for evaluation of a large mandibular mass. The boy was born at 39-week, 1-day gestational
age to a healthy 30-year-old, gravida 2 para 1 mother. Pregnancy and delivery were
uncomplicated. Maternal prenatal laboratory tests and fetal ultrasonography at 20-weeks’
gestation were normal. There was no family history of genetic diseases or similar
lesions. The boy was born at 3,003 grams with good Apgar scores. Physical examination
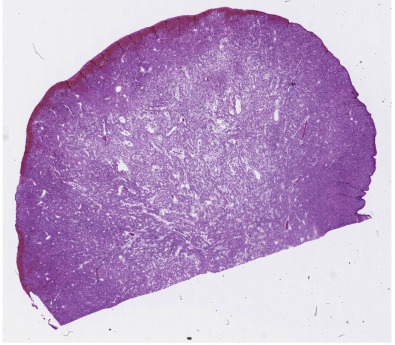
revealed a pink mass protruding out of the oral cavity (Figure 1). The mass interfered with closure of the mouth, but there was no immediate airway
obstruction. Close examination revealed a firm, 4-cm pedunculated mass attached onto
the left mandibular alveolar ridge through a vascular stalk. A primary mandibular
tooth was palpable at the base of the stalk.

Figure 1A prominent mass protruding out of the newborn’s oral cavity.
To read this article in full you will need to make a payment
References
Elin Fall von. Congenitaler epulis.
Arch Heilk. 1871; 12: 189
WHO Classification of Head and Neck Tumours.
World Health Organization,
2017Granular cell tumors of the head and neck.
J Oral Surg. 1979; 37: 402
Soft tissue tumors.
in: Neville B.W. Damm D.D. Allen C.M. Chi A.C. Oral and Maxillofacial Pathology. 4th ed. Saunders/Elsevier,
2016Congenital epulis: review of the literature and case report.
J Oral Maxillofac Surg. 1993; 51: 1040-1043
Congenital epulis of the newborn.
Oral Surg. 1977; 43: 687-691
Congenital epulis.
AJNR Am J Neuroradiol. 1997; 18: 739-741
Obstructive congenital epulis in a newborn.
Ann Plast Surg. 1991; 27: 152-155
Prenatal diagnosis of congenital epulis: a case report.
Ultrasound Obstet Gynecol. 2002; 20: 627-629
Congenital epulis: prenatal ultrasonographic and postnatal MR features with pathologic correlation.
Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008; 106: 743-748
Congenital granular cell tumor (epulis): postnatal imaging appearances.
J Comput Assist Tomogr. 2005; 29: 520-523
Congenital granular cell epulis.
Arch Pathol Lab Med. 2014; 138: 128-131
Spontaneous regression of congenital epulis: a case report and review of the literature.
J Med Case Rep. 2010; 4: 331
Oral Pathology in the Pediatric Patient: A Clinical Guide to the Diagnosis and Treatment of Mucosal Lesions.
Springer International Publishing,
2016Management of the oral hemangiomas in infants and children: scoping review.
Med Oral Patol Oral Cir Bucal. 2020; 25: e252-e261
Diagnosis and management of infantile hemangiomas.
Pediatric Clin North Am. 2014; 61: 383-402
Pediatric vascular tumors of the head and neck.
Oral Maxillofac Surg Clin North Am. 2016; 28: 105-113
Oral lymphangioma: a rare case report.
Contemp Clin Dent. 2015; 6: 584-587
Lymphangioma. In: StatPearls. StatPearls Publishing; 2020. Accessed December 4, 2020.
Oral lymphangiomas: clinical and histopathological relations: an immunohistochemically analyzed case series of varied clinical presentations.
J Oral Maxillofac Pathol. 2018; 22: S108-S111
Effectiveness of sirolimus in the treatment of complex lymphatic malformations: single center report of 56 cases.
J Pediatr Surg. 2020; 55: 2454-2458
Melanotic neuroectodermal tumor of infancy: review of literature and case report.
J Pediatr Surg. 2008; 43: E25-E29
Melanotic neuroectodermal tumor of infancy: a systematic review.
J Oral Maxillofac Surg. 2015; 73: 1946-1956
Melanotic neuroectodermal tumor of infancy: a neoplasm of neural crest origin—report of a case associated with high urinary excretion of vanilmandelic acid.
Cancer. 1966; 19: 196-206
Melanotic neuroectodermal tumor of infancy: clinicopathological, immunohistochemical, and flow cytometric study.
Am J Surg Pathol. 1993; 17: 566-573
Oral teratomas: a report of 5 cases.
J Oral Maxillofac Surg. 2012; 70: 2809-2813
Cervical and oral teratoma in the fetus: a systematic review of etiology, pathology, diagnosis, treatment and prognosis.
Arch Gynecol Obstet. 2010; 282: 355-361
Congenital facial teratoma.
J Maxillofac Oral Surg. 2012; 11: 243-246
Benign teratoma of the buccal mucosa in a 9-year-old girl: report of case and review of the literature.
Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2005; 100: 598-602
Epignathus combined with cleft palate, lobulated tongue, and lingual hamartoma: report of a case.
Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006; 101: 481-486
Giant epignathus teratoma: report of a case.
J Oral Maxillofac Surg. 2007; 65: 337-340
Biography
Dr. Moon is a resident, Department of Oral and Maxillofacial Surgery, School of Dental Medicine, University of Pennsylvania, Philadelphia, PA.
Biography
Dr. Caughey is a resident, Department of Oral and Maxillofacial Surgery, School of Dental Medicine, University of Pennsylvania, Philadelphia, PA.
Biography
Mr. Wang is a DMD candidate, School of Dental Medicine, and an MPH candidate, Perelman School of Medicine, University of Pennsylvania, Philadelphia, PA.
Biography
Dr. Queenan is an assistant professor, Department of Clinical Pathology and Laboratory Medicine, Children’s Hospital of Philadelphia, Philadelphia, PA.
Biography
Dr. Ford is an assistant professor, Department of Oral and Maxillofacial Surgery, School of Dental Medicine, University of Pennsylvania, Philadelphia, PA.
Article Info
Publication History
Published online: October 13, 2021
Publication stage
In Press Corrected Proof
Footnotes
Disclosure. None of the authors reported any disclosures.
Identification
DOI: https://doi.org/10.1016/j.adaj.2021.07.010
Copyright
© 2021 American Dental Association. All rights reserved.
ScienceDirect
Access this article on ScienceDirect