 constraint, dentition reference frame, and timing is commonly incorporated by dentists during implant placement. It is supported by the dentition and completely constrains the implant placement in terms of position, depth, and timing (Figure 5). Alternatively, a freehand implant placement may involve no surgical guide and therefore yield a classification of constraint Type 0, reference frame type field of view, and no timing (Figure 1).
Interestingly, a visual aid surgical guide that provides no constraints and no timing but relies on electronic vision system navigation would be classified as Type 1 constraint, electronic vision reference frame, and no timing (timing is currently not available for electronic systems). In another example, a visual aid surgical guide that incorporates electronic vision system navigation with physical constraints on the drills and implant may be classified as a constraint Type 4, reference frame electronic vision, with no timing (Figure 10).
CONCLUSION
Successful dental implant treatment outcomes are predicated not only on meticulous treatment planning, but also on selecting the right guide for the clinical situation at hand. It is therefore incumbent upon clinicians to select from available dental implant surgical guide options based on their demonstrated success in contributing to predictable and accurate dental implant placement, how they will be used in the context of the patient’s oral anatomical environment, and the type and extent of guidance they provide.
Several authors have classified dental implant placement surgical guides to facilitate their differentiation; evaluation; and, ultimately, selection. However, the classification system and table selection tool proposed herein defines 3 key attributes of dental implant surgical guides (physical constraints, reference frame, and timing) to enhance communication among members of the treatment planning team, advance the standard of implant care, facilitate guide selection, and enable relevant outcome comparisons in future research endeavors.
REFERENCES
1. Geng W, Liu C, Su Y, et al. Accuracy of different types of computer-aided design/computer-aided manufacturing surgical guides for dental implant placement. Int J Clin Exp Med. 2015;8(6):8442–9.
2. D’haese J, Ackhurst J, Wismeijer D, et al. Current state of the art of computer-guided implant surgery. Periodontol 2000. 2017;73(1):121–33. doi:10.1111/prd.12175
3. Umapthy T, Jayam C, Anila BS, et al. Overview of surgical guides for implant therapy. J Dent Implants. 2015;5(1):48-52.
4. D’Souza KM, Aras MA. Types of implant surgical guides in dentistry: a review. J Oral Implantol. 2012;38(5):643–52. doi:10.1563/AAID-JOI-D-11-00018
5. Winkler S, Morris HF. Dental implant research: a perspective. J Oral Implantol. 2009;35(1):3-4. doi:10.1563/1548-1336-35.1.3
6. Kim T, Lee S, Kim GB, et al. Accuracy of a simplified 3D-printed implant surgical guide. J Prosthet Dent. 2020;124(2):195-201.e2. doi:10.1016/j.prosdent.2019.06.006
7. Ozan O, Turkyilmaz I, Ersoy AE, et al. Clinical accuracy of 3 different types of computed tomography-derived stereolithographic surgical guides in implant placement. J Oral Maxillofac Surg. 2009;67(2):394-401. doi:10.1016/j.joms.2008.09.033
8. Sun TM, Lee HE, Lan TH. Comparing accuracy of implant installation with a navigation system (NS), a laboratory guide (LG), NS with LG, and freehand drilling. Int J Environ Res Public Health. 2020;17(6):2107. doi:10.3390/ijerph17062107
9. Abduo J, Lau D. Accuracy of static computer-assisted implant placement in anterior and posterior sites by clinicians new to implant dentistry: in vitro comparison of fully guided, pilot-guided, and freehand protocols. Int J Implant Dent. 2020;6(1):10. doi:10.1186/s40729-020-0205-3
10. Salem D, Mansour MH. Surgical guides for dental implants: a suggested new classification. J Dent Oral Health. 2019;6(104):1-8.
11. Stumpel LJ 3rd. Cast-based guided implant placement: a novel technique. J Prosthet Dent. 2008;100(1):61–9. doi:10.1016/S0022-3913(08)60140-7
12. Bartling WC, Schleyer TK, Visweswaran S. Retrieval and classification of dental research articles. Adv Dent Res. 2003;17:115–20. doi:10.1177/154407370301700126
13. Emery RW, Merritt SA, Lank K, et al. Accuracy of dynamic navigation for dental implant placement-model-based evaluation. J Oral Implantol. 2016;42(5):399-405. doi:10.1563/aaid-joi-D-16-00025
ABOUT THE AUTHOR
Dr. Stanley received his DDS degree from the University of North Carolina at Chapel Hill School of Dentistry. He received his BS, MS, and PhD degrees in engineering with a concentration in control theory from North Carolina State University. He enjoyed almost a decade with a telecommunications company in Research Triangle Park before pursuing his passion of dentistry. He has extensive experience in implant surgery as well as advanced bone and soft-tissue grafting.
He is a Diplomate with the American Board of Oral Implantology and the International College of Oral Implantologists; is certified in oral, IV, and conscious sedation; and is a member of the AGD, the American Academy of Cosmetic Dentistry, the ADA, the Raleigh-Wake Dental Society, the North Carolina Dental Society, the Dental Organization for Conscious Sedation, and the International Association of Comprehensive Aesthetics.
Dr. Stanley frequently consults with dental industry manufacturers, suppliers, and laboratories on product and process creation and improvement.
He can be reached at drrobert@stanleyinstitute.com.
Disclosure: Dr. Stanley reports no disclosures.


