INTRODUCTION
Ceramics have become the material of choice for indirect restorations, with one of the nation’s largest laboratories reporting that 90% of their indirect restorations were fabricated from ceramic.1 Perhaps one of the more confusing aspects of using ceramic crowns is the decision of whether or not to bond the restoration, followed by the clinical steps involved to either conventionally cement or bond the ceramic restoration. For the purpose of this article, conventional cementation involves the use of a glass ionomer or resin-modified glass ionomer (RMGI) cement, whereas bonding implies the use of a resin cement and ceramic primer.
According to the National Dental Practice-Based Research Network study of nearly 4,000 single-unit crowns, 38% of the crowns were bonded with resin cement, whereas 52% of the crowns were cemented with RMGI cement, and 9% were cemented with conventional glass ionomer cement. In this study, 70% of lithium disilicate, 30% of zirconia, and 14% of PFM crowns were bonded with resin cement, and the remainder were conventionally cemented.2 Although resin cements provide more retention3 and greater strength reinforcement of ceramic crowns4 than RMGI cement, RMGI cements are easier to use, more moisture tolerant, and protective of crown margins.
CHOOSING WHICH CEMENT TO USE
The choice of which cement to use for a ceramic restoration can be simplified into an assessment of the need for additional retention of the preparation or additional reinforcement needed for the restoration. Retention is assessed by axial wall height and taper. Axial wall height, as determined by prosthodontic literature, should be 3 mm for premolars and 4 mm for molars.5 If crowns are shorter, resistance form can also be improved by adding proximal grooves; however, decreasing the taper of the cervical portion of the crown preparation is more effective at improving resistance form.6 Preparation taper also affects resistance form. A taper of 12° is recommended for conventional cementation7 (Figure 1).
Figure 1. (a)
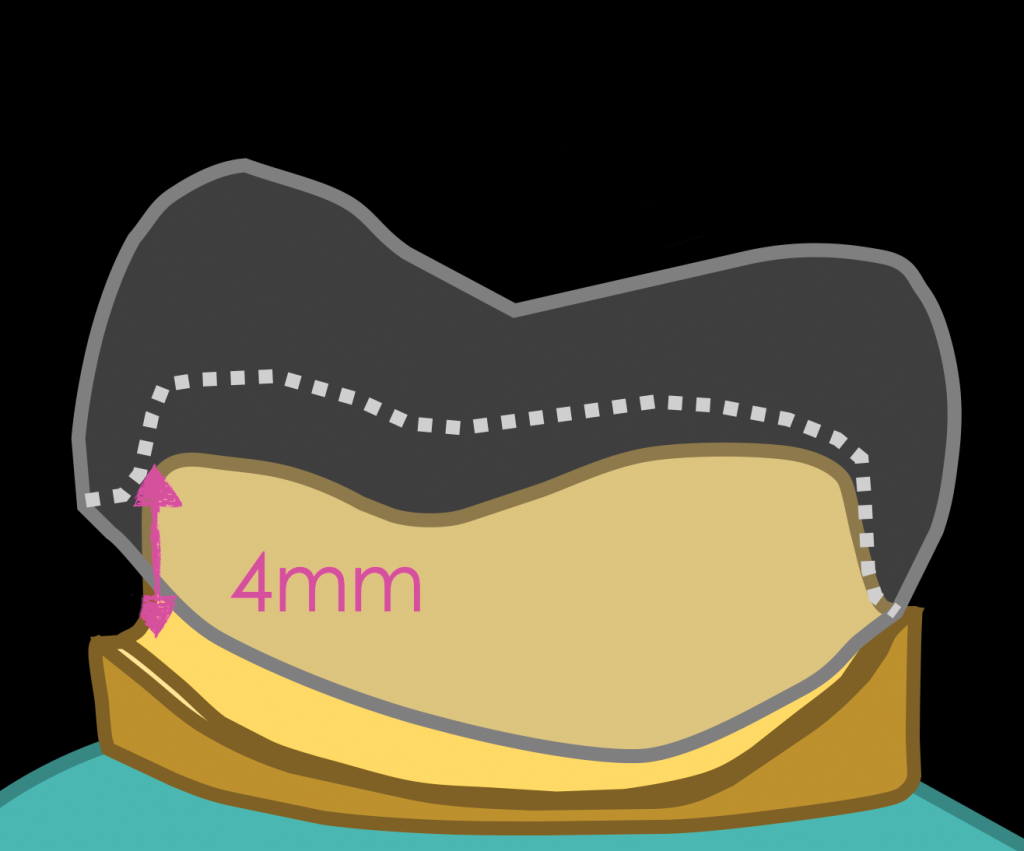
Figure 1. (a) Axial wall height should be 3 mm for premolars and (b) 4 mm for molars.
Ceramic crowns are also bonded in order to improve their strength. In theory, a bonded crown will transfer occlusal forces to the substructure, whereas a conventionally cemented crown will not. The need for strength reinforcement through bonding is dependent on both the strength of the ceramic material and the thickness at which it is used. For materials such as feldspathic porcelain veneers, the ceramic must be bonded to tooth structure in order to survive in the mouth.
For lithium disilicate, manufacturers recommend a minimal restoration thickness of 1 mm if the crown is bonded and 1.5 mm if the crown is cemented with a glass ionomer or an RMGI cement. Recommendations for zirconia are dependent on its composition (3 mol%, 4 mol%, or 5 mol% yttria-containing).
Translucent zirconia (4 mol% or 5 mol% yttria-containing) is weaker than traditional zirconia (3 mol% yttria-containing), which means it will require slightly more restoration thickness.
A recent study suggested a restoration thickness of 1.2 mm for 4 mol% or 5 mol% yttria-containing zirconia, whereas 3 mol% yttria-containing zirconia has been recommended8 to be used between 0.6 mm and 1 mm.
Bonding both translucent and traditional zirconia will improve its strength; however, it is less critical to bond any type of zirconia than it is to bond to lithium disilicate.4
Despite the advantages of resin cements, a limitation is that they must be used in cases in which isolation from saliva and blood is possible. They will also require a more complicated clinical procedure. Therefore, conventional cementation is still very popular. The next section of this article will discuss considerations for RMGI cementation, followed by a discussion of the steps for bonding ceramic crowns with resin cement (Table 1).

CONSIDERATIONS FOR CONVENTIONAL CEMENTATION WITH RMGI OR GLASS IONOMER CEMENT
Ease of Use
RMGI cements are easier to use than resin cements as they are often easier to clean and do not require the additional steps needed for bonding ceramic crowns.
An ADA Clinical Evaluator Panel survey of resin cements reported that 21% of dentists clean some uncured cement, 85% of dentists clean some tack-cured cement, and 28% of dentists clean some fully cured cement.9 If the trend is similar for RMGI cement, it will imply that many clinicians undertake the task of cleaning fully or tack-cured RMGI cement (some brands of RMGI cement are capable of tack curing). RMGI does not bond to tooth structure as strongly as resin cements. Therefore, the cleanup of RMGI cements is easier as the cement does not adhesively bond to the tooth structure below the crown margins or on the adjacent teeth. Also, most RMGI is white opaque and can be visualized easier than resin cement (Figure 2).
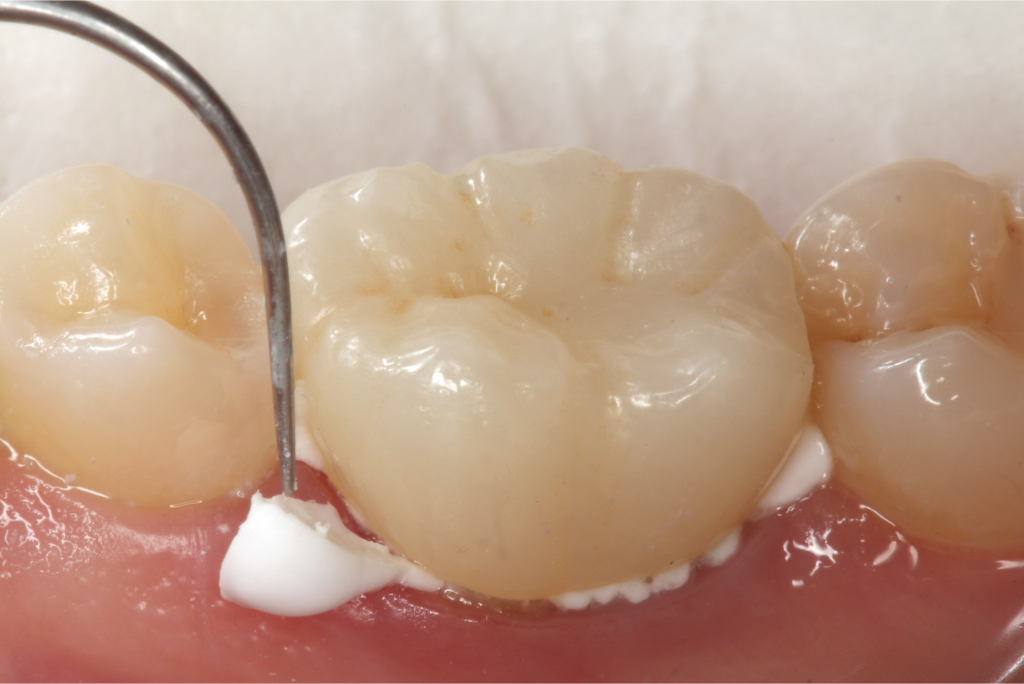
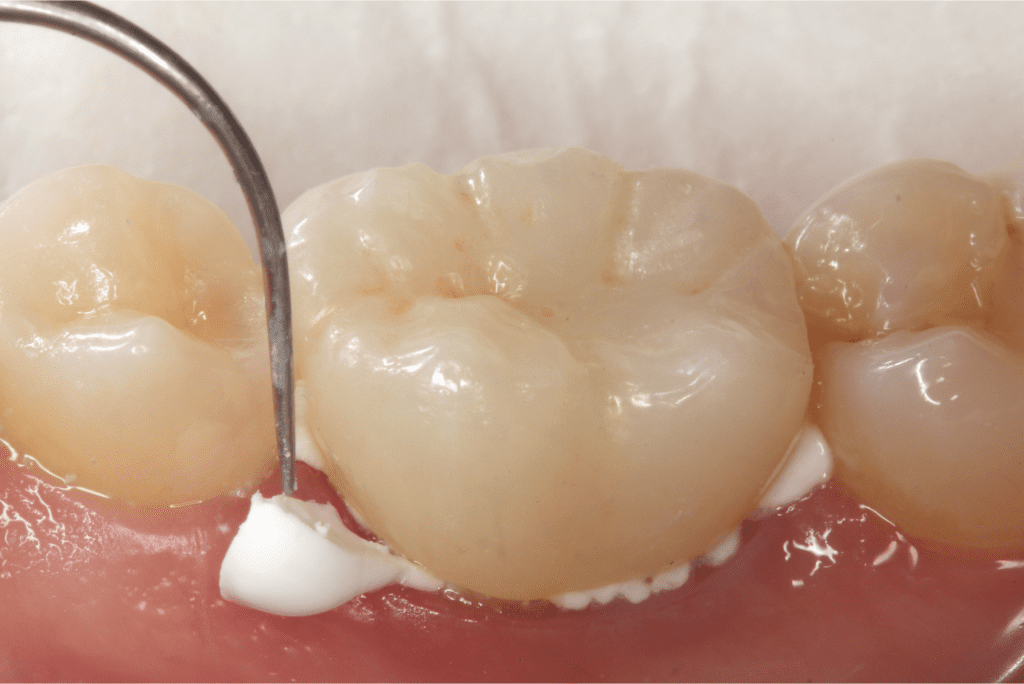
Figure 2. Cementing a zirconia crown with RMGI cement.
Cementation of ceramic crowns with RMGI cement requires fewer steps than bonding ceramic crowns as no primers are required on the ceramic surface. The ceramic primers include those containing silane for chemically bonding to glass-based ceramics and 10-methacryloyloxydecyl dihydrogen phosphate (10-MDP) for bonding to zirconia. These primers chemically link the ceramic surfaces with methacrylate-based resin cements. In the case of RMGI cements, there is no evidence that the RMGI cement chemically bonds with primed ceramic surfaces. In fact, the use of a primer on the surfaces of glass-based or zirconia crowns may actually reduce their bond with RMGI cement. A study performed in our laboratory reported that the application of a silane/10-MDP-containing primer reduced the bond with RMGI to lithium disilicate by 23% and to zirconia by 48%.10 Since there is no evidence of a chemical bond between ceramics and RMGI cements, it does not seem necessary to use a ceramic cleaner to remove salivary contaminants on the inside of ceramic crowns when using RMGI cements. Rinsing the crown with water after try-in is likely sufficient.
Mechanically roughening the intaglio of ceramic crowns, however, does seem to be necessary when cementing ceramic crowns with RMGI cement. In our laboratory study, etching lithium disilicate with hydrofluoric acid improved its bond by 16 times, and sandblasting zirconia with 50-µm alumina particles improved its bond by almost 3 times.11
Moisture Tolerance
The bond of glass ionomer-based materials occurs by an ionic bond of the polyacrylic acid in the glass ionomer and calcium in the tooth. This ionic bond does not provide as high retention to dentin as the hybrid layer that forms between demineralized dentin and cured adhesive resin. For this reason, a higher crown retention is achieved with resin cements than with RMGI cements. The bond between dentin and resin-based materials is significantly affected by the presence of salivary contamination, whereas glass ionomer and RMGI materials are not. In a laboratory study, a glass ionomer, RMGI, and resin composite were bonded to dentin contaminated with dry or wet saliva.12 The bonds with the glass ionomer and RMGI were not affected by saliva’s presence. The bond to the resin composite dropped by about 35% in the presence of dried saliva and 50% in the presence of wet saliva. These findings do not imply that crowns should be cemented with RMGI cement in the presence of saliva; however, if a crown has a subgingival margin or is located in a part of the mouth that is difficult to isolate from saliva, RMGI cement may be a more appropriate choice. As RMGI cements are not as retentive as resin cements, a more retentive crown preparation is advised in these cases of difficult isolation.
Protection of Crown Margins
Crown margins are susceptible to recurrent caries when tooth structure below the crown margins experiences demineralization. In order to help prevent the process of recurrent caries, a cement may release ions present in tooth structure to help counteract the demineralization from acid in plaque. A recent laboratory study examined the protective effect of RMGI cement in an acid-based artificial caries model.13 Extracted human molars were prepared with small restorations at their CEJs that were composed of RMGI or resin cement.
The teeth were then subjected to 30 days of pH cycling to induce demineralization at the surface of the root dentin. The teeth were sectioned, and the demineralization was examined with polarized light microscopy (Figure 3).
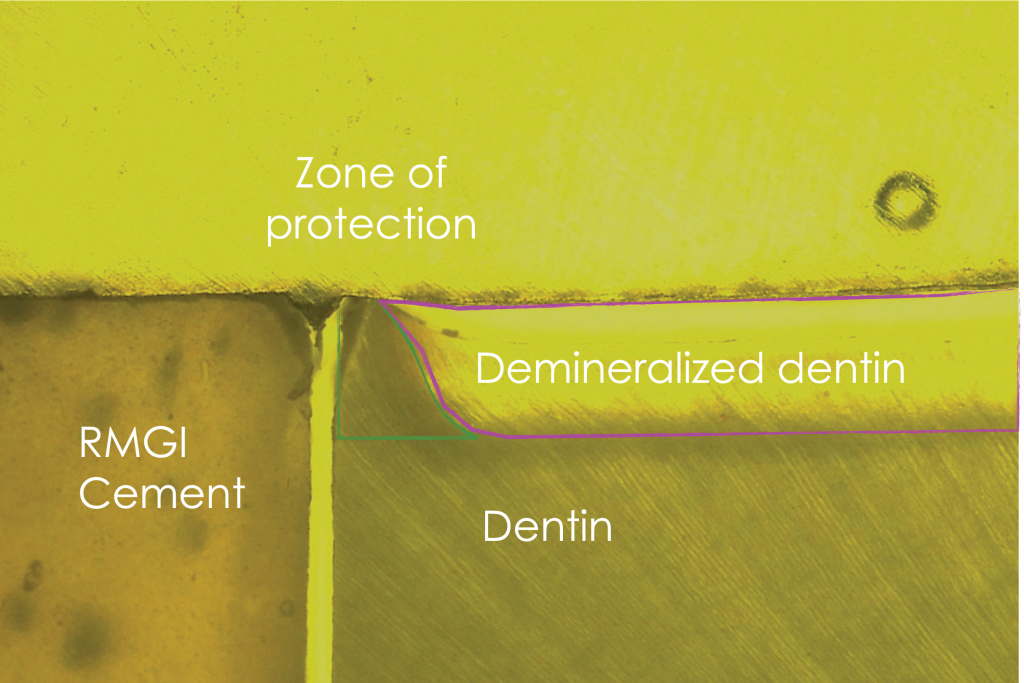
Figure 3. Interface of RMGI cement and root dentin showing a “zone of protection” against acid-induced demineralization provided by RMGI cement.
The root dentin in contact with RMGI cement showed a zone of protection with less demineralization than the surrounding root dentin. The resin cement created “wall lesions” at the interface of the root dentin, which are areas of increased demineralization.
This study suggests that fluoride release from RMGI cements may help prevent demineralization of surrounding dentin.
Methods of Dispensing
RMGI cements can be dispensed in dual-barrel paste/paste syringes or powder/liquid capsules to separate the cements’ 2 chemical-cured components. The cements can either be mixed through hand-mixing or by automixing through a mixing tip or triturated capsule. In a laboratory study that tested the mechanical properties of RMGI materials from the same brand with different mixing techniques, the fracture toughness of the hand-mixed powder/liquid cement was higher than the hand-mixed paste/paste cement, which was greater than the automixed paste/paste cement. There was no significant difference between the mixing/dispensing techniques for compressive strength or diametral tensile strength of the same cements. For another brand of RMGI cement, the compressive strength of powder/liquid automix cement was higher than the paste/paste automix, but there were no differences in the fracture toughness or diametral tensile strength.14 Another laboratory study determined that a powder/liquid version of an RMGI cement provided higher crown retention force than the same cement in a paste/paste form.15 These studies imply a slight improvement in properties with the powder/liquid versions of RMGI cements; however, paste/paste systems are often easier to use.
Disadvantages of RMGI Cements
There are some disadvantages of RMGI cements. They experience more toothbrush wear than resin cements, which become relevant in cases with larger cement gaps.16 RMGI cements show more microleakage than resin cements.17 Additionally, RMGI cements show more water solubility (1.9% to 4.8%) compared to resin cements (0.1% to 1.1%) and more water sorption (14% to 18%) than resin cements (1.8% to 2.7%).18 Water solubility may be detrimental if cement weakens or dissolves at the margin. Water sorption could lead to hygroscopic expansion, putting stress on the internal surface of a crown. Laboratory studies have shown that hydroscopic expansion of an RMGI cement caused cracking of a glass-based ceramic coping19 but not a stronger polycrystalline ceramic coping.20 Resin cements are also preferred over RMGI cements for aesthetic restorations as they may be provided in different shades and translucencies to affect the final color of translucent restorations.
Summary of Glass Ionomer and RMGI Cementation
The use of ceramic primers and cleaners is not indicated for ceramic crowns when using RMGI cements; however, surface roughening should be performed. The retention provided by RMGI cements is less affected by saliva contamination than that of resin cements, and the fluoride release of RMGI cements may help prevent recurrent caries. Powder/liquid and hand-mixed RMGI cements may provide slightly improved properties over paste/paste and automixed cements. Assuming ideal bonding conditions, RMGI cements may be less able to seal the margins of a crown than resin cements, and hygroscopic expansion of RMGI cements may be an issue with weaker glass-based ceramics.
CONSIDERATIONS FOR BONDING WITH RESIN CEMENT
Mechanisms of Bonding
Bonding to any type of restorative material can be achieved by 2 basic mechanisms. First, surface roughening of the ceramic (ie, etching or sandblasting) allows micromechanical retention between the resin cement and the restorative material. Second, a chemical link can be formed between the restorative material and the resin cement through a primer.
An ADA survey reported that 42% of dentists would ask a laboratory to etch glass-based restorations, and 70% will ask the laboratory to sandblast zirconia restorations (and about 10% of dentists don’t know what their laboratories are doing).9 If this surface roughening occurs in the laboratory, a cleaning step must be added after the restoration is tried into the mouth and contaminated with saliva (Table 2).
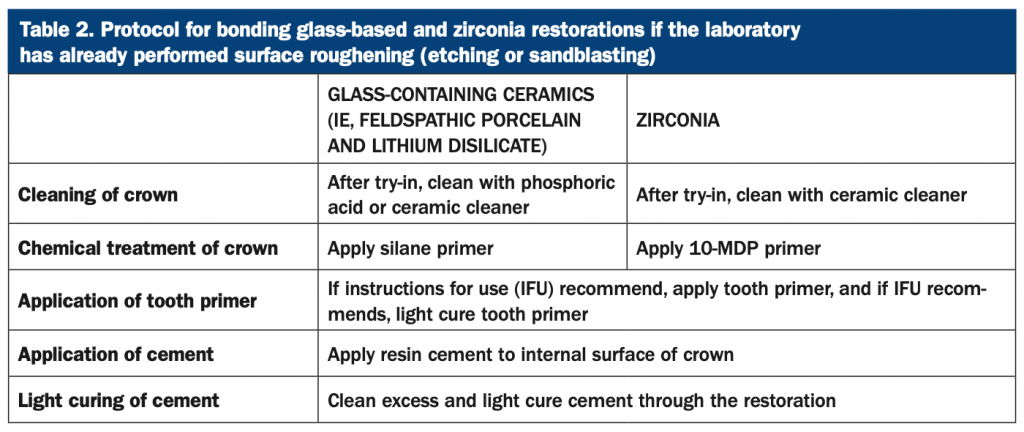

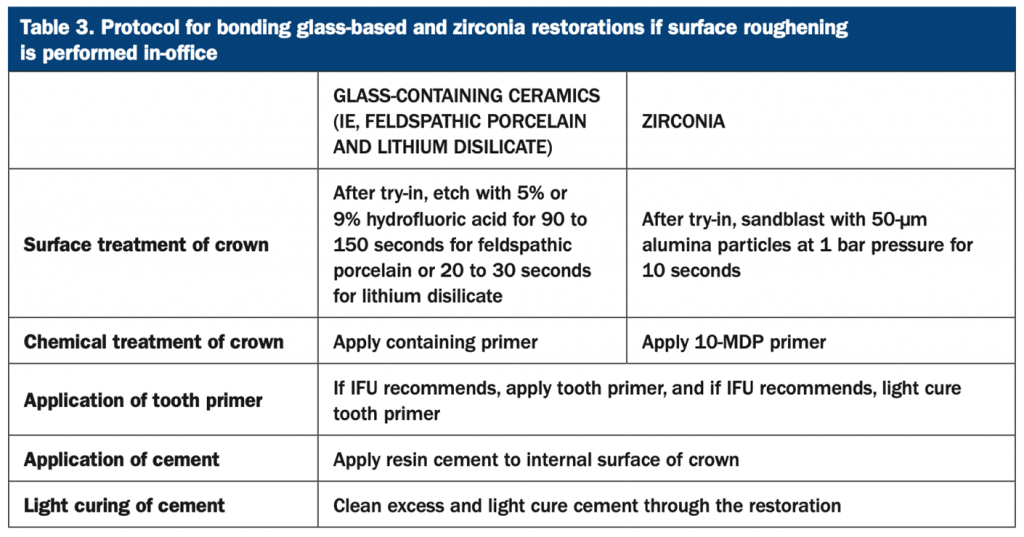
If the clinician chooses to etch or sandblast in his or her own office, then the crowns may be tried in prior to surface roughening to avoid the cleaning step (Table 3).
Alternatively, the primer may be applied in the office or laboratory prior to try-in of the restoration. Application of the primer will make the surface of the restoration resistant to saliva contamination so that any saliva present on the crown after try-in can be rinsed with water.21,22 The basic mechanisms of bonding apply to both glass-based ceramics (ie, feldspathic porcelain and lithium disilicate) as well as zirconia; however, the steps to achieve these goals are completely different for both materials (Tables 2 and 3).
Bonding Glass-Based Ceramics
In order to bond to glass-containing ceramics such as feldspathic porcelain or lithium disilicate, surface roughening is done by removing some of the glass with hydrofluoric acid. Generally, most manufacturers recommend etching feldspathic porcelain between 90 to 150 seconds with around 10% hydrofluoric acid and etching lithium disilicate with 5% hydrofluoric acid for 20 to 30 seconds.23 Scanning electron microscopy reveals that the etching time of lithium disilicate has a greater impact on its etch pattern than the etchant concentration (Figures 4 to 6).

Figure 4. Lithium disilicate after etching for the manufacturer’s recommended time (20 seconds) and with its recommended etchant (5% hydrofluoric acid).

Figure 5. Lithium disilicate after etching for 20 seconds with 9.5% hydrofluoric acid demonstrates a similar etch pattern as 5% hydrofluoric acid.

Figure 6. Lithium disilicate after etching for 60 seconds with 5% hydrofluoric acid exposes more of the crystalline phase, leading to a deeper etch pattern.
After etching, saliva can be removed from porcelain or lithium disilicate with a cleaning solution (ie, Ivoclean [Ivoclar Vivadent], ZirClean [BISCO Dental Products], and Katana Cleaner [Kuraray America]) or phosphoric acid.22 A chemical bond is formed with porcelain and lithium disilicate by using a silane-containing primer.
These primers may be 2-bottle (longer shelf life) or one-bottle (more convenient) options.
Bonding Zirconia
As zirconia does not contain glass, surface roughness must be achieved by sandblasting (Figure 7).

Figure 7. Zirconia after sandblasting with 50-µm alumina at 1 bar pressure demonstrates surface roughness.
A recent study examined the effect of sandblasting pressure on the bond strength and flexural strength of both 3 mol% and 5 mol% yttria-containing zirconia. Without sandblasting, the bond to the zirconia dropped significantly; however, pressures over 1 bar (15 psi) did not increase the bond. Although the strength of 3 mol% yttria-containing zirconia was not negatively affected by any sandblasting pressure, the strength of 5 mol% yttria-containing zirconia decreased with higher pressures.24 Therefore, a sandblasting pressure of around 1 bar (15 psi) is recommended for any type of zirconia. A general recommendation is to use 50-µm alumina particles at 1 bar pressure for 10 seconds from a distance of 10 mm.
Zirconia, unlike glass-based ceramics, cannot have saliva cleaned with phosphoric acid as the phosphate contaminants will prevent it from bonding. Therefore, saliva must be cleaned from zirconia by either re-sandblasting or with the use of ceramic cleaners (ie, Ivoclean, ZirClean, and Katana Cleaner).22 Once the surface is cleaned, a chemical bond to zirconia may be achieved with a primer containing the molecule 10-MDP. It (or a functionally similar molecule) may be found in some universal adhesives (ie, Scotchbond Universal [3M], All-Bond Universal [BISCO Dental Products], and Adhese Universal [Ivoclar Vivadent]), in zirconia-specific primers (ie, Z-PRIME Plus [BISCO Dental Products]), or general ceramic primers (ie, Monobond Plus [Ivoclar Vivadent] and CLEARFIL CERAMIC PRIMER [Kuraray America]).
Cement Selection
Finally, a resin cement must be selected in order to bond the restoration. Broadly, resin cements are categorized as those that are used with a primer on the tooth and as self-adhesive resin cements, which are used without a tooth primer. An ADA survey reported that most dentists used resin cements associated with a tooth primer for ceramic restorations.9 The advantage of using a resin cement with a tooth primer is higher retention; however, this must be balanced with the extra amount of time required for isolation if using this step.
Light Curing
The choice to light cure the primer/adhesive on the tooth or the resin cement through the ceramic crown necessitates further discussion. Light curing of the primer/adhesive on the tooth is required for some cement systems and is either optional or unecessary for others. Laboratory data indicates that light curing an adhesive on the tooth prior to seating the crown significantly improves the bond strength.25 The clinician must weigh this benefit against the possibility of creating a layer of cured adhesive that prevents completing the seating of the restoration. Many clinicians will light cure their dual-cure resin cement through lithium disilicate restorations. Laboratory data reports that light curing through 3Y zirconia is also possible. As irradiance decreases significantly with darker shades and thicker restorations,16 the author recommends light curing through A1- or B1-shade zirconia up to a 1.5-mm thickness, whereas darker shades only benefited up to a 0.5-mm thickness.26
IN SUMMARY
The protocol for bonding glass-based ceramics is to etch the ceramic with hydrofluoric acid, clean any saliva with phosphoric acid or a ceramic cleaner, and apply a silane primer. Bonding a zirconia restoration is accomplished by sandblasting the internal surface with 50-µm alumina particles, cleaning with a ceramic cleaner, and applying a 10-MDP primer. The cleaning step may be avoided if the clinician tries in the crown prior to performing surface roughening (etching glass ceramics or sandblasting zirconia). The cleaning step may be simplified if the clinician applies ceramic primer prior to try-in as this will eliminate the need for a ceramic cleaner. Once the ceramic is prepared, the clinician may choose a resin cement (used with adhesive or self-adhesive) based on the need for retention and the available time for which isolation is possible.
REFERENCES
1. Christensen GJ. Which crown types are best for which situations? Dent Econ. 2022;112(2):61–4.
2. Lawson NC, Litaker MS, Ferracane JL, et al; National Dental Practice-Based Research Network Collaborative Group. Choice of cement for single-unit crowns: Findings from The National Dental Practice-Based Research Network. J Am Dent Assoc. 2019;150(6):522–30. doi:10.1016/j.adaj.2019.01.021
3. Turker SB, Ozcan M, Mandali G, et al. Bond strength and stability of 3 luting systems on a zirconia-dentin complex. Gen Dent. 2013;61(7):e10-3.
4. Lawson NC, Jurado CA, Huang CT, et al. Effect of surface treatment and cement on fracture load of traditional zirconia (3Y), translucent zirconia (5Y), and lithium disilicate crowns. J Prosthodont. 2019;28(6):659–65. doi:10.1111/jopr.13088
5. Weed RM, Baez RJ. A method for determining adequate resistance form of complete cast crown preparations. J Prosthet Dent. 1984;52(3):330–4. doi:10.1016/0022-3913(84)90437-2
6. Roudsari RV, Satterthwaite JD. The influence of auxiliary features on the resistance form of short molars prepared for complete cast crowns. J Prosthet Dent. 2011;106(5):305–9. doi:10.1016/S0022-3913(11)60135-2
7. Cameron SM, Morris WJ, Keesee SM, et al. The effect of preparation taper on the retention of cemented cast crowns under lateral fatigue loading. J Prosthet Dent. 2006;95(6):456–61. doi:10.1016/j.prosdent.2006.03.021
8. Abdulmajeed A, Sulaiman T, Abdulmajeed A, et al. Fracture load of different zirconia types: a mastication simulation study. J Prosthodont. 2020;29(9):787–91. doi:10.1111/jopr.13242
9. Lawson NC, Khajotia S, Bedran-Russo AK, et al; Council on Scientific Affairs. Bonding crowns and bridges with resin cement: An American Dental Association Clinical Evaluators Panel survey. J Am Dent Assoc. 2020;151(10):796-797.e2. doi:10.1016/j.adaj.2020.07.023
10. Mantri C, Shah K, Nizami B, et al. Effect of primer on bonding of RMGI cement to ceramics. J Dent Res. 2022;101:A0730.
11. Sayed A, Mantri C, Shah K, et al. Bond Strength of RMGI Cements to Ceramics with Different Surface Treatment. J Dent Res. 2022;101:A0101.
12. Shimazu K, Karibe H, Oguchi R, et al. Influence of artificial saliva contamination on adhesion in class V restorations. Dent Mater J. 2020;39(3):429–34. doi:10.4012/dmj.2019-032
13. Huang CT, Blatz MB, Arce C, et al. Inhibition of root dentin demineralization by ion releasing cements. J Esthet Restor Dent. 2020;32(8):791–6. doi:10.1111/jerd.12645
14. Sulaiman TA, Abdulmajeed AA, Altitinchi A, et al. Physical properties, film thickness, and bond strengths of resin-modified glass ionomer cements according to their delivery method. J Prosthodont. 2019;28(1):85-90. doi:10.1111/jopr.12779
15. Johnson GH, Lepe X, Zhang H, et al. Retention of metal-ceramic crowns with contemporary dental cements. J Am Dent Assoc. 2009;140(9):1125–36. doi:10.14219/jada.archive.2009.0340
16. Suzuki S, Minami H. Evaluation of toothbrush and generalized wear of luting materials. Am J Dent. 2005 Oct;18(5):311–7.
17. Chang B, Goldstein R, Lin CP, et al. Microleakage around zirconia crown margins after ultrasonic scaling with self-adhesive resin or resin modified glass ionomer cement. J Esthet Restor Dent. 2018;30(1):73-80. doi:10.1111/jerd.12348
18. Labban N, AlSheikh R, Lund M, et al. Evaluation of the water sorption and solubility behavior of different polymeric luting materials. Polymers (Basel). 2021;13(17):2851. doi:10.3390/polym13172851
19. Sindel J, Frankenberger R, Krämer N, et al. Crack formation of all-ceramic crowns dependent on different core build-up and luting materials. J Dent. 1999;27(3):175–81. doi:10.1016/s0300-5712(98)00049-9
20. Snyder MD, Lang BR, Razzoog ME. The efficacy of luting all-ceramic crowns with resin-modified glass ionomer cement. J Am Dent Assoc. 2003;134(5):609–12. doi:10.14219/jada.archive.2003.0228
21. Angkasith P, Burgess JO, Bottino MC, et al. Cleaning methods for zirconia following salivary contamination. J Prosthodont. 2016;25(5):375–9. doi:10.1111/jopr.12441
22. Yoshida K. Influence of cleaning methods on the bond strength of resin cement to saliva-contaminated lithium disilicate ceramic. Clin Oral Investig. 2020;24(6):2091–7. doi:10.1007/s00784-019-03074-w
23. Alex G. Preparing porcelain surfaces for optimal bonding. Compend Contin Educ Dent. 2008;29(6):324–35.
24. Fu C, Darkoue Y, Burgess JO, et al. Surface treatment- shear-bond strength and biaxial flexural strength of zirconia. J Dent Res. 2019;98:A3619.
25. Lührs AK, Pongprueksa P, De Munck J, et al. Curing mode affects bond strength of adhesively luted composite CAD/CAM restorations to dentin. Dent Mater. 2014;30(3):281–91. doi:10.1016/j.dental.2013.11.016
26. Ilie N, Stawarczyk B. Quantification of the amount of light passing through zirconia: the effect of material shade, thickness, and curing conditions. J Dent. 2014;42(6):684–90. doi:10.1016/j.jdent.2014.03.007
ABOUT THE AUTHORS
Dr. Lawson is the director of the division of biomaterials and program director of the biomaterials residency program at the University of Alabama at Birmingham (UAB) School of Dentistry. He can be reached at nlawson@uab.edu.
Disclosure: Dr. Lawson has received research grants and/or speaking honoraria from 3M, Ivoclar Vivadent, Kuraray, Dentsply Sirona, and BISCO Dental Products, but did not receive any support for writing this article.
Dr. Ahmed is a second-year resident in the biomaterials program at the UAB School of Dentistry. He can be reached at amsayeda@uab.edu.
Disclosure: Dr. Ahmed reports no disclosures.