Alif Moosajee presents a restorative and tooth whitening case study that achieved a highly accurate and predicable result.
32-year-old male patient presented with dissatisfaction with the appearance of his three-unit bridge. This spanned his upper right central incisor to upper left lateral incisor. He also complained that the bridge felt bulky and uncomfortable against his upper lip. On examination, he exhibited some gum recession, but had no other oral health or medical problems (Figure 1).
During a discussion about replacing the bridge, the patient was asked if he was happy with the overall colour of his teeth. It was suggested he might like to consider tooth whitening prior to having the new appliance fitted, as once the new bridge was created, it would not be possible to change the colour of the porcelain.
The patient readily agreed and the top and bottom arches were scanned with the Itero 5D digital scanner to ensure the most accurate tooth whitening trays could be created.
The patient was provided with Zoom Daywhite and instructions to whiten daily for two weeks. They were advised this because the whitening gel is presented in a dual barrel. It is mixed as it is dispensed. Therefore, he simply needed to inject a tiny dot into each scallop of the trays. He was also advised that the syringes did not need to be stored in a fridge.
The patient was very happy with the outcome of his whitening. He noted that his teeth were several shades lighter and had a healthy lustre (Figure 2). The patient experienced no sensitivity as a result of the presence of amorphous calcium phosphate (ACP) in the Zoom gel formulation.
Bridge fabrication
Photographs were taken of the patient’s newly whitened teeth to enable accurate communication with my lab technician, Lino Adolf. This enabled him to fabricate a bridge that would have the most accurate colour match possible.
The Elab protocol was used for this case. This novel digital protocol uses two elements to ensure the best level of communication about the exact colour for the restoration. Firstly, a polarising filter is used (Figure 3), which reduces the glare that comes from the teeth so that the technician is able to clearly see the character of the tooth and mimic that in his restoration.
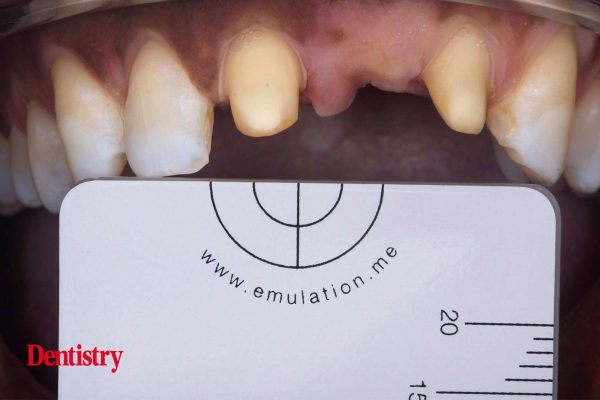
The other element is the use of a white balance grey reference card. This is a card that has a known colour temperature. When the technician receives the photograph, they are then able to calibrate the image according to that colour temperature. This means the technician can be sure that the colour of the teeth they are viewing on the monitor is exactly the same as the colour of the teeth in the mouth.
It is a beautifully elegant way of conveying the colour and character of the teeth because the standard protocol of using shade tabs is fraught with potential problems and can often lead to dissatisfaction from clinicians and patients.
Best kept secret
In my opinion, the system achieves a new standard for shade management in restorative dentistry, it represents a massive breakthrough and is a ‘best kept secret’.
As the patient’s old bridge was quite short, the teeth were prepared so that the new crowns would fit closer to the gum line. I also created a bed in the gingival tissue for the pontic part of the restoration to sit in (Figure 5).
An ovate shaped pontic was created so that the bridge would fit neatly into the gum and create the illusion of a tooth emanating from the gum rather than one simply sitting on top of it (Figures 6 and 7).
The final restoration was extremely harmonious, fitted comfortably and achieved a highly accurate colour and texture match. The patient was absolutely delighted with the final outcome. A good day is when the restoration disappears into the smile!
Discussion: colour matching challenges
The classic shade guide is not standardised if you compare one version with another, or with different porcelain powders, so the challenge of colour matching restorations with existing teeth is fraught.
Not even the best shade guide will allow dentist/laboratory technician communication about the character of the tooth. No one tooth is a uniform colour all the way through – it is typically darker at the margin. There could be cracks or little characteristic areas in it, and dentist and technician need to work out a way to describe the unique character of each tooth. One person’s B2 shade is not someone else’s B2, so the old shade guide is too blunt an instrument.
Colour
Colour is made up of:
- Hue
- Chroma
- Value.
The hue relates to the colour itself (is it red or blue or green?). The chroma is the intensity of the colour (for example, if you had a glass of water and poured blackcurrant juice into it, if one drop goes in, this has a low chroma and as you add more juice, the concentration of that purple increases – then the chroma increases).
The last aspect is value or brightness. If you were to desaturate a picture and show it as completely black and white, then the value would be assessed by going from white all the way to black, and all the shades of grey in between.
Now let’s talk about colours in dentistry. Teeth are all yellow and creamy coloured.
We use the terms chromaticity and value to assess the colour of the teeth. The chromaticity (the hue and chroma) comes from the dentine in the tooth and the value comes from the enamel.
If we can understand how these two factors together influence the colour, shade and character of the tooth, we can communicate those aspects to our technicians much more accurately, so that they can create restorations that are much more lifelike.
Shade guides were designed and arranged the shade tabs in value. Within these values, you will find the correct chromaticity (Vita 3D-Master). This was better and a step in the right direction, but there was still an issue about describing and communicating the character of the tooth. This only really changed once we were able to communicate better with photography.
Photography
The next evolutionary step was the use of photography for communication of the tooth’s unique character. However, there was still a challenge standardising what the technician was looking at from a photograph on the screen.
Another challenge was allowing the technician to see ‘through the tooth’ to detect all the character within it. So, polarising filters were introduced.
When you take a photograph of a tooth, flash bounces right back to the camera, as the tooth is shiny. The flash stops us from being able to perceive all of this character within the tooth. By using a polarising filter on the flash itself and on the lens, it is possible to counter this.
The polarising filters remove all the incidental light so you can really see all the character of the teeth; you can see mamelons and areas where there are halos and opacity of colours. These are the real details that gives the technician a blue print to make the restoration as beautiful and accurate as possible.
This article first ran in Clinical Dentistry magazine. You can sign up and receive the latest issue of Clinical Dentistry magazine here.