Abstract
Background
In 2020, the Centers for Disease Control and Prevention and the America Dental Association released COVID-19 infection control interim guidance for US dentists, advising the use of optimal personal protection equipment during aerosol-generating procedures. The aim of this longitudinal study was to determine the cumulative prevalence and incidence rates of COVID-19 among dentists and to assess their level of engagement in specific infection control practices.
Methods
US dentists were invited to participate in a monthly web-based survey from June through November 2020. Approximately one-third of initial respondents (n = 785) participated in all 6 surveys, and they were asked about COVID-19 testing received, symptoms experienced, and infection prevention procedures followed in their primary practice.
Results
Over a 6-month period, the cumulative COVID-19 infection prevalence rate was 2.6%, representing 57 dentists who ever received a diagnosis of COVID-19. The incidence rates ranged from 0.2% through 1.1% each month. The proportion of dentists tested for COVID-19 increased over time, as did the rate of dentists performing aerosol-generating procedures. Enhanced infection prevention and control strategies in the dental practice were reported by nearly every participant monthly, and rates of personal protection equipment optimization, such as changing masks after each patient, dropped over time.
Conclusions
US dentists continue to show a high level of adherence to enhanced infection control procedures in response to the ongoing pandemic, resulting in low rates of cumulative prevalence of COVID-19. Dentists are showing adherence to a strict protocol for enhanced infection control, which should help protect their patients, their dental team members, and themselves.
Practical Implications
COVID-19 infections among practicing dentists will likely remain low if dentists continue to adhere to guidance.
Key Words
Abbreviation Key:
ADA (American Dental Association), AGP (Aerosol-generating procedure), CDC (Centers for Disease Control and Prevention), HCP (Health care provider), PPE (Personal protective equipment), SARs-CoV-2 (Severe acute respiratory syndrome coronavirus 2)
- Sommerstein R.
- Fux C.A.
- Vuichard-Gysin
- et al.
The scientific community has established that transmission of COVID-19 is linked to aerosol-generating procedures (AGPs) and that the total viral load to which the health care providers (HCPs) are exposed is the main risk factor for infection.
- Bianco F.
- Incollingo P.
- Grossi U.
- Gallo G.
Therefore, both the Centers for Disease Control and Prevention (CDC) and World Health Organization have issued statements specific to AGPs and the need for the use of enhanced personal protective equipment (PPE).
Interim infection prevention and control guidance for dental settings during the COVID-19 response. December 4, 2020.
,
Clinical management of COVID-19. May 27, 2020.
In 2020, a cross-sectional study published by our group reported that the prevalence of COVID-19 among US dentists was low, with a weighted estimated rate of 0.9% (95% CI, 0.5% to 1.5%).
- Estrich C.G.
- Mikkelsen M.
- Morrissey R.
- et al.
The study’s results showed that dentists following interim safety guidance were well prepared to resume their practice.
- Estrich C.G.
- Mikkelsen M.
- Morrissey R.
- et al.
- Estrich C.G.
- Mikkelsen M.
- Morrissey R.
- et al.
there have been limited reports on rates of COVID-19 among dentists. One report evaluated safety practices in 3 specialty dental clinics in the New York, New York, area and observed 0 cases of COVID-19 among 2,810 patients, 2 dentists, and 3 registered dental hygienists during a 6-month period. The practices indicated enhanced use of PPE, increased measures to screen and protect patients seeking care, and assessment of infection risk factors.
Considering the infection rate in New York, New York, at the time, the authors concluded that oral health care can be safely provided as long as appropriate safety measures are followed.
Another report surveyed 454 members of the American Academy of Endodontics, finding a high rate of adherence to enhanced infection control measures, including the use of N95 respirator (also called an “N95 mask”) by 83.1% of the participants.
- Martinho F.C.
- Griffin I.L.
Interim infection prevention and control guidance for dental settings during the COVID-19 response. December 4, 2020.
,
ADA interim guidance for management of emergency and urgent dental care.
As of December 2020, the revised CDC interim recommendations mandated that dental HCPs wear N95 masks or those that offer an equivalent or higher level of protection, gowns or protective clothing, and gloves and eye protection (goggles or full face shields) during AGPs and in areas with moderate to substantial community transmission of COVID-19 during AGPs.
Guidance for dental settings. December 4, 2020.
- ▪
determine the cumulative prevalence rate of COVID-19 among dentists;
- ▪
calculate the monthly incidence rate for the same population over the course of the study;
- ▪
assess the level of engagement in specific infection control practices among dentists over a 6-month period.
Methods
- Estrich C.G.
- Mikkelsen M.
- Morrissey R.
- et al.
We made several changes to the questionnaire after the first survey on June 8, 2020, which are detailed in the Supplemental File. All participants signed an electronic informed consent before starting the survey.
Interim infection prevention and control guidance for dental settings during the COVID-19 response. December 4, 2020.
- Estrich C.G.
- Mikkelsen M.
- Morrissey R.
- et al.
Results
- Estrich C.G.
- Mikkelsen M.
- Morrissey R.
- et al.
but was included in this analysis.
- Estrich C.G.
- Mikkelsen M.
- Morrissey R.
- et al.
When exploring factors potentially related to participation rates, we observed that age, sex, race and ethnicity, region, and dental practice type were not associated with continued participation (P > .3). Among the respondents, 536 (an estimated 24.4%) had at least 1 medical condition associated with higher risk of developing severe illness from COVID-19, most commonly asthma (160 [7.3%]) and obesity (166 [7.6%]).
TableCharacteristics of the survey sample and comparison with all private practice or public health dentists licensed in United States.

Figure 1Dentists reporting any in-person contact outside the home, by month and US Census Bureau division (9,320 observations).
Throughout the study period, a minority of participants reported contact with someone with a suspected or confirmed COVID-19 infection in the past month. The percentage reporting contact with someone with COVID-19 significantly increased over time, from 4.6% (n = 100) in the first survey to 16.1% (n = 208) in the final survey (P < .01). In total, contact with someone with a suspected or confirmed COVID-19 infection was reported 875 times among the 2,196 participants over the course of 6 months; 430 (49.1%) of those reports were because of contact with dental patients. Another 310 (35.4%) stated that within the past month a coworker had COVID-19. In the study period, the likely source of COVID-19 was identified via contact tracing by a health agency or clinic in only 23 cases among dentists; in 2 instances, the dental practice was identified as the likely infection source.

Figure 2Personal protective equipment use according to Centers for Disease Control and Prevention interim guidelines for dental settings by month (8,966 observations, restricted to those practicing dentistry each month). AGP: Aerosol-generating procedure.
Interim infection prevention and control guidance for dental settings during the COVID-19 response. December 4, 2020.
In the first month, only 355 (17.6%) dentists reported changing their masks or respirators between patients, and 407 (20.2%) changed them only if soiled or damaged. Over time, there was a decrease in PPE optimization, as significantly more dentists changed their masks with every patient (P

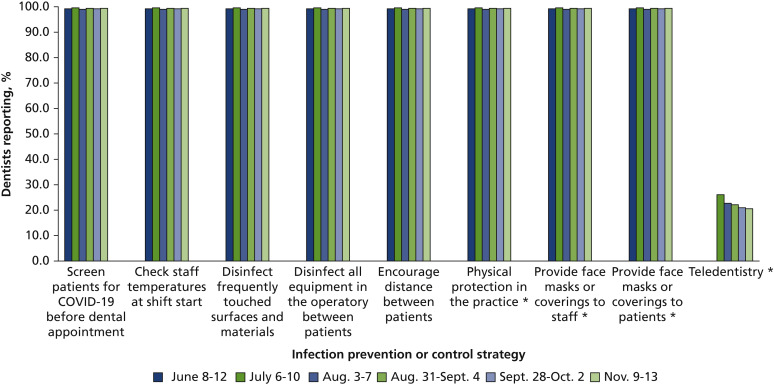
Figure 3Infection prevention and control methods used in dental practices by month (8,966 observations, restricted to those practicing dentistry each month). ∗ Significantly different over time, P < .05

Figure 4Monthly incidence and percentage ever had COVID-19 in survey of US dentists, June through November 2020 (n = 2,196).
Discussion
- Wei W.E.
- Li Z.
- Chiew C.J.
- Yong S.E.
- Toh M.P.
- Lee V.J.
; however, no confirmed cases of COVID-19 transmission related to patients’ receiving oral health care have been reported to date. Furthermore, the results of our earlier cross-sectional study
- Estrich C.G.
- Mikkelsen M.
- Morrissey R.
- et al.
and the results of this study show that prevalence and incidence rates among dentists continue to be very low in comparison with the population as a whole and with other HCPs.
- Nguyen L.H.
- Drew D.A.
- Graham M.S.
- on behalf of the Coronavirus Pandemic Epidemiology Consortium
- et al.
compared with findings from our study. A prevalence of COVID-19 was found among 2,727 cases per 100,000 HCPs compared with 242 cases per 100,000 people in the general population. The high number of cases mostly were associated with direct contact with infected patients and lack of appropriate PPE, with the highest rates reported in large metropolitan areas such as New York, New York, and London, United Kingdom.
- Nguyen L.H.
- Drew D.A.
- Graham M.S.
- on behalf of the Coronavirus Pandemic Epidemiology Consortium
- et al.
In addition, the same study showed that in the United States, 4.1% of medical HCPs were tested during the period of the study compared with 1.1% of the general population. In another report, results of a cross-sectional survey of front-line HCPs in the United States (n = 3,083) showed a reported prevalence rate of 29%,
- Firew T.
- Sano E.D.
- Lee J.W.
- et al.
which is much higher than the 2.6% rate among dentists reported in our study. In August 2020, 24% of employees of a large oncology hospital in New York, New York, were quarantined because of COVID-19.
- Press R.H.
- Hasan S.
- Chhabra A.M.
- Choi J.I.
- Simone C.B.
Another cross-sectional study examined levels of antibodies among HCPs and indicated that 265 of the 500 HCPs tested showed presence of SARS-CoV-2 antibodies, possibly resulting from a previous infection with the virus.
- Venugopal U.
- Jilani N.
- Rabah S.
- et al.
Compared with these reports of nondental HCPs, our longitudinal data show lower rates for US dentists over the June through November 2020 time frame. Although the near universal adoption of enhanced PPE per the interim CDC guidance may have minimized the risk of getting an infection in the dental office, we also observed a higher rate of testing among dentists (up to 43.9%) than front-line HCPs. Despite this high testing rate, the cumulative prevalence among dentists in our survey was 2.6% by November 13, 2020.
Furthermore, dentists have shown continued low monthly incidence of disease despite several regional and national COVID-19 rate spikes during the study period. This may indicate that dentists are able to mitigate much of their own exposure in clinical environments through consistent use of enhanced PPE and interim guidance adherence. The results of our study show high rates of preappointment screening of patients and appropriate infection control measures throughout the study period.
- Seidelman J.L.
- Lewis S.S.
- Advani S.D.
- et al.
An important distinction between dentists and other HCPs is that many medical procedures that do not involve intubation for anesthesia can be performed while a patient is wearing a mask. However, dental procedures universally require patients to be seen unmasked. This highlights the importance of continued use of enhanced PPE, in particular N95 masks, and the need for continued availability and prioritization of such protections for dental HCPs. We observed a minor shift in the use of PPE during the 6-month period of our study, most likely owing to access to the equipment, clinical judgment, schedule planning, and other resources that dentists implemented since practice reopening. In mid-November 2020, 59.8% of dental practices in the United States reported having at least a 2-week supply of N95 or KN95 masks.
COVID-19: economic impact on dental practices, week of December 14 results. Health Policy Institute.
Expanded use of N95 masks may be limited by supply shortages and the number of hours each HCP may be exposed to potentially infected patients.
- Kambhampati A.K.
- O’Halloran A.C.
- Whitaker M.
- et al.
Therefore, we expect our estimation of the monthly incidence and cumulative prevalence to be affected less by hospitalization or death than survey research in professions with higher rates of severe COVID-19 cases.
Conclusions
The level of adherence to enhanced infection control procedures in response to the COVID-19 pandemic continues to be high among US dentists. The low rates of cumulative prevalence (2.6%) and monthly incidence ranging from 0.2% through 1.1% reflect the high level of self-care among dentists. Oral health care is being delivered safely because dentists are showing adherence to a strict protocol for enhanced infection control, which should help protect their patients, their dental team members, and themselves.
Supplemental Data
References
Risk of SARS-CoV-2 transmission by aerosols, the rational use of masks, and protection of healthcare workers from COVID-19.
Antimicrob Resist Infect Control. 2020; 9: 100
Preventing transmission among operating room staff during COVID-19 pandemic: the role of the Aerosol Box and other personal protective equipment.
Updates Surg. 2020; 72: 907-910
Interim infection prevention and control guidance for dental settings during the COVID-19 response. December 4, 2020.
()
Clinical management of COVID-19. May 27, 2020.
()
Estimating COVID-19 prevalence and infection control practices among US dentists.
JADA. 2020; 151: 815-824
Incidence of COVID-19 virus transmission in three dental offices: a six-month retrospective study.
Int J Periodontics Restorative Dent. 2020; 40: 853-859
A cross-sectional survey on the impact of Coronavirus disease 2019 on the clinical practice of endodontists across the United States.
J Endod. 2021; 47: 28-38
ADA interim guidance for management of emergency and urgent dental care.
()
Guidance for dental settings. December 4, 2020.
()
Presymptomatic transmission of SARS-CoV-2: Singapore, January 23–March 16, 2020. Centers for Disease Control and Prevention.
Morb Mortal Wkly Rep. 2020; 69: 411-412
Risk of COVID-19 among front-line health-care workers and the general community: a prospective cohort study.
Lancet Public Health. 2020; 5: e475-e483
Protecting the front line: a cross-sectional survey analysis of the occupational factors contributing to healthcare workers’ infection and psychological distress during the COVID-19 pandemic in the USA.
BMJ Open. 2020; 10: e 042752
Quantifying the impact of COVID-19 on cancer patients: a technical report of patient experience during the COVID-19 pandemic at a high-volume radiation oncology proton center in New York City.
Cureus. 2020; 12e7873
SARS-CoV-2 seroprevalence among health care workers in a New York City hospital: a cross-sectional analytics during COVID-19 pandemic.
Int J Infect Diseases. 2021; 102: 63-69
Universal masking is an effective strategy to flatten the severe acute respiratory coronavirus virus 2 (SARS-CoV-2) healthcare worker epidemiologic curve.
Infect Control Hospital Epidem. 2020; 41: 1466-1467
COVID-19: economic impact on dental practices, week of December 14 results. Health Policy Institute.
()
COVID-19-associated hospitalizations among health care personnel: COVID-net, 13 states, March 1-May 31.
Morb Mortal Wkly Rep. 2020;
Biography
Dr. Araujo is the chief science officer, American Dental Association, and the chief executive officer, ADA Science and Research Institute, Chicago, IL.
Dr. Estrich is a health science research analyst, ADA Science and Research Institute, Chicago, IL.
Mr. Mikkelsen is the manager of education surveys, American Dental Association Health Policy Institute, Chicago, IL.
Ms. Morrissey is an education research analyst, American Dental Association Health Policy Institute, Chicago, IL.
Ms. Harrison is a coordinator for research and editing, American Dental Association Health Policy Institute, Chicago, IL.
Dr. Geisinger is a professor and the director, Advanced Education Program in Periodontology, University of Alabama at Birmingham, Birmingham, AL.
Dr. Ioannidou is a professor, Oral Health and Diagnostic Sciences, and the director, Dental Clinical Research Center, University of Connecticut Health Center, Farmington, CT.
Dr. Vujicic is the chief economist and vice president, American Dental Association Health Policy Institute, Chicago, IL.
Article Info
Publication History
Published online:
Accepted:
March 25,
2021
Received in revised form:
March 22,
2021
Received:
January 22,
2021
Footnotes
Disclosures. The authors have no disclosures to report.
The authors thank all of the dentists who participated in this survey and shared their time and expertise and Kelly O’Brien for her advice and insights.
Identification
DOI: https://doi.org/10.1016/j.adaj.2021.03.021
Copyright
© 2021 American Dental Association. All rights reserved.
ScienceDirect
Access this article on ScienceDirect