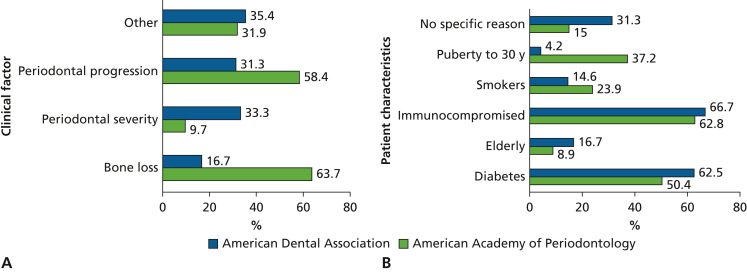
Background
In the absence of a full spectrum of evidence-based guidelines for the appropriate
use of antimicrobial agents, dentists, including periodontists, remain a highly frequent
antibiotic prescribing group. With the goal of understanding antibiotic prescribing
practices, the authors surveyed a convenience sample of dental practitioners and periodontists
to identify differences between the 2 cohorts and assess the factors that affect prescribing
practices.
Methods
An institutional review board–approved 15-item survey was developed to capture antibiotic
prescribing practices addressing the main research question, factors affecting systemic
antibiotic prescription patterns, and prescription timing. The authors collaborated
with the American Dental Association (ADA) and the American Academy of Periodontology
(AAP) for survey dissemination. Responses were summarized using descriptive statistics.
Multivariable models were developed to identify antibiotic prescription predictors.
Results
Overall, 32.4% of the participants prescribed systemic antibiotics with scaling and
root planing. When comparing the 2 groups, the authors found that 46.4% and 18.7%
of the AAP and ADA members, respectively, prescribed systemic antibiotics with scaling
and root planing (P = .0001). The authors found a significant difference between the AAP and ADA groups
in prescription timing (P = .01). The multivariable model revealed that practitioner sex (P = .03), AAP membership (P = .0001), and years of practitioner experience (P = .04) predicted antibiotic prescription practices. The geographic location, practice
setting, and occupation type did not predict antibiotic prescription patterns.
Conclusion
The authors found a lack of clarity related to prescription timing, factors determining
prescription patterns, and selection of patient population who would benefit more
from antibiotics.
Practical Implications
This study confirmed a lack of clarity related to antibiotic prescription patterns
in combination with nonsurgical periodontal treatment.