Abstract
Background
The objective of this study was to evaluate differences in number and type of radiographs used among 3 age groups (0-5, 6-12, 13-18 years) by general dentists, pediatric dentists, and other specialists, and to determine the association between number and type of radiographs and clinical need.
Methods
A retrospective analysis of insurance claims by age group and oral health care provider type included children aged 0 through 8 years in 2005 who had a minimum of 10 years of continuous eligibility. Indicator claim variables were calculated to identify high-risk, high-need patients.
Results
A total of 6,712,155 records from 105,010 patients and 34,406 providers were analyzed. There was a significant effect (P < .001) of age on the number of radiographs obtained per visit. The estimated rates of radiographs per visit for ages 0 through 5, 6 through 12, and 13 through 18 were 0.373, 0.492, and 0.393, respectively. There was a significant interaction effect between age and provider type. For patients younger than 13 years, general dentists had lower rates of obtaining radiographs than did pediatric dentists, with no significant difference between providers for the 13- through 18-year age group. Treatments received, except for extractions and prosthodontics, were significantly associated with rate of radiographs per visit, with “number of restorations” as an indicator of increased risk, need, or both showing an inverse association with radiograph use.
Conclusions
Child age and provider type had an effect on number of radiographs obtained per visit. Lack of caries diagnostic codes and uncommon use of risk codes hindered interpretation of whether use, frequency, or both is associated with need.
Practical Implications
Radiograph use should follow existing guidelines or recommendations based on clinical need.
Guideline on prescribing dental radiographs for infants, children, adolescents, and persons with special health care needs. 2017. Revised 2021.
In addition, in pediatric patients, radiographs provide information regarding the position and development of the dentition and related facial structures.
Guideline on prescribing dental radiographs for infants, children, adolescents, and persons with special health care needs. 2017. Revised 2021.
,
Dental radiographic examinations: recommendations for patient selection and limiting radiation exposure. Revised 2012.
However, the guidelines allow for a range of interpretation that results in a broad variance of radiographic exposure among patients. In 1995, Bohay and colleagues
- Bohay R.
- Stephens R.
- Kogon S.
surveyed general dentists (GDs) and pediatric dentists (PDs) and found that although most of the respondents followed existing guidelines for children younger than 6 years, this was not the case for children with mixed dentition. In 1999, Button and colleagues
- Button T.
- Moore W.
- Goren A.
found that excessive prescription of bite-wing radiographs by dentists was due to a lack of clear understanding of the criteria for prescription. In 2014, a national campaign called Image Gently was launched in the United States with the goal of increasing awareness about the effects of excessive ionizing radiation in children.
Major national and international organizations responsible for evaluating radiation risk agreed that dentists should act as if even low doses of radiation may potentially cause harm and should always minimize the prescription of radiographs according to the as low as diagnostically acceptable, being indication-oriented and patient-specific principle.
Methods
were calculated to identify high-risk, high-need patients: number of extractions, problem-focused evaluations, restorations, endodontic therapies, periodontic therapies, prosthodontic therapies, oral surgery codes, and orthodontic treatment codes.
Primary outcomes of the study included counts of radiographs obtained within each age group and counts of specific radiograph types (such as ≥ 2 bite-wing radiographs, full-mouth series, occlusal radiographs, panoramic radiographs, lateral cephalometric radiographs, and cone-beam computed tomographic scans) within each age group. Counts and types of radiographs were summarized as means (standard deviations) and range by age group and by provider type. Histograms were used to graphically explore counts of radiographs and types by age group and provider type. Owing to overdispersion in the radiograph counts, a negative binomial random effect model was used to evaluate the association of the number of radiographs with age group, provider type, and other high-risk patient characteristics; high-risk patient characteristics were included to account for possible differences among provider types and ages for factors that might affect the need for radiographs. Poisson regression was used to explore the association of number of specific radiograph types with age and provider type. The interaction of age by provider type was tested. The number of visits (with visits defined per encounter date) was included in the model as an exposure variable. The possibility of correlation between outcomes from the same patient was accounted for in the models by a random patient effect. For other specific types of radiographic outcomes (that is, panoramic radiographs and lateral cephalometric radiographs) logistic regression models were used to explore association of the presence of these specific radiographs with age and provider type. Number of visits was included in the model as a covariate. Few children in the 0- through 5-year age group underwent these types of radiography, and, thus, they were excluded from these analyses. Results from the negative binomial and Poisson models are presented as rates and incidence rate ratios (IRRs) with 95% CIs, and as odds ratios (ORs) with 95% CIs from logistic regression models. All statistical tests were conducted as 2-sided tests with a 5% level of significance.
Results
Effect of age and oral health care provider type on total number of radiographs
Table 1Summary of specific radiograph types by age group.
Table 2Estimated rates of radiographs obtained per visit by age and oral health care provider type.
Table 3Estimated incidence rate ratios of radiographs between general and pediatric dentists by age group.
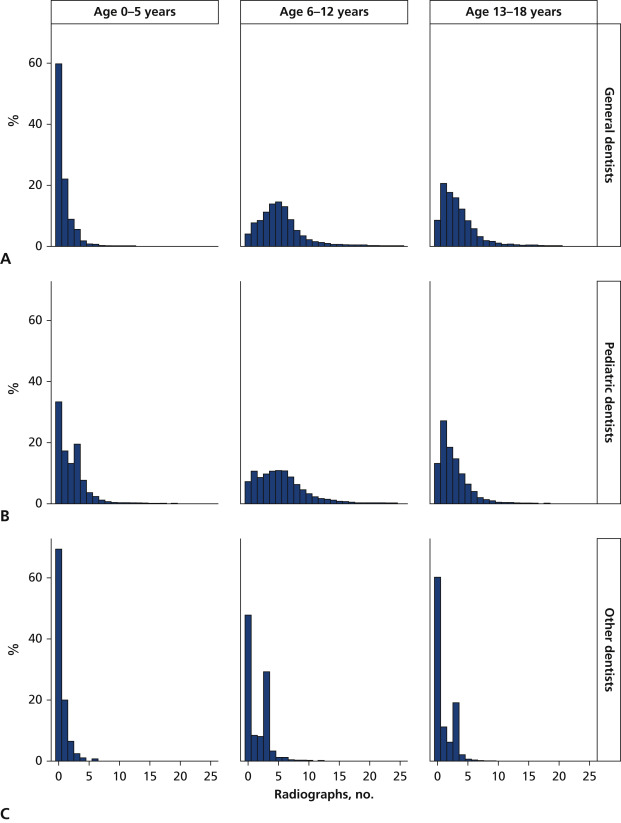
FigureDistribution of the number of radiographs per person by age and provider type. General dentists (A), pediatric dentists (B), others (C).
Effect of age and oral health care provider type on number of bite-wing radiographs
Table 4Estimated rates of radiographs per patient per visit, by age and oral health care provider type, for all radiograph types and bite-wing radiographs.
Effect of age and oral health care provider type on use of lateral cephalometric radiographs
The interaction between age and oral health care provider type was significant (P < .0001). Patients aged 6 through 12 years were more likely to undergo lateral cephalometric radiography if seen by a GD than a PD (0.6% versus 0.4%; OR, 1.511; 95% CI, 1.343 to 1.699; P < .0001), whereas provider type was not a factor for 13- through 18-year-olds (1.6% versus 1.7%; OR, 0.945; 95% CI, 0.813 to 1.098; P = .4583). Thirteen- through 18-year-olds were more likely to undergo lateral cephalometric radiography than 6- through 12-year-olds (GDs: OR, 2.579; 95% CI, 2.384 to 2.790; P < .0001; PDs: OR, 4.124; 95% CI, 3.448 to 4.933; P < .0001).
Effect of age and oral health care provider type on use of panoramic radiographs
The interaction between age and oral health care provider type was significant (P < .0001). Patients aged 6 through 12 years were less likely to undergo panoramic radiography if seen by a GD than a PD (14.6% versus 23.0%; OR, 0.572; 95% CI, 0.554 to 0.589; P < .0001), whereas provider type was not a factor for 13- through 18-year-olds (18.7% versus 18.0%; OR, 1.048; 95% CI, 0.997 to 1.102; P = .0671). Thirteen- through 18-year-olds were more likely to undergo panoramic radiography than 6- through 12-year-olds if seen by GDs (OR, 1.349; 95% CI, 1.311 to 1.389; P < .0001); however, 13- through 18-year-olds were less likely to have had a panoramic radiograph obtained than 6- through 12-year-olds if seen by PDs (OR, 0.736; 95% CI, –0.697 to 0.777; P < .0001).
Effect of risk factor (that is, treatment type) on number and type of radiographs
Patient risk factors (that is, types of treatment received), except for number of extractions (P = .0762) and number of prosthodontic therapies (P = .8248), were significantly associated with the rate of radiographs. However, there was a significant interaction between age and oral health care provider type (P < .0001). After adjusting for all risk factors, patients in the 6- through 12-year and 13- through 18-year age groups who were treated by GDs had a 2 times higher incidence rate of having radiographs than patients in the 0- to 5-year age group (P < .0001; IRR, 1.91; 95% CI, 1.89 to 1.94 and 2.05; 95% CI, 2.02 to 2.08, respectively). Patients in the 13- through 18-year age group also had a 1.1 times higher incidence rate of having radiographs than patients in the 6- through 12-year age group (P < .0001; IRR, 1.07; 95% CI, 1.07 to 1.08). Among patients treated by PDs, the 6- through 12-year age group had a 4.3% higher incidence rate of radiographs than the 0- through 5-year age group (P < .0001; IRR, 1.04; 95% CI, 1.03 to 1.06), and the 13- through 18-year age group had 5.5% lower incidence rate of radiographs than the 6- through 12-year age group (P < .0001; IRR, 0.95; 95% CI, 0.93 to 0.96). There was no significant difference between the 0- through 5-year and 13- through 18-year age groups (P = .1157). After controlling for age and provider type, every additional occurrence of problem-focused evaluation, endodontic therapy, periodontal therapy, and oral surgery was associated with an estimated 3.2%, 4.2%, 2.4%, and 0.6% increase in rate of having radiographs, respectively (all P < .0001 except oral surgery, P = .0326). However, for every additional occurrence of restoration and orthodontic encounter, the estimated rate of radiography decreased by 0.8% and 2.7%, respectively (P < .0001).
Discussion
Guideline on prescribing dental radiographs for infants, children, adolescents, and persons with special health care needs. 2017. Revised 2021.
,
Dental radiographic examinations: recommendations for patient selection and limiting radiation exposure. Revised 2012.
To balance the risks and benefits and to minimize radiation exposure the guidelines also suggest that decisions should be individualized (for example, by age, type of dentition, or whether it is a new patient or recall appointment) and always preceded by a clinical examination and review of patient history and caries risk.
Guideline on prescribing dental radiographs for infants, children, adolescents, and persons with special health care needs. 2017. Revised 2021.
,
Dental radiographic examinations: recommendations for patient selection and limiting radiation exposure. Revised 2012.
In agreement with the literature, we found that child age was associated with the number of radiographs obtained over time. The 0- through 5-year age group had the lowest number of radiographs regardless of the type of oral health care provider. This is expected, as younger pediatric patients only have primary dentition and, in many cases, because of spacing between primary teeth, the clinical examination allows for visualization of proximal contacts.
- Meyers D.R.
- McKnight-Hanes C.
- Dushku J.C.
- Thompson W.O.
- Durham L.C.
Thus, radiographs do not provide a clear benefit over visual examination for detection of carious lesions in most children younger than 6 years.
- Pontes L.R.A.
- Novaes T.F.
- Lara J.S.
- et al.
Many providers may also decide to postpone radiographs until a later age for patient comfort and owing to behavioral issues.
- Yepes J.F.
- Powers E.
- Downey T.
- et al.
also using private dental insurance claims, found that GDs prescribed more panoramic radiographs in patients younger than 5 years, whereas PDs prescribed more for 7- through 8-year-olds, with no differences by provider in 9- through 18-year-olds. In our study, patients aged 6 through 12 years were also less likely to undergo panoramic radiography if seen by a GD than a PD, with provider type not being a factor for 13- through 18-year-olds. Obtaining panoramic radiographs more frequently in older children aligns with current guidelines, which state that these radiographs should not be recommended for routine care before eruption of the permanent mandibular first molars.
Guideline on prescribing dental radiographs for infants, children, adolescents, and persons with special health care needs. 2017. Revised 2021.
,
Dental radiographic examinations: recommendations for patient selection and limiting radiation exposure. Revised 2012.
The fact that GDs obtain them more frequently in younger children may be associated with issues concerning behavior management or the need to anticipate potential problems that could require early referral. On the other hand, it is unclear why 6- to 12-year-olds were more likely to undergo lateral cephalometric radiography if seen by a GD.
- Meyers D.R.
- McKnight-Hanes C.
- Dushku J.C.
- Thompson W.O.
- Durham L.C.
The 6- through 12-year age group had more radiographs prescribed by PDs, which is expected as contacts close and radiographs can facilitate interproximal caries diagnosis. The 13- through 18-year age group had more radiographs as prescribed by GDs, with no significant difference in number of radiographs ordered per visit by GDs and PDs. As pediatric patients gets older, GDs would tend to refer these patients less often to a PD and would feel more comfortable treating them in their office; this would increase the number of radiographs in this age group. Also, these patients are going to have a mostly permanent dentition, and the need for radiographs to assess proximal surfaces that are no longer visualized clinically increases in this age group.
- Foster Page L.A.
- Boyd D.
- Fuge K.
- et al.
These trends are similar to claims data from the Netherlands, in which PDs obtained more radiographs in children until 8 years of age, with no significant difference among providers for children aged 12 through 17 years.
- Schorer-Jensma M.A.
- Veerkamp J.S.J.
- Muzzin K.B.
- Flint D.J.
- Schneiderman E.
A survey of GDs in England found that whereas 71% of respondents accepted the influence of high-risk factors (that is, multiple restorations, irregular attendance, and poor oral hygiene) in prescribing bite-wing radiographs, the influence of low-risk factors was less clear, with only good oral hygiene and few restorations perceived as relevant.
- Rushton V.E.
- Horner K.
- Worthington H.V.
Also, fissure sealants were an influence in favor of radiography by almost one-third of dentists, even when radiographs are not indicated before placing a sealant.
- Fontana M.
- Zero D.T.
- Beltrán-Aguilar E.D.
- Gray S.K.
Dentists were also influenced by patients’ opinions and by fear of legal consequences.
- Rushton V.E.
- Horner K.
- Worthington H.V.
- Kalenderian E.
- Ramoni R.L.
- White J.M.
- et al.
,
- Shimpi N.
- Ye Z.
- Koralkar R.
- Glurich I.
- Acharya A.
As expected, endodontic therapies had the greatest increase in the rate of radiographs, as most of these procedures would require multiple radiographs.
- Foster Page L.A.
- Boyd D.
- Fuge K.
- et al.
However, the number of restorations did not reflect the need for radiographs. In fact, additional numbers of restorations slightly decreased the rate of radiographs per visit. This may be explained, in part, by the fact that restored teeth are unlikely to require radiographic follow-up evaluation in pediatric patients.
- Kühnisch J.
- Anttonen V.
- Duggal M.S.
- et al.
- Gillies R.C.
- Quiñonez C.
- Wood R.E.
- Lam E.W.N.
Factors more strongly associated with overprescription were
- Gillies R.C.
- Quiñonez C.
- Wood R.E.
- Lam E.W.N.
seeing patients after images were obtained, owning a panoramic and a cone-beam computed tomographic imaging system, and the belief that images should be obtained to screen for occult pathoses.
- Hedesiu M.
- Marcu M.
- Salmon B.
- et al.
Irradiation provided by dental radiological procedures in a pediatric population.
- ▪
Data collected were based on claims of a single commercial insurance company (and how they reimburse for radiographs may also affect behaviors) and may not represent other segments of dental practice, for example, out-of-pocket payments and public insurance (Medicaid).
- ▪
The number of radiographs obtained per age group is likely underestimated, as it is expected that poor-quality radiographs that are reobtained would not be submitted for insurance coverage.
- ▪
Limitations in the available claims data affected factors that were assessed to determine clinical needs.
- ▪As we did not have access to sociodemographic data, it is not known how these factors may have affected the study outcomes. Similar limitations have been identified in other radiographic prescription studies.10
- Yepes J.F.
- Powers E.
- Downey T.
- et al.
Prescription of panoramic radiographs in children: a health services assessment of current guidelines.
Biography
Dr. Fontana is a professor, Department of Cariology, Restorative Sciences and Endodontics, School of Dentistry, University of Michigan, Ann Arbor, MI.
Dr. Yepes is a professor, Department of Pediatric Dentistry, School of Dentistry, Indiana University, Indianapolis, IN.
Mr. Eckert is a biostatistician, Department of Biostatistics and Health Data Science, School of Medicine and Richard M. Fairbanks School of Public Health, Indiana University, Indianapolis, IN.
Dr. Hale is a pediatric dentist, Grand Blanc, MI.
Dr. Benavides is a clinical associate professor, Department of Periodontics and Oral Medicine, School of Dentistry, University of Michigan, Ann Arbor, MI.
Article Info
Publication History
Published online: February 03, 2022
Accepted:
September 29,
2021
Received in revised form:
September 27,
2021
Received:
May 27,
2021
Publication stage
In Press Corrected Proof
Footnotes
Disclosure. Dr. Fontana is a scientific advisory consultant for the Delta Dental Plans Association.
Statistical analyses were supported through a gift from Renaissance Health Services.
The authors thank Delta Dental Plans Association for access to their database; Baye Fitsum, MS, biostatistician, Department of Biostatistics and Health Data Science, School of Medicine and Richard M. Fairbanks School of Public Health, Indiana University, for help with the analyses; and Renaissance Health Services for support for the conduct of this study.
Identification
DOI: https://doi.org/10.1016/j.adaj.2021.09.014
Copyright
© 2022 American Dental Association.
User License
Creative Commons Attribution – NonCommercial – NoDerivs (CC BY-NC-ND 4.0) |

Permitted
For non-commercial purposes:
- Read, print & download
- Redistribute or republish the final article
- Text & data mine
- Translate the article (private use only, not for distribution)
- Reuse portions or extracts from the article in other works
Not Permitted
- Sell or re-use for commercial purposes
- Distribute translations or adaptations of the article
Elsevier’s open access license policy
ScienceDirect
Access this article on ScienceDirect