Imogen Wood looks at how the current COVID-19 pandemic might impact the practice of dentistry when lockdown finishes.
In the early weeks of the COVID-19 outbreak hitting the UK, dental practices continued to run ‘as normal’. Dental professionals all awaited further guidance from governing bodies. Working in such close proximity to our patients and with regular exposure to saliva and aerosols, many clinicians felt understandably anxious about continuing to practise.
Dentistry.co.uk reported that dental jobs filled 80% of the highest risk jobs during the pandemic. Dental hygienists fell into the highest risk position. This was followed by GDPs, with nurses and dental laboratory technicians filling two more positions. Dental hygienists scored an alarming 100/100 for risk of exposure to infectious diseases.
With more news emerging about non-symptomatic COVID-19 patients each day, as a self-employed clinician, I found myself in the dilemma of whether to continue to work and keep earning or to hang up my scrubs in an effort to minimise the spread of the virus, and reduce the risk to myself. I am sure I was not alone in this. It came as a relief to me, therefore, when we received official guidance to stop all non-urgent treatment.
It has been suggested that without an effective vaccine, this virus could return each year like a seasonal flu. In addition to this, we must consider that a vaccine will only be effective if the virus does not mutate to a point at which the inoculation is no longer effective. This would also mean that people who had developed immunity through exposure to the virus would still be at risk of contracting any new strain of the disease. On the other hand, we cannot stop working forever. We watch closely as China has begun to end its lockdown and reopen its borders in the hope that we too, will soon be able to return to ‘normal’ and go back to work.
COVID-19 changes
I find myself wondering how the global pandemic will affect the future of dentistry. The virus has highlighted a number of ‘weak-points’ in our practice with respect to viral spread. Will it require us to make temporary or perhaps even permanent changes to our clinical practice to address these when we return to work?
PPE has been front-page news everyday during the pandemic. Surgical masks provide adequate protection against large droplets, splashes and contact transmission. But it has now been widely agreed that they have limited use against viruses including COVID-19. This is because surgical masks cannot effectively remove submicrometer-sized aerosol particles, such as aerosolised blood borne pathogens and aerosolised influenza (Chen and Willeke, 1992; Makison et al, 2013). There are many pathogens that can become airborne such as TB, measles and Hepatitis B, but we can vaccinate against all these. This is not the case, however, with viruses like Ebola, SARS, MERS-CoV and COVID-19 (Tellier et al, 2019).
Minimising aerosol contamination
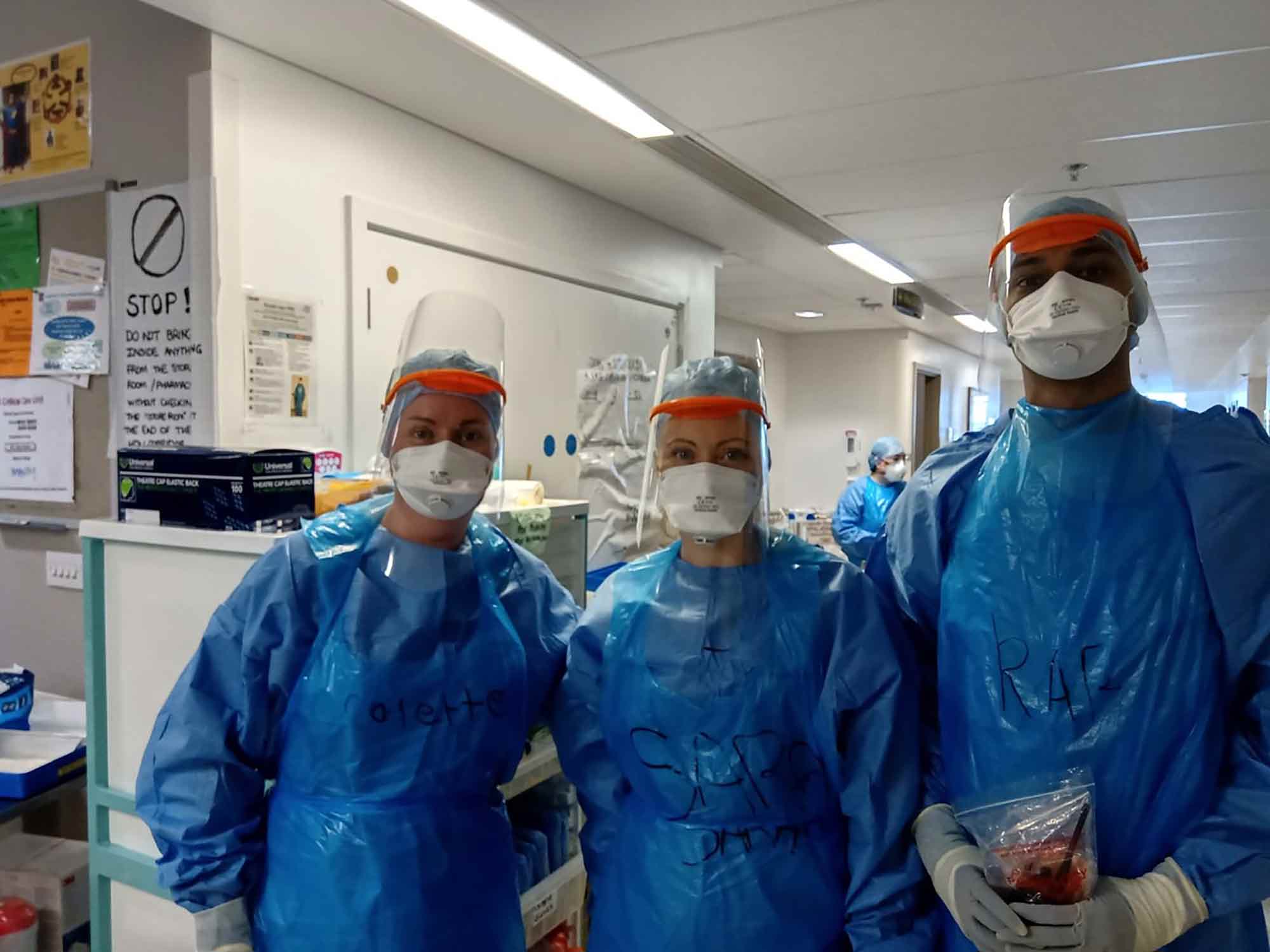
Aerosol use makes up a huge part of the working practice of both the dentist and hygienist. With this in mind, is it likely that we will be required to wear N95 or FFP3 masks when we return to working with aerosols?
The current PPE guidance includes use of FFP3 masks when performing aerosol generating procedures (AGPs) as well as long sleeves gowns, aprons, disposable visors and hairnets. Is it possible that we would need to use this full PPE when we return and, if so, how long for?
Wearing this equipment is hot, uncomfortable and costly. The FFP3 masks cost around £8 each (or much more during a shortage!) in comparison to just a few pence for the masks currently used. Some masks are reusable but reuse may not be practical. Wearing these masks for a prolonged period is not workable. Staff need to take breaks and perform other tasks in the practice, so will need to remove them frequently. In the process of touching the masks we risk spreading the virus particles on them.
The masks will also naturally impair our ability to communicate with patients, a vital part of our jobs. I use my Oral-B Test Drive unit every day to demonstrate brushing technique in a patient’s mouth. How can I do this with enhanced PPE?
We must also consider how they will affect vision, especially when combined with prescription glasses or loupes.
Sustainability
There are of course other, more sustainable, ways in which we can minimise aerosols. The use of chlorhexidine 0.2% rinse prior to starting AGPs is shown to significantly reduce the aerosol contamination, especially when you combine this with the use of high volume aspiration. Suction with a powerful spray mist suction system is the only way to reduce aerosol. Only a spray mist suction system with a suction volume of approximate 300 l/min is able to reduce aerosol (Barnes, Harrel and Rivera-Hidalgo, 1998). Suction manufacturer, Durr Dental, has also advised that we should also always work with a large suction tip. A saliva ejector or a suction tip with a small diameter reduces the suction volume. Four-handed dentistry is therefore essential, as the dental nurse will need to focus on suction technique.
Will this virus be the push that we need to make nursing support obligatory for all clinicians working with aerosols? As a solo working hygienist, I certainly hope so. We may also be able to look deeper into the airflow of our surgeries such as positioning of windows, doors, air conditioning systems and vents.
Patients return
On the matter of patients returning, I can see two potential responses. There will be some, to whom dental health has always been important. They will be desperate to return for their ongoing periodontal care. I fear, however, that many will continue to postpone their visits beyond the end of the lockdown. Either due to economic effects of being out of work or in fear of heading back out to public areas. I believe our return to work will happen, but that we are many many months away from full diaries. This time at home is of course hard, but it is also precious. It brings us time to reflect on our practices. Time to learn and of course to enjoy our families and homes.
I want to finish by thanking everyone for playing their role in the recovery from this challenging time. Many members of the dental team are redeploying in other areas. Or they have volunteered to work in hospitals and others continue to offer emergency dental care. For many of us our role has been helping our communities locally and saving lives by staying at home. We are in this together.
References
Barnes JB, Harrel SK and Rivera-Hidalgo F (1998) Blood contamination of the aerosols produced by in vivo use of ultrasonic scalers. J Periodontol 69(4): 434-8
Chen C and Willeke K (1992) Aerosol penetration through surgical masks. American Journal of infection Control 20 (4): 177-84
Makison C, Clayton M, Crook B and Gawn JM (2013) Effectiveness of surgical masks against influenza bioaerosols. J Hosp Infect 84(1): 22-6
Tellier R, Li Y, Cowling BJ and Tang JW (2019) Recognition of Aerosol transmission of infectious agents: a commentary. BMC Infect Dis 19(1): 101


