Abstract
Background
Globally, children’s caries prevalence exceeds 30% and has not markedly changed in
30 years. School-based caries prevention programs can be an effective method to reduce
caries prevalence, obviate traditional barriers to care, and use aerosol-free interventions.
The objective of this study was to explore the clinical effectiveness of a comprehensive
school-based, aerosol-free, caries prevention program.
Methods
The authors conducted a 6-year prospective open cohort study in 33 US public elementary
schools, providing care to 6,927 children in communities with and without water fluoridation.
After dental examinations, dental hygienists provided twice-yearly prophylaxis, glass
ionomer sealants, glass ionomer interim therapeutic restorations, fluoride varnish,
toothbrushes, fluoride toothpaste, oral hygiene instruction, and referral to community
dentists as needed. The authors used generalized estimating equations to estimate
the change in the prevalence of untreated caries over time.
Results
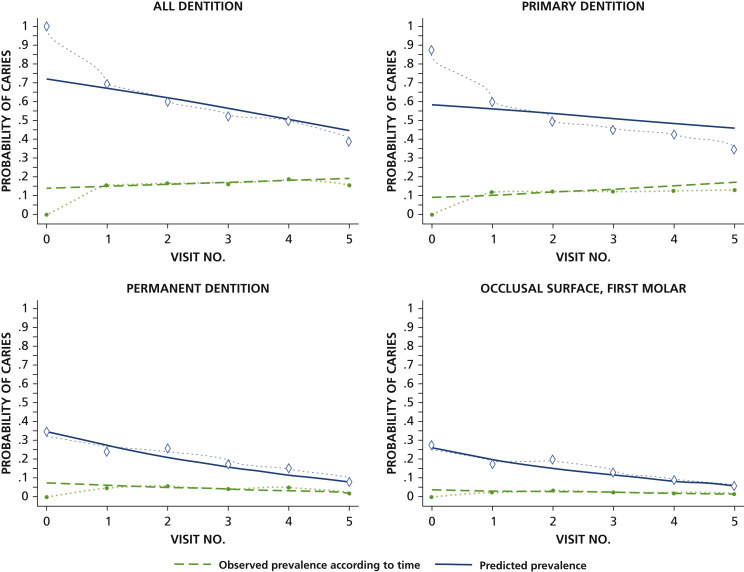
The prevalence of untreated caries decreased by more than 50%: from 39% through 18%
in phase 1, and from 28% through 10% in phase 2. The per-visit adjusted odds ratio
of untreated caries was 0.79 (95% confidence interval, 0.73 to 0.85).
Conclusions and Practical Implications
This school-based comprehensive caries prevention program was associated with substantial
reductions in children’s untreated caries, supporting the concept of expanding traditional
practices to include office- and community-based aerosol-free care.
Article Info
Footnotes
Disclosures. None of the authors reported any disclosures.
This work was supported in part by grant U24MDD006964 from the National Institutes of Health and National Institute on Minority Health and Health Disparities . This work was also supported by GC America, which provided glass ionomer, and Colgate-Palmolive, which provided fluoride varnish, fluoride toothpaste, and toothbrushes. Seed and continuing finding was provided by Dental Service of Massachusetts (now DentaQuest), Bingham Trust, the Massachusetts State Legislature, and the American Dental Trade Alliance.
The authors thank the above funding organizations. The authors thank the following people who contributed to the clinical and analytic work reported in this article: Alice Bisbee, Howard Cabral, MaryAnn Cugini, Ralph Kent, Ellen Gould, Denise Guerrero, Carolina Hommes, Timothy Martinez, Valarie Osborn, John Roberge, Aronita Rosenblatt, Karina Roldan, Jennifer Soncini, Michael Stanley, Philip Stashenko, Mary Tavares, Xiaoshan Wang, and Barbara Yates. The authors thank the following community organizations that facilitated care for the children enrolled in the study: The Lynn and Harbor Community Health Centers (T. Martinez) and the Lynn, Boston, and Cape Cod, Massachusetts, school systems. The authors particularly thank New England Survey Systems (J. Roberge and M. Stanley) for their work in developing the proprietary electronic patient record software used in data collection for this study. The authors also thank the Massachusetts Department of Health (M. Foley and L. Bethel) for background guidance. Finally, the authors posthumously thank and dedicate this article to Drs. Dominick DePaola and James Ware. Dr. DePaola from the Forsyth Institute inspired this work, and Dr. Ware from the Harvard School of Public Health assisted in developing the statistical analysis plan.
Identification
DOI: https://doi.org/10.1016/j.adaj.2020.12.005
Copyright
© 2020 Published by Elsevier Inc. on behalf of the American Dental Association.
ScienceDirect
Access this article on ScienceDirect