Andrew Wallace offers his guidance on how to succeed with tooth whitening before sharing a case study demonstrating how whitening can transform a smile with minimal intervention.
When it comes to tooth whitening, a predictable outcome very much depends on a good assessment: you will always want a history and examine the teeth thoroughly and document your findings before having an open and frank conversation about your findings and expectations.
Things to ask as part of your history:
- Have your teeth always been this colour or have you noticed them get darker and at what moment in time?
- Diet history, looking for highly coloured foods eaten frequently
- Tobacco use
- Trauma or endodontics on front teeth
- Sensitivity to hot and cold.
When assessing a potential whitening case, I will look for:
- Base shade A and B shade respond more predictably
- Gradation of shade from incisal edge to cervical
- Restorations
- Cracks
- Incisal edge translucency or halo
- Cervical root exposure
- Banding
- White patches
- Incisal dentine exposure.
All of these issues will have a potential effect on the outcome and the patient needs to be forewarned of this.
Manage expectations
Patients may not have the same understanding of what is possible from whitening as the clinician. Educating the patient on what is possible comes from a thorough assessment.
A and B shades will respond most predictably and age-related discolouration will tend to reverse, most predictably.
Where the teeth start in the darker A and B shades, like A3.5, the colour change may be more noticeable to the patient than starting from A1.
Manage sensitivity
Managing sensitivity is critical to good compliance and patients need to know that some sensitivity is normal during whitening. Those that begin with some sensitivity are likely to find it more challenging.
It is important to manage any pre-existing sensitivity before beginning treatment. Often, a sensitive toothpaste used for a couple of weeks is enough, sometimes we need to use additional products, such as those containing amorphous calcium phosphate (ACP).
Using a whitening product with ACP built-in – like Philips Zoom Daywhite and Nitewhite – helps control sensitivity during treatment.
Don’t start off too strong: start off with a reduced wear time for the first few days, this helps gauge how sensitive the patient will become.
If the patient is going to have some significant sensitivity during treatment, it tends to start at day three or four.
For the first few days, I have the patient wearing it for shorter periods of time.
Using stronger gel, such as 16% carbamide peroxide, does not produce teeth that are any whiter but causes much more sensitivity. This is therefore likely to impact on patient compliance, adversely affecting the outcome.
Better photography
Photography is an amazing tool for patient communication and initiating conversations. It should, therefore, form part of your normal dental records and examination.
Simply putting a photo up on the screen in front of the patient will often initiate a conversation about whitening.
That photograph can then be used to aid in your assessment. Also, to manage the patient’s expectations about things such as colour changes of root surfaces and exposed dentine, or how white patches will react to whitening.
If your photographs are of a consistent quality, they can be used to form a portfolio of your work and are great for before and after comparisons.
If your photographs lack consistency and control of colour, they will not be very helpful for growing your whitening business.
When taking photographs for whitening or for shade matching, the reference colour tab should be at the same distance from the camera flash, otherwise it will reflect more light back to the camera and will look artificially whiter than the teeth that are further away.
Better trays
Good whitening depends on accurately fitting trays, which depend on accurate impressions or scans.
Good trays should have a very snug fit at the gingival margin. Reservoirs or gingival scalloping are no longer routinely required.
The excellent fit at the gingival margin is required to keep saliva out of the trays. This not only dilutes but also inactivates the gel.
Trays that are too thin or flex too readily will allow for the entry of saliva.
Day versus night
Daytime or night-time whitening will depend on the patient and clinician preference.
My personal preference is daytime whitening, as a lot of my patients are using aligners at the same time.
Patients who clench and grind teeth should also be treated using a daytime product, as the clenching on the trays at night will cause the trays to flex.
Know your chemistry
Dentists should know what their whitening products contain – hydrogen peroxide, carbamide peroxide – as well as the percentages contained so they can choose the right product for the right procedures.
Saturation point
The patient should be aware that treatment can take more than two to three weeks.
Often, the upper lateral incisors are the quickest teeth to respond and the lower canines can be the slowest.
In most cases, the patient should be prepared to continue until the canine teeth are of an even colour, ensuring that you have got to the saturation point of colour change.
Teeth will tend to whiten from the incisal edge and the gingival area where enamel is thinnest and dentine thickest will take longer.
Incomplete whitening will often leave ‘two-tone’ or ‘snowcapped’ canines.
Options
Different treatment options will ensure that you can cater for the patient’s requirements. We offer Philips Zoom chairside whitening in the practice for those patients who want to reduce the time required whitening at home or want the initial whitening results faster.
Maintenance
Patients need to know and to buy into the fact that they will need to maintain their whitening. Most patients will require two to three top-ups per year, normally requiring two to three days of treatment.
Case study
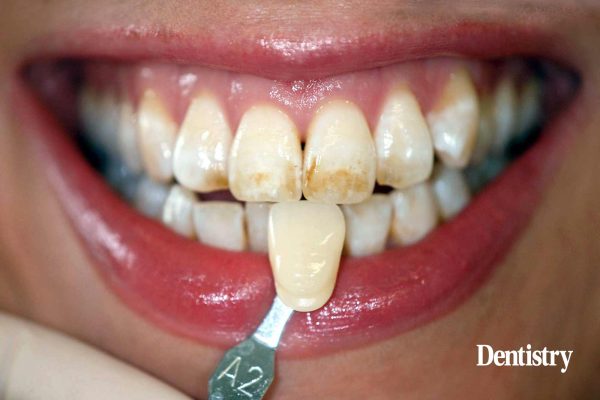
A young lady attended the practice primarily for a cosmetic assessment of her significantly discoloured teeth (Figure 1).
She had a history of several mild childhood ailments and was given fluoride supplements as a child; she had no previous restorative dental treatment.
A diagnosis of moderate enamel mottling due to fluorosis was made and a discussion ensued regarding the options available for this level and type of discolouration (Figures 2-4).
Dental whitening is a very predictable and reliable procedure. With cases of fluorosis where the teeth are marked with white and brown mottling of the enamel, the result may not always be completely successful.
Even with a significant colour improvement, this may not be enough of an improvement for the patient, as some white mottling may remain.
The patient agreed with a stepwise approach, starting with the least invasive and least expensive option, with the option to move on through the various options if the previous intervention did not satisfy her aesthetic requirement. The patient was very much on board with trying the least invasive approaches first, only moving to the next stage if required.
A variety of incremental stages were presented:
- Two-week whitening
- Four- to six-week whitening
- Enamel microabrasion
- Resin infiltration of the enamel
- Spot removal of the affected enamel and restoration with composite
- Porcelain laminate veneers.
Treatment
Starting the first stage, impressions were taken in alginate in order to create her tooth whitening trays and the patient was advised to use desensitising toothpaste.
Non-scalloped, no reservoir, closely fitting bleaching trays were made in the practice and the patient subsequently returned for a fit appointment.
During this session the whitening process was explained; the patient was shown how to apply the gel, insert the trays, and was given verbal and written instructions as well as watching a short video demonstration on the process.
They were warned to expect that the teeth may look worse initially.
The patient was supplied with the upper and lower trays and three syringes of Philips Zoom Nitewhite 10% carbamide peroxide and three tubes of 16% carbamide peroxide.
Instructions were given to start with the 10% and then move on to the stronger gel if there was no undue sensitivity.
She returned after two weeks of treatment and two weeks rest, having not used all of the gel provided but with the result that had transformed her smile and with which she was thoroughly delighted.
Reflection
This case highlights the need to have a progressive approach to cosmetic dental cases. It allows the patient to decide the end-point, rather than it being dictated by the clinician or dental laboratory.
This approach requires more discussion and explanation but, ultimately, this is time well spent as the patient has more ‘ownership’ and understanding of their problem.
Given the subjective nature of dental aesthetics, this is invaluable.
Had the patient decided that there were other aspects of her smile that she was displeased with, using bleaching as a starting intervention allows us to assess patient compliance, expectations, and makes any restorative treatment (such as porcelain laminate veneers) easier, more predictable and less invasive because we are not relying on using opaquers within the restoration, thicker restorations or cement to block out the discolouration.
Further reading
Thylstrup A, Fejerskov O (1978) Clinical appearance of dental
fluorosis in permanent teeth in relation to histologic changes. Community Dent Oral Epidemiol 6: 315-28
Pendrys DG (1999) The differential diagnosis of fluorosis. J Public Health Dent 59: 235-8
Haywood VB (2002) Dentine hypersensitivity: bleaching and restorative considerations for successful management. Int Dent J 52: 376-84
Haywood VB (2003) Frequently asked questions about bleaching. Compendium 24(4A): 324-337
Douglas RD, Przybylska M, Douglas RD, et al (1999) Predicting porcelain thickness required for dental shade matches. J Prosthet Dent 82: 143-9
Chaiyabutr Y, Kois JC, LeBeau D, et al (2011) Effect of abutment tooth color, cement color, and ceramic thickness on the resulting optical color of a CAD/CAM glass-ceramic lithium disilicate-reinforced crown. J Prosthet Dent 105: 83-90
Did you enjoy this article? Sign up to Clinical Dentistry magazine to see more.