Abstract
Background
The authors examined trends in opioid prescriptions by dentists for children and nonsenior adults enrolled in Medicaid.
Methods
The authors used the IBM Watson Medicaid claims databases for 2012 through 2019 and the Centers for Disease Control and Prevention conversion data set. Opioid prescriptions were linked to a dental visit when prescribed within 3 days of the dental visit and if the patient had no medical visit reported during that period. The authors conducted descriptive analyses for age, procedures performed, treatment history, and prescription strength.
Results
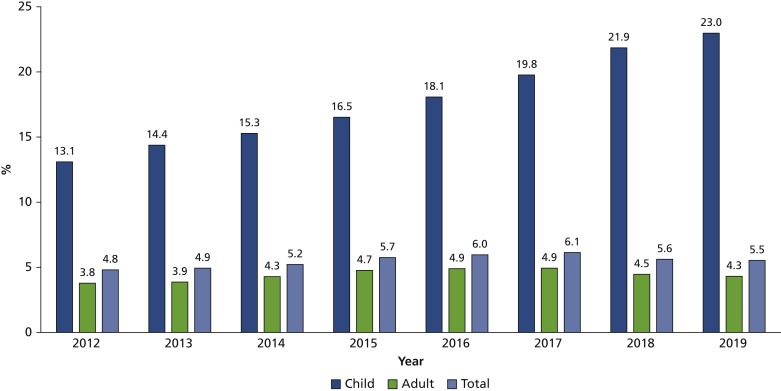
The results of the study showed consistent decreases in opioid prescription rates in dentistry during the study period from 2.7% to 1.6% among children (aged 0-20 years) and from 28.6% to 12.2% for adults (aged 21-64 years). The adult opioid prescription rate decreased for nonsurgical dental procedures from 9.7% to 2.9%. For surgical procedures, the adult prescription rate decreased from 48.0% to 28.7%. Most dental-related opioids were prescribed for oral surgeries (children, 70.8%; adults, 58.6%). By 2019, 23% of all opioid prescriptions for children were dental related.
Conclusions
The authors found that opioid prescription rates in dentistry for people enrolled in Medicaid declined substantially from 2012 through 2019 for both children and adults. The percentage of prescriptions written for nonsurgical visits consistently declined over the observed time. During the same time, opioid prescription rates for both dental surgical procedures and dental nonsurgical procedures.
Practical Implications
Although the trends revealed in the analysis show declining opioid prescription patterns, these results suggest that the overall rate is still too high and prescriptions are being written unnecessarily.
Key Words
Abbreviation Key:
CDC (Centers for Disease Control and Prevention), MME (Morphine milligram equivalent)
U.S. opioid dispensing rate maps.
This decreased to 153.3 million, or 46.7 prescriptions per 100 people, in 2019.
U.S. opioid dispensing rate maps.
Although efficacious when used and monitored appropriately, when misused, opioids are a leading cause of morbidity and mortality and have significant social and economic costs. Opioids, both prescribed and illicit, were the leading cause of drug-overdose deaths in 2017 according to the CDC and were involved in 47,800, or 68%, of all overdose-associated deaths.
Opioid overdose.
For 2017 and 2018 inclusive, the federal government allocated almost $11 billion to address the epidemic of opioid abuse.
Tracking federal funding to combat the opioid crisis, March 2019.
From 1999 through 2013, state Medicaid programs spent more than $72.4 billion to combat the epidemic, $8 billion in 2013 alone.
- Leslie D.L.
- Ba D.M.
- Agbese E.
- Xing X.
- Liu G.
The total economic burden of the opioid epidemic from 2018 through 2020 was reported to be at least $631 billion by the Society of Actuaries.
- Davenport S.
- Weaver A.
- Caverly M.
- Volkow N.D.
- McLellan T.A.
- Cotto J.H.
- Karithanom M.
- Weiss S.B.
Patients receiving oral health care in an emergency department were more than 7 times more likely to receive an opioid prescription than were patients treated in a dental office.
- Janakiram C.
- Chalmers N.I.
- Fontelo P.
- et al.
Among all dental patients, surgical, implant, and root canal procedures were associated with the highest rates of opioid prescriptions.
- Steinmetz C.N.
- Zheng C.
- Okunseri E.
- Szabo A.
- Okunseri C.
Among adolescents and young adults, dental-related visits are often the first exposure to opioids.
- Nadeau R.
- Hasstedt K.
- Sunstrum A.B.
- Wagner C.
- Tu H.
,
- McCabe S.E.
- West B.T.
- Boyd C.J.
,
- McCauley J.L.
- Hyer J.M.
- Ramakrishnan V.R.
- et al.
One study revealed that 11.2% of dentist-prescribed opioids were written for patients younger than 21 years.
- McCauley J.L.
- Hyer J.M.
- Ramakrishnan V.R.
- et al.
When exposed in high school, young adults are 33% more likely to misuse opioids in the future.
- Miech R.
- Johnston L.
- O’Malley P.M.
- Keyes K.M.
- Heard K.
More than one-half of all dental prescriptions remain unused 3 weeks after a dental surgical extraction and may lead to nonmedical misuse.
- Maughan B.C.
- Hersh E.V.
- Shofer F.S.
- et al.
It is estimated that up to 1,500 deaths annually are due to therapeutically provided dentist-written prescriptions.
- Dionne R.A.
- Gordon S.M.
- Moore P.A.
- Dowell D.
- Haegerich T.M.
- Chou R.
A 2020 study based on more than one-half million adult dental visits found that 29.3% of dental opioid prescriptions exceeded the MME-based recommendation, whereas 53% exceeded the recommended days’ supply.
- Suda K.J.
- Zhou J.
- Rowan S.A.
- et al.
- Lev R.
- Lee O.
- Petro S.
- et al.
Together with oxycodone, it remains one of the most commonly prescribed medications by dentists.
Hydrocodone, oxycodone, codeine, and tramadol are associated with high incidence of opioid-related adverse effects.
- Chung C.P.
- Callahan S.T.
- Cooper W.O.
- et al.
Tramadol is associated with higher rates of hospitalization, need for escalated care, and death than other medications, particularly among adolescents.
- Chung C.P.
- Callahan S.T.
- Cooper W.O.
- et al.
Owing to the associated medical complications of both codeine and tramadol, the US Food and Drug Administration on April 20, 2017, issued guidance recommending no use of either medication in children younger than 12 years.
FDA Drug Safety Communication: FDA restricts use of prescription codeine pain and cough medicines and tramadol pain medicines in children—recommends against use in breastfeeding women.
- Obadan-Udoh E.
- Lupulescu-Mann N.
- Charlesworth C.J.
- et al.
Among those enrolled in Medicaid who had an opioid-use disorder, the percentage without a current opioid prescription increased from 32% in 2005 to 38% in 2015, despite targeted efforts and programs designed specifically for this population.
- Ali M.M.
- Cutler E.
- Mutter R.
- et al.
In Montana, 28% of unintentional opioid deaths among adults were those enrolled in Medicaid.
- Fernandes J.C.
- Campana D.
- Harwell T.S.
- Helgerson S.D.
Although many studies have evaluated the overall impact of opioids, prescribing practices, and even particular diagnostic subsets, including dental services, there are not many studies that have reviewed only patients enrolled in Medicaid, and fewer still have evaluated specific trends and patterns in that population at the national level.
In our study, we evaluated trends in opioid prescriptions associated with a dental procedure, along with demographic and other characteristics of patients in a nationally representative population of those enrolled in Medicaid. We calculated rates of prescriptions within the population. In addition, we reviewed specific prescription types, dosages, MMEs, and procedures associated with opioids.
Methods
Data source and sample selection
IBM MarketScan Research Databases.
The database contains all individual claims from 10 million dental patients among 13 states enrolled in Medicaid across all 8 years and is considered nationally representative of the overall US population enrolled in Medicaid. This research was determined exempt from review by the Western Institutional Review Board.
- Roberts S.M.
- Wilson C.F.
- Seale N.S.
- McWhorter A.G.
We removed buprenorphine-naloxone, buprenorphine, methadone hydrochloride, buprenorphine hydrochloride, morphine sulfate-naltrexone hydrochloride, and naloxone hydrochloride-pentazocine hydrochloride owing to their use in treating opioid dependence.
Opioid addiction.
Measures
- Gupta N.
- Vujicic M.
- Blatz A.
We defined an opioid prescription as dental-related if the prescription occurred either on the same day as a dental visit or within 3 days before or after the visit. However, if a medical inpatient or outpatient visit happened within the same 3 days of the prescription, we excluded it because the reason for the prescription could not be determined as dental-related (Figure 1). We then calculated the percentage of patients receiving an opioid prescription in a calendar year by dividing the number of dental patients receiving at least 1 opioid prescription by the total number of patients receiving a dental service.
Figure 1Sample selection criteria for opioid dental claims.
Owing to differences in coverage, eligibility criteria, and guidance on prescribing of dental opioids, we stratified patients into 2 age groups: child patients aged 0 through 20 years and adult patients aged 21 through 64 years. Children and young adults younger than 21 years who are enrolled in Medicaid have mandated dental coverage and thus are eligible for early and periodic screening, diagnostic, and treatment benefits along with other covered screenings and health services. However, dental coverage is optional under federal law for adults (≥ 21 years) and varies substantially by state.
Calculating total daily dose of opioids for safer dosage.
The normalization process allowed for comparison across opioids as the formulations vary considerably in strength. In alignment with CDC recommendations, we classified MMEs into 4 groups: 0 through 19.9 MMEs, 20 through 49.9 MMEs, 50 through 89.9 MMEs, and 90 MME or greater.
- Gupta N.
- Vujicic M.
- Blatz A.
If a surgical code was not present in the claim record, we classified the visit as nonsurgical.
We performed all analysis using SAS Version 9.4 (SAS).
Results
Table 1Dental opioid prescriptions

Figure 2Dental opioid prescriptions by morphine milligram equivalent per day categories by year.

Figure 3Percentage of all opioid prescriptions that are dental related.
- Dowell D.
- Haegerich T.M.
- Chou R.
The percentage of prescriptions higher than 120 MMEs declined from 33.1% in 2012 to 16.4% in 2019. When considering the CDC recommendations based on documented days’ supply, the percentage of prescriptions for adults more than 3 days’ duration decreased from 45.0% in 2012 to 41.6% in 2019 (eTable 1, available online at the end of this article). These CDC recommendations are made for chronic pain and are not meant specifically to serve as guidelines for acute dental-related pain.
Table 2Opioid prescription rates by race or ethnicity and sex.
Table 3Percentage of opioid prescriptions associated with the procedure categories.
Table 4Opioid prescription rate for nonsurgical and surgical encounters by age group.
Discussion
The results of this study show steadily declining opioid prescription rates in patients enrolled in Medicaid since 2012, particularly among adults. Given the increased likelihood of opioid misuse and abuse for prescriptions when written for more than 50 MMEs per day, our results show a decrease from 15.5% in 2012 to 3.4% as a percentage of total in 2019 in prescriptions written for that level. These results also represent a decline in opioids prescribed for nonsurgical visits from a 9.7% prescription rate for adults in 2012 to 2.9% in 2019. Although our findings show that progress is being made, they also suggest that more improvements are necessary to reduce the rate even further through targeting of particular prescription categories.
- McCabe S.E.
- West B.T.
- Boyd C.J.
,
- McCauley J.L.
- Hyer J.M.
- Ramakrishnan V.R.
- et al.
,
- Miech R.
- Johnston L.
- O’Malley P.M.
- Keyes K.M.
- Heard K.
This early exposure may make those children more likely to misuse opioids throughout their lives.
established that pain associated with third-molar extraction is best controlled by using a combination of acetaminophen and ibuprofen rather than an opioid analgesic. Opioid analgesics often are not the most effective tool for pain relief and should not be considered a first-line choice. However, research shows that this is still not the standard. For instance, from 2000 through 2010, 42% of dental patients enrolled in Medicaid filled an opioid prescription within 7 days of having a third-molar extraction.
- Baker J.A.
- Avorn J.
- Levin R.
- Bateman B.T.
In another study, 65% of all dental-related opioids from 2013 through 2018 were prescribed for tooth extractions in a population with combined Medicaid and commercial insurance, with third molars accounting for 40% of these extractions.
- Chua K.P.
- Hou H.M.
- Waljee J.F.
- Brummett C.M.
- Nalliah R.P.
- Dowell D.
- Haegerich T.M.
- Chou R.
These guidelines were used by Suda and colleagues
- Suda K.J.
- Zhou J.
- Rowan S.A.
- et al.
to evaluate opioid prescription patterns in patients with commercial insurance. They found that 16% of dental-related Medicaid opioid prescriptions exceeded MMEs recommended for chronic pain in 2019. Regarding opioids that exceeded their recommended days’ supply, 42% were prescribed for more than 3 days in 2019 for patients enrolled in Medicaid. The results show that overprescribing has been on a consistent downward trend in dentistry covered by Medicaid.
- McCauley J.L.
- Leite R.S.
- Melvin C.S.
- Fillingam R.B.
- Brady K.T.
Our data set does not identify the individual states, so it is impossible to link our results to specific prescription-drug monitoring program regulations; however, it is likely their use is affecting these reductions.
Limitations
- Gupta N.
- Vujicic M.
- Blatz A.
We excluded prescriptions filled outside that window from the analysis. In addition, we restricted opioid claims to initial fills only and did not account for refill or repeat prescriptions.
Because this analysis uses claims data, it does not include procedures or prescriptions that were not paid or otherwise reflected in claims data. In addition, even though we excluded dual eligibilities for Medicaid and Medicare, we may have missed some procedures or prescriptions that were paid for by an alternative insurance, as Medicaid is the payer if no other insurance is available. Owing to limitations in the data, we are unable to identify the state policy environment in which the prescriptions were written. This limits our ability to identify the reasons for the decline in opioid prescriptions for dental procedures identified in our analysis or to assess the impact of the particular policy environment in which opioids were prescribed.
Conclusions
Our results are among the first to our knowledge to evaluate opioid prescribing patterns for dental patients in a nationally representative Medicaid-enrolled population. The results showed a significant reduction in overall prescription rates, especially among adults 64 years and younger. Most opioid prescriptions were affiliated with surgical visits, with the percentage written for nonsurgical visits declining for each year in the study. The percentage of prescriptions equal to or exceeding CDC guidelines of 50 MME per day declined across the study period. Although these decreases in both quantity and strength signify a positive trend, our analysis suggests that the overall rate is still too high, and prescriptions are being written unnecessarily when an alternative treatment would be more effective in managing pain and reducing the incidence of opioid use disorder.
Appendix
CDC: Centers for Disease Control and Prevention.
recommendations for chronic pain.
The CDC recommends prescribing no more than 120 morphine milligram equivalent (MME) units per prescription as well as a maximum of 3 days’ supply for chronic pain.15
The US Food and Drug Administration released guidelines in the second quarter of 2017 recommending against prescribing codeine or tramadol to children younger than 12 years for pain management.20 These medicines are associated with difficulty breathing and other potentially life-threatening complications, with effects most pronounced in children younger than 12 years.
The US Food and Drug Administration released guidelines in the second quarter of 2017 recommending against prescribing codeine or tramadol to children younger than 12 years for pain management.20 These medications are associated with difficulty breathing and other potentially life-threatening complications, with effects most pronounced in children younger than 12 years.
References
U.S. opioid dispensing rate maps.
()
Opioid overdose.
()
Tracking federal funding to combat the opioid crisis, March 2019.
()
The economic burden of the opioid epidemic on states: the case of Medicaid.
Am J Manag Care. 2019; 25: S243-S249
Economic impact of non-medical opioid use in the United States.
()
Characteristics of opioid prescriptions in 2009.
JAMA. 2011; 305: 1299-1301
Sex and race or ethnicity disparities in opioid prescriptions for dental diagnoses among patients receiving Medicaid [published correction appears in JADA. 2019;150(10):e135-e144].
JADA. 2018; 149: 246-255
Opioid analgesic prescribing practices of dental professionals in the United States.
JDR Clin Trans Res. 2017; 2: 241-248
Addressing the opioid epidemic: impact of opioid prescribing protocol at the University of Minnesota School of Dentistry.
Craniomaxillofac Trauma Reconstr. 2018; 11: 104-110
Leftover prescription opioids and nonmedical use among high school seniors: a multi-cohort national study.
J Adolesc Health. 2013; 52: 480-485
Dental opioid prescribing and multiple opioid prescriptions among dental patients: administrative data from the South Carolina prescription drug monitoring program.
JADA. 2016; 147: 537-544
Prescription opioids in adolescence and future opioid misuse.
Pediatrics. 2015; 136: e1169-e1177
Unused opioid analgesics and drug disposal following outpatient dental surgery: a randomized controlled trial.
Drug Alcohol Depend. 2016; 168: 328-334
Prescribing opioid analgesics for acute dental pain: time to change clinical practices in response to evidence and misperceptions.
Compend Contin Educ Dentist. 2016; 37: 372-378
CDC guideline for prescribing opioids for chronic pain: United States, 2016. Centers for Disease Control and Prevention.
()
Overprescribing of opioids to adults by dentists in the U.S., 2011-2015.
Am J Prev Med. 2020; 58: 473-486
Who is prescribing controlled medications to patients who die of prescription drug abuse?.
Am J Emerg Med. 2016; 34: 30-35
Dentistry and the opioid epidemic: do dentists over prescribe opioids?.
()
Individual short-acting opioids and the risk of opioid-related adverse events in adolescents.
Pharmacoepidemiol Drug Saf. 2019; 28: 1448-1456
FDA Drug Safety Communication: FDA restricts use of prescription codeine pain and cough medicines and tramadol pain medicines in children—recommends against use in breastfeeding women.
()
Opioid prescribing patterns after dental visits among beneficiaries of Medicaid in Washington state in 2014 and 2015.
JADA. 2019; 150: 259-268
Opioid use disorder and prescribed opioid regimens: evidence from commercial and Medicaid claims, 2005-2015.
J Med Toxicol. 2019; 15: 156-168
High mortality rate of unintentional poisoning due to prescription opioids in adults enrolled in Medicaid compared to those not enrolled in Medicaid in Montana.
Drug Alcohol Depend. 2015; 153: 346-349
IBM MarketScan Research Databases.
()
Evaluation of morphine as compared to meperidine when administered to the moderately anxious pediatric dental patient.
Pediatr Dent. 1992; 14: 306-313
Opioid addiction.
()
Opioid prescribing practices from 2010 through 2015 among dentists in the United States: what do claims data tell us?.
JADA. 2018; 149: 237-245
Calculating total daily dose of opioids for safer dosage.
()
American Dental Association. Code on Dental Procedures and Nomenclature (CDT Code). American Dental Association; 2021. Accessed June 11, 2021. https://www.ada.org/en/publications/cdt
Combining ibuprofen and acetaminophen for acute pain management after third-molar extractions: translating clinical research to dental practice.
JADA. 2013; 144: 898-908
Opioid prescribing after surgical extraction of teeth in Medicaid patients, 2000-2010.
JAMA. 2016; 315: 1653-1654
Opioid prescribing patterns by dental procedure among US publicly and privately insured patients, 2013 through 2018.
JADA. 2021; 152: 309-317
Dental opioid prescribing practices and risk mitigation strategy implementation: identification of potential targets for provider-level intervention.
Subst Abus. 2016; 37: 9-14
Do more robust prescription drug monitoring programs reduce prescription opioid overdose?.
Addiction. 2017; 112: 1773-1783
Biography
Mr. Okunev is a biostatistician, Analytics and Evaluation, CareQuest Institute for Oral Health, Boston, MA.
Dr. Frantsve-Hawley is the director, Analytics and Evaluation, CareQuest Institute for Oral Health, Boston, MA.
Dr. Tranby is a manager, Data and Impact, Analytics and Evaluation, CareQuest Institute for Oral Health, Boston, MA.
Article Info
Footnotes
Disclosures. None of the authors report any disclosure or conflicts of interest.
The authors would like to sincerely thank Avery Brow for his contributions in writing assistance, editing, and proofreading of this article.
Identification
DOI: https://doi.org/10.1016/j.adaj.2021.04.013
Copyright
© 2021 American Dental Association.
User License
Creative Commons Attribution – NonCommercial – NoDerivs (CC BY-NC-ND 4.0) |

Permitted
For non-commercial purposes:
- Read, print & download
- Redistribute or republish the final article
- Text & data mine
- Translate the article (private use only, not for distribution)
- Reuse portions or extracts from the article in other works
Not Permitted
- Sell or re-use for commercial purposes
- Distribute translations or adaptations of the article
Elsevier’s open access license policy
ScienceDirect
Access this article on ScienceDirect