Abstract
Background
Understanding the risks associated with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) transmission during oral health care delivery and assessing mitigation strategies for dental offices are critical to improving patient safety and access to oral health care.
Methods
The authors invited licensed US dentists practicing primarily in private practice or public health to participate in a web-based survey in June 2020. Dentists from every US state (n = 2,195) answered questions about COVID-19–associated symptoms, SARS-CoV-2 infection, mental and physical health conditions, and infection control procedures used in their primary dental practices.
Results
Most of the dentists (82.2%) were asymptomatic for 1 month before administration of the survey; 16.6% reported being tested for SARS-CoV-2; and 3.7%, 2.7%, and 0% tested positive via respiratory, blood, and salivary samples, respectively. Among those not tested, 0.3% received a probable COVID-19 diagnosis from a physician. In all, 20 of the 2,195 respondents had been infected with SARS-CoV-2; weighted according to age and location to approximate all US dentists, 0.9% (95% confidence interval, 0.5 to 1.5) had confirmed or probable COVID-19. Dentists reported symptoms of depression (8.6%) and anxiety (19.5%). Enhanced infection control procedures were implemented in 99.7% of dentists’ primary practices, most commonly disinfection, COVID-19 screening, social distancing, and wearing face masks. Most practicing dentists (72.8%) used personal protective equipment according to interim guidance from the Centers for Disease Control and Prevention.
Conclusions
COVID-19 prevalence and testing positivity rates were low among practicing US dentists. This indicates that the current infection control recommendations may be sufficient to prevent infection in dental settings.
Practical Implications
Key Words
Abbreviation Key:
ADA (American Dental Association), AGDP (Aerosol-generating dental procedure), CDC (Centers for Disease Control and Prevention), FQHC (Federally qualified health center), OSHA (Occupational Safety and Health Administration), PPE (Personal protective equipment), SARS-CoV-2 (Severe acute respiratory syndrome coronavirus 2)
How COVID-19 spreads.
The COVID-19 pandemic, with its considerable morbidity and mortality, causes social and economic disruptions and health care delivery problems. The pandemic is of particular concern owing to the airborne transmission dynamics in asymptomatic and presymptomatic people.
- Kissler S.M.
- Tedijanto C.
- Goldstein E.
- Grad Y.H.
- Lipsitch M.
,
- Prather K.A.
- Wang C.C.
- Schooley R.T.
,
- Wei W.E.
- Li Z.
- Chiew C.J.
- Yong S.E.
- Toh M.P.
- Lee V.J.
Virus-containing droplets (5-12 micrometers) and aerosols (≤ 5 μm) from infected people are transmitted into the environment through breathing, speaking, coughing, and sneezing.
- Kutter J.S.
- Spronken M.I.
- Fraaij P.L.
- Fouchier R.A.
- Herfst S.
Susceptible people can then become infected if virus-containing respiratory droplets or aerosols settle on mucosal membranes or are inhaled.
- Kutter J.S.
- Spronken M.I.
- Fraaij P.L.
- Fouchier R.A.
- Herfst S.
Respiratory viruses like SARS-CoV-2 can also be spread if a susceptible person touches viral particles on contaminated surfaces and transfers them to their mucus membranes.
- Kutter J.S.
- Spronken M.I.
- Fraaij P.L.
- Fouchier R.A.
- Herfst S.
Multiple dental professionals at the School and Hospital of Stomatology, Wuhan University, Wuhan, China, have contracted COVID-19, but it is unclear whether these infections were due to community transmission or transmission associated with oral health care delivery.
Developing a fuller understanding of the risks to patients and practitioners related to transmission during oral health care delivery and assessing mitigation strategies within the dental office are key components of improving patient safety and access to ongoing oral health care in this pandemic environment.
and, in April and May 2020, the American Dental Association (ADA) and the Centers for Disease Control and Prevention (CDC), respectively, released interim guidance on infection control protocols and changes to the practice and office environments.
Guidance for Dental Settings: interim infection prevention and control guidance for dental settings during the coronavirus disease (COVID-19) pandemic.
,
ADA interim guidance for minimizing risk of COVID-19 transmission.
These guidelines and other local interim guidance documents broadly agree, but the degree to which the US dental profession is aware of and adheres to these recommendations remains unknown. Furthermore, baseline data evaluating infection rates among dentists throughout the US are not widely known because CDC surveillance groups dental professionals with all other health care personnel.
CDC COVID data tracker: maps, charts, and data provided by the CDC—United States COVID-19 cases and deaths by state.
Guidance for Dental Settings: interim infection prevention and control guidance for dental settings during the coronavirus disease (COVID-19) pandemic.
,
ADA interim guidance for minimizing risk of COVID-19 transmission.
Methods
COVID-19 economic impact: survey results.
they reported that they would be willing to participate in a study on symptoms, testing, or diagnosis of COVID-19. In total, 5,479 dentists received an invitation to participate in the survey on June 8, 2020; a reminder invitation e-mail was sent June 11, 2020.
Coronavirus disease 2019 (COVID-19): cases, data, & surveillance—purpose and methods.
The survey also asked respondents to identify symptoms experienced in the past month (defined as since May 8, 2020), health conditions associated with COVID-19 severity,
Coronavirus disease 2019 (COVID-19): people at increased risk—and other people who need to take extra precautions, people at increased risk for severe illness.
and dental and nondental activities in the past month.
- Löwe B.
- Wahl I.
- Rose M.
- et al.
,
Welcome to the Patient Health Questionnaire (PHQ) Screeners.
Respondents who reported providing oral health care in the past month were asked about infection prevention or control procedures in their primary dental practice. Respondents indicated which personal protective equipment (PPE) they used when treating patients in the past month and whether they used it sometimes or always. The CDC interim guidance document was used to categorize PPE use,
Guidance for Dental Settings: interim infection prevention and control guidance for dental settings during the coronavirus disease (COVID-19) pandemic.
and respondents were categorized as following PPE guidance for AGDP if, in addition to basic clinical PPE of gloves and protective clothing, they “always” wore an N95 or similarly protective respirator (also called an “N95 mask”) with eye protection, or the highest level of surgical face mask available with a full-face shield. Dentists who performed no AGDP were categorized as following PPE guidance if they “always” wore gloves, protective clothing, a surgical mask, and eye protection. Occupational Safety and Health Administration guidance was used to categorize the risk of transmitting SARS-CoV-2 to dental providers or patients.
COVID-19: control and prevention—dentistry workers and employers.
Finally, respondents who reported wearing respirators or masks were asked how often they changed them. The ADA Institutional Review Board approved the research protocol and survey, which are registered at ClinicalTrials.gov (NCT04423770).
All statistical analysis was conducted in Stata software, Version 14.0 (StataCorp). For COVID-19 prevalence, statistical weighting was performed using linearization variance estimation so that the sample appropriately represented licensed US dentists in private practice or public health according to age group and US Census Bureau division. The weights and information on age, race or ethnicity, gender, dental specialty, and US Census Bureau division for all licensed US dentists in private practice or public health came from the ADA master file of all dentists (ADA members and nonmembers) in the United States. Dentist records are updated weekly through state licensure databases, death records, ADA surveys of dentists, and other sources. The data used for weighting in our study were extracted from the ADA master file on June 25, 2020. Differences between continuous variables were tested using analysis of variance and between categorical variables using χ2 tests, with statistical significance set at .05. Single and multivariable logistic regression models were used to test for associations between age category, race or ethnicity, gender, dental practice type, dental specialty, medical conditions, and confirmed or probable SARS-CoV-2 infection. Due to complex survey question skip patterns and because respondents were able to skip any question or stop answering the survey at any time, not all respondents answered all questions. The percentage of missing answers ranged from 2.0% through 3.5% per question.
Results
Participant characteristics
Coronavirus disease 2019 (COVID-19): people at increased risk—and other people who need to take extra precautions, people at increased risk for severe illness.
The most common conditions were asthma (7.3%) and obesity (7.6%). Compared with all dentists licensed in the United States in private practice or public health, higher proportions of survey respondents were aged 40 through 69 years, and fewer were 39 years or younger and 70 years or older (Table 1). Compared with dentists nationally, survey respondents were more likely to come from certain US Census Bureau divisions, be non-Hispanic white, female, or a general dentist.
Table 1Characteristics of the survey sample and comparison with all private practice or public health dentists licensed in the United States.
Symptoms among dentists
A total of 414 dentists (19.5%) scored 3 or higher on the anxiety symptom questions (mean [standard error], 1.42 [0.04]), indicating potential generalized anxiety disorder, a significantly lower proportion than in the general population (25.5%)
(P
- Löwe B.
- Wahl I.
- Rose M.
- et al.
Table 2Dentists’ self-reported symptoms and activities outside of their households in the month before survey administration.
Activities outside the household
Dental practice and infection control
Table 3Self-reported infection prevention and control efforts by dentists who practiced in the month before survey administration.
PPE
Guidance for Dental Settings: interim infection prevention and control guidance for dental settings during the coronavirus disease (COVID-19) pandemic.
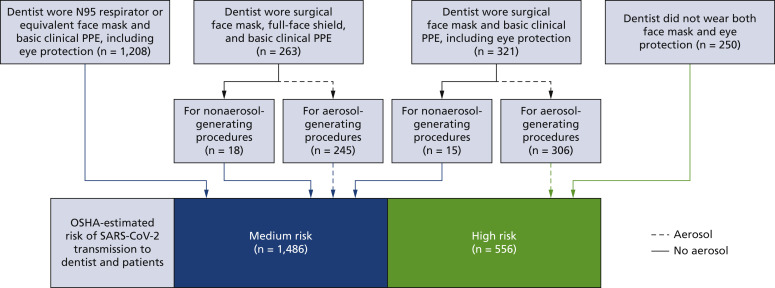
Of the 146 dentists who reported performing non-AGDP in the past month, 82.9% (n = 121) always wore masks, basic clinical PPE, and eye protection (Figure). During AGDP with patients assumed to be noncontagious, interim guidance suggests use of a fitted N95 or equivalent mask and basic clinical PPE, including eye protection; 59.0% of dentists (n = 1,117) who reported performing AGDPs in the past month always wore this combination of PPE, and 61.6% (n = 90) dentists reported wearing this during non-AGDP. If N95 or equivalent masks are not available, the CDC interim guidance recommends using both the highest-level surgical face mask available and a full-face shield during AGDPs
Guidance for Dental Settings: interim infection prevention and control guidance for dental settings during the coronavirus disease (COVID-19) pandemic.
; 12.9% of dentists (n = 245) performing AGDPs used this combination of PPE, as did 12.3% (n = 18) dentists during non-AGDP. In all, 72.8% (n = 1,486) of dentist respondents used PPE according to CDC interim guidance.
Guidance for Dental Settings: interim infection prevention and control guidance for dental settings during the coronavirus disease (COVID-19) pandemic.

FigurePersonal protective equipment (PPE) always worn in past month, according to dental procedure. OSHA: Occupational Safety and Health Administration. SARS-CoV-2: Severe acute respiratory syndrome coronavirus 2.
COVID-19: economic impact on dental practices—week of June 1 results.
Some respondents (17.6%, n = 355) reported changing masks in between patients. More commonly, dentists changed masks between multiple patients (20.2%; n = 407), daily (34.2% , n = 689), weekly (7.7%, n = 155), or only if soiled or damaged (20.2%, n = 407). Respondents also wrote in to report that they used multiple masks simultaneously, with surgical masks worn over N95 or equivalent masks, and replaced the surgical masks more often.
Confirmed or probable COVID-19 among dentists
Among respondents, 16.6% (n = 355) reported that they had been tested for SARS-CoV-2 with at least 1 testing type. Fifty-one respondents (2.3%) were tested with 2 testing types—50 (2.3%) with both blood and nasal or throat swab tests and 1 (0.05%) with saliva and nasal or throat swab tests. A total of 244 respondents (11.1%) were tested with a nasal or throat swab, of which 9 (3.7%) tested positive. One hundred and fifty-six respondents (7.1%) were tested with a blood sample, and 4 (2.7%) had a positive result. Six respondents (0.3%) were tested for SARS-CoV-2 using a saliva sample and 0 had a positive result. Because testing was not widely available during this time, respondents were also asked whether they had received a diagnosis of probable COVID-19 infection and 7 (0.3%) had. Twenty dentists (0.9%) in this sample had either confirmed or probable COVID-19 cases. Weighted to approximate the age and location of licensed private practice and public health dentists nationally, the estimated prevalence of confirmed or probable COVID-19 among dentists was 0.9% (95% confidence interval, 0.5 to 1.5). The likely source of SARS-CoV-2 transmission was identified via contact tracing through a health agency or clinic in only 5 cases, and in none of those cases was the source of transmission the dental practice.
Association between COVID-19 and personal characteristics
Interim guidelines for COVID-19 antibody testing: interim guidelines for COVID-19 antibody testing in clinical and public health settings.
a sensitivity analysis was conducted that excluded COVID-19 cases confirmed with antibody tests only. This analysis similarly found no statistically significant associations with age, gender, race or ethnicity, dental practice type, dental specialty, or US Census Bureau division (all χ2P > .2). However, there was a statistically significant association between antigen or viral confirmed or health care provider–suspected COVID-19 cases and patient-reported immunocompromised status. Specifically, 0.9% (n = 17) of COVID-19 negative dentists were immunocompromised compared with 6.3% (n = 1) of COVID-19 positive dentists (χ2P = .02).
Discussion
- Kluytmans-van den Bergh M.F.
- Buiting A.G.
- Pas S.D.
- et al.
and China (1.1%),
- Lai X.
- Wang M.
- Qin C.
- et al.
but lower than the rate in Seattle, Washington (5.3%).
Mani NS, Budak JZ, Lan KF, et al. Prevalence of COVID-19 infection and outcomes among symptomatic healthcare workers in Seattle, Washington [published online ahead of print June 16, 2020]. Clin Infect Dis. https://doi.org/10.1093/cid/ciaa761.
Furthermore, in our sample, 3.7% of nasal or throat swabs tested positive, which is lower than the 10.3% positivity in respiratory specimens from the broader US population from March 1, 2020 through June 13, 2020.
COVIDView summary ending on June 13, 2020.
This might reflect the higher socioeconomic status of many dentists and their subsequent ability to use social distancing and mitigate viral exposure.
Guidance for Dental Settings: interim infection prevention and control guidance for dental settings during the coronavirus disease (COVID-19) pandemic.
As of June 29, 2020, patient volume in dental practices nationwide was estimated to be 70% of pre–COVID-19 levels, and it has been increasing steadily.
COVID-19 economic impact: survey results.
Use of disposable products for PPE and infection control might increase if patient volume increases, which could result in scarcity or alteration of practices within dental offices based on availability. In addition, changes in local and regional ordinances and infection rates might also alter practices within dental offices moving forward, particularly as COVID-19 cases resurge in many states.
Coronavirus resource center: impact of opening and closing decisions by state—a look at how social distancing measures may have influenced trends in COVID-19 cases and deaths.
- Fang L.
- Karakiulakis G.
- Roth M.
Angiotensin-converting enzyme 2 is upregulated in the presence of certain systemic diseases.
but nonrespondents might differ from respondents, which can reduce the validity and generalizability of these results. The survey sample might also be subject to selection bias, leading to an underestimation of COVID-19 prevalence or severity because dentists who have died or been hospitalized with COVID-19, for example, cannot or might be less likely to participate. Due to the limited availability of COVID-19 tests in the United States,
it is possible respondents had limited access to COVID-19 testing and might have had undiagnosed infections. Furthermore, these findings are only as accurate as the COVID-19 tests and diagnoses themselves, which can be subject to false-negative and false-positive results.
- Woloshin S.
- Patel N.
- Kesselheim A.S.
There might be recall bias in the questions that asked about activities and symptoms in the past month. It is likely that respondents reported higher levels of social distancing and infection prevention and control compliance due to social desirability bias and unrecognized lapses in PPE usage. These cross-sectional data were also limited in that the timing of known SARS-CoV-2 infections in this survey sample precluded testing for associations with symptoms, activities, or infection prevention and control efforts.
Guidance for Dental Settings: interim infection prevention and control guidance for dental settings during the coronavirus disease (COVID-19) pandemic.
,
Subsequently, the number of dental patients seen and procedures conducted in the United States dropped.
COVID-19 economic impact: survey results.
In this survey sample, 75.0% (n = 15) of dentists with presumed or confirmed COVID-19 tested positive in March or April, when 95% of US dental practices were closed or provided only emergency oral health care.
COVID-19 economic impact: survey results.
Subsequent surveys sent to the cohort described in our study will continue to collect COVID-19 test results, symptoms, activities, and infection prevention and control efforts in dental practices. Future research in this cohort might therefore be able to estimate COVID-19 incidence, as well as associations with dental activities and infection prevention or control efforts.
Conclusions
This survey was conducted to initiate surveillance of licensed, practicing dentists and public health dentists to determine the prevalence of COVID-19 before June 12, 2020, as well as the behavioral and infection control and prevention practices of dentists from May 8, 2020 through June 12, 2020. To our knowledge, this is the first study to estimate the prevalence of COVID-19 among US dentists. For this sample of dentists, the weighted prevalence of COVID-19 was 0.9%. Among the tested respiratory samples, 3.7% had positive results. These rates support that use of the CDC’s currently recommended infection prevention and control procedures in dental offices will contribute to the reduced risk of developing infection during the delivery of oral health care, and risks associated with nonclinical activities and community spread might pose the most substantial risks for the exposure of dentists to COVID-19. Future investigations will assess ongoing rates of COVID-19 for US dentists and can assess modifiable risk factors for SARS-CoV-2 transmission and development of COVID-19 disease, in addition to defining incidence rates of disease.
Supplemental Data
References
How COVID-19 spreads.
()
Projecting the transmission dynamics of SARS-CoV-2 through the postpandemic period.
Science. 2020; 368: 860-868
Reducing transmission of SARS-CoV-2.
Science. 2020; 368: 1422-1424
Presymptomatic transmission of SARS-CoV-2: Singapore, January 23-March 16, 2020.
MMWR Morb Mortal Wkly Rep. 2020; 69: 411-415
Transmission routes of respiratory viruses among humans.
Curr Opin Virol. 2018; 28: 142-151
Aerosols and splatter in dentistry: a brief review of the literature and infection control implications.
JADA. 2004; 135: 429-437
Coronavirus disease 2019 (COVID-19): emerging and future challenges for dental and oral medicine.
J Dent Res. 2020; 99: 481-487
Guidance for Dental Settings: interim infection prevention and control guidance for dental settings during the coronavirus disease (COVID-19) pandemic.
()
ADA interim guidance for minimizing risk of COVID-19 transmission.
() ()
CDC COVID data tracker: maps, charts, and data provided by the CDC—United States COVID-19 cases and deaths by state.
()
COVID-19 economic impact: survey results.
()
Coronavirus disease 2019 (COVID-19): cases, data, & surveillance—purpose and methods.
()
Coronavirus disease 2019 (COVID-19): people at increased risk—and other people who need to take extra precautions, people at increased risk for severe illness.
()
A 4-item measure of depression and anxiety: validation and standardization of the Patient Health Questionnaire-4 (PHQ-4) in the general population.
J Affect Disord. 2010; 122: 86-95
Welcome to the Patient Health Questionnaire (PHQ) Screeners.
()
COVID-19: control and prevention—dentistry workers and employers.
()
Mental health, substance use, and suicidal ideation during the COVID-19 pandemic: United States, June 24-30, 2020.
MMWR Morb Mortal Wkly Rep. 2020; 69: 1049-1057
COVID-19: economic impact on dental practices—week of June 1 results.
()
Interim guidelines for COVID-19 antibody testing: interim guidelines for COVID-19 antibody testing in clinical and public health settings.
()
Prevalence and clinical presentation of health care workers with symptoms of coronavirus disease 2019 in 2 Dutch hospitals during an early phase of the pandemic.
JAMA Network Open. 2020; 3e209673
Coronavirus disease 2019 (COVID-2019) infection among health care workers and implications for prevention measures in a tertiary hospital in Wuhan, China.
JAMA Network Open. 2020; 3e209666
Mani NS, Budak JZ, Lan KF, et al. Prevalence of COVID-19 infection and outcomes among symptomatic healthcare workers in Seattle, Washington [published online ahead of print June 16, 2020]. Clin Infect Dis. https://doi.org/10.1093/cid/ciaa761.
COVIDView summary ending on June 13, 2020.
()
Coronavirus resource center: impact of opening and closing decisions by state—a look at how social distancing measures may have influenced trends in COVID-19 cases and deaths.
()
Are patients with hypertension and diabetes mellitus at increased risk for COVID-19 infection?.
Lancet Respir Med. 2020; 8: e21
E-mail survey response rates: a review.
J Comput Mediat Commun. 2001; 6
COVID-19 testing problems started early, U.S. still playing from behind.
() ()
False negative tests for SARS-CoV-2 infection: challenges and implications.
N Engl J Med. 2020; 383: e38
ADA recommending dentists postpone elective procedures. ADA News. March 16, 2020.
() ()
Biography
Dr. Estrich is a health research analyst, Evidence Synthesis and Translation Research, ADA Science and Research Institute, 211 E. Chicago Ave, Chicago, IL 60611.
Biography
Mr. Mikkelsen is a manager, Education Surveys, Health Policy Institute, American Dental Association, Chicago, IL.
Biography
Ms. Morrissey is a research analyst, Education, Health Policy Institute, American Dental Association, Chicago, IL.
Biography
Dr. Geisinger is a professor, Advanced Education Program in Periodontology; and the director, UAB Faculty Development and Support, Department of Periodontology, University of Alabama at Birmingham, Birmingham, AL.
Biography
Dr. Ioannidou is a professor of oral health and diagnostic sciences and the director, Dental Clinical Research Center, University of Connecticut, Farmington, CT.
Biography
Dr. Vujicic is the chief economist and vice president, Health Policy Institute, American Dental Association, Chicago, IL.
Biography
Dr. Araujo is the chief science officer, American Dental Association; the chief executive officer, ADA Science and Research Institute, American Dental Association; and the chief executive officer, American Dental Association Foundation, Chicago, IL.
Article Info
Publication History
Accepted:
September 10,
2020
Received in revised form:
September 9,
2020
Received:
July 16,
2020
Footnotes
Disclosure. None of the other authors reported any disclosures.
The authors thank all of the dentists who participated in this survey and shared their time and expertise, and Adriana Menezes and Dr. Ruth Lipman for their advice and insights.
Identification
DOI: https://doi.org/10.1016/j.adaj.2020.09.005
Copyright
© 2020 American Dental Association.
User License
Creative Commons Attribution – NonCommercial – NoDerivs (CC BY-NC-ND 4.0) |

Permitted
For non-commercial purposes:
- Read, print & download
- Redistribute or republish the final article
- Text & data mine
- Translate the article (private use only, not for distribution)
- Reuse portions or extracts from the article in other works
Not Permitted
- Sell or re-use for commercial purposes
- Distribute translations or adaptations of the article
Elsevier’s open access license policy
ScienceDirect
Access this article on ScienceDirect