Background
In 2007, the American Heart Association recommended that antibiotic prophylaxis (AP)
be restricted to those at high risk of developing complications due to infective endocarditis
(IE) undergoing invasive dental procedures. The authors aimed to estimate the appropriateness
of AP prescribing according to type of dental procedure performed in patients at high
risk, moderate risk, or low or unknown risk of developing IE complications.
Methods
Eighty patients at high risk, 40 patients at moderate risk, and 40 patients at low
or unknown risk of developing IE complications were randomly selected from patients
with linked dental care, health care, and prescription benefits data in the IBM MarketScan
Databases, one of the largest US health care convenience data samples. Two clinicians
independently analyzed prescription and dental procedure data to determine whether
AP prescribing was likely, possible, or unlikely for each dental visit.
Results
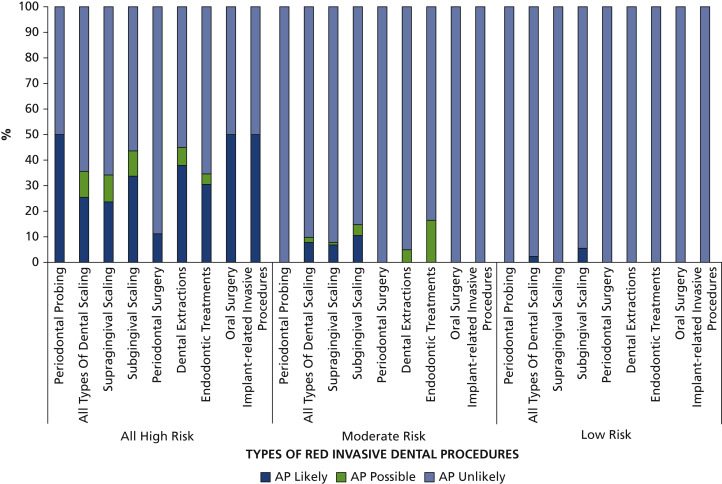
In patients at high risk of developing IE complications, 64% were unlikely to have
received AP for invasive dental procedures, and in 32 of 80 high-risk patients (40%)
there was no evidence of AP for any dental visit. When AP was prescribed, several
different strategies were used to provide coverage for multiple dental visits, including
multiday courses, multidose prescriptions, and refills, which sometimes led to an
oversupply of antibiotics.
Conclusions
AP prescribing practices were inconsistent, did not always meet the highest antibiotic
stewardship standards, and made retrospective evaluation difficult. For those at high
risk of developing IE complications, there appears to be a concerning level of underprescribing
of AP for invasive dental procedures.
Practical Implications
Some dentists might be failing to fully comply with American Heart Association recommendations
to provide AP cover for all invasive dental procedures in those at high risk of developing
IE complications.