Background
Results from several randomized controlled trials have shown a beneficial effect of
ozone in reducing postsurgical complications after impacted mandibular third-molar
surgery, but the literature is lacking a systematic review and meta-analysis.
Methods
The authors conducted this systematic review according to the Preferred Reporting
Items for Systematic Reviews and Meta-Analyses guidelines after exclusion and inclusion
criteria were applied and the following outcome parameters were evaluated: pain, swelling,
trismus, quality of life, number of analgesics consumed, and adverse events. RevMan
Cochrane Collaboration software, Version 5.3, was used to perform meta-analysis and
the Grading of Recommendation Assessment, Development and Evaluation approach was
used to rate the certainty of evidence.
Results
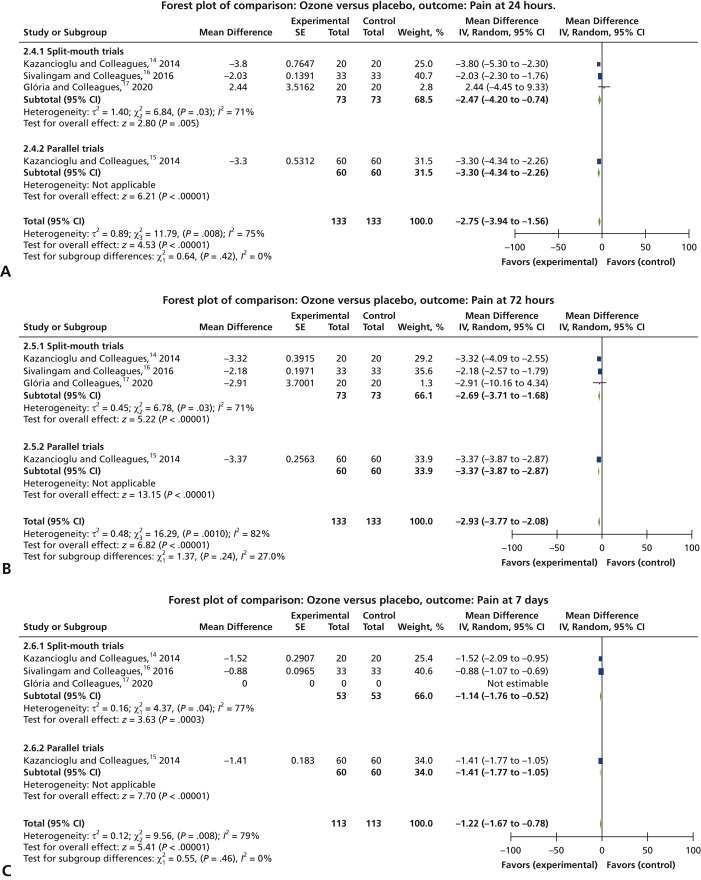
Patients who underwent adjuvant ozone application reported lower pain scores than
patients in the control group at 24 hours after surgery (95% CI, –3.94 to –1.56) and
at 7 days (95% CI, –1.67 to –0.78). Pooled analysis of all 4 included trials revealed
a standardized mean difference (SMD) in swelling of –0.44 at 24 hours, 0.63 at 72
hours, and –0.87 at 7 days after surgery in the experimental group. Higher mean estimates
in mouth opening were experienced by patients who received ozone at 24 hours (SMD,
2.74; 95% CI, –1.93 to 7.41; 4 studies, 133 patients), 72 hours (SMD, 2.77; 95% CI,
–0.63 to 6.17; 4 studies, 133 patients), and 7 days after surgery (SMD, 1.42 SMD;
95% CI, –1.34 to 4.18; 4 studies, 133 patients).
Practical Implications
Evidence suggests that adjuvant ozone application can offer some benefit for reducing
pain, improving quality of life, and decreasing mean intake of analgesics after impacted
mandibular third-molar surgery, but it is not effective in reducing facial swelling
and trismus, which paves the way for future research.