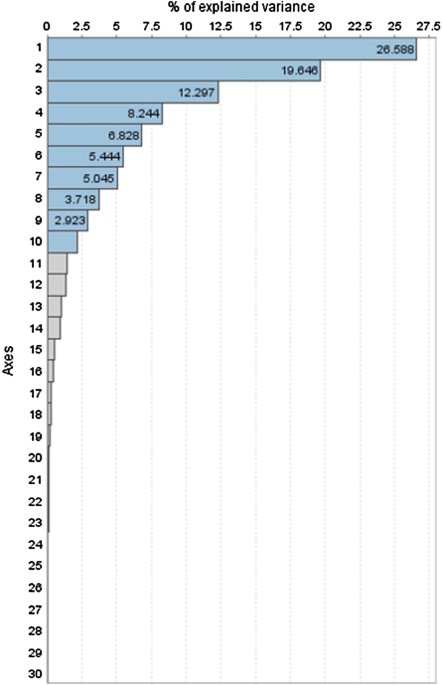
In the present study, 6 different types of class III skeletal malocclusion phenotypes and 10 main components were obtained using grouping techniques. Both approaches, principal component generation and morphological class III cluster generation, form part of a sequential process in which the principal component axes are not real biological coordinates of the system but a means of grouping the variables for later construction of the class III clusters. Specifically, the analysis of the main components facilitated the generation of 10 axes, which were constructed exclusively from the 55 skeletal measurements of the subjects of the study. This allowed for extremely high coverage of variance (92.7% of the variance). We found differences in the size of the axis models generated compared with previously published studies5,8,17, which restricted the number of main components to five17 and six5,8, respectively, and covered 67%17 to 81.2%5 of total variance in their sample. This may be because in the present study, only skeletal measurements were considered for the axis model generation.
Dental and soft tissue measurements were excluded to avoid potential interactions with the construction of the purely skeletal class III clusters, as these parameters could modify or mask the underlying craniofacial structure12. Hence, using a large number of critical measurements, 55 skeletal variables, we achieved a notable percentage of explained variation, which, although not excellent, shows minimal loss of information, which might be of critical importance for the configuration of skeletal clusters, although assuming, as with other diagnostic methods, that some uncovered features would be underrepresented.
As described in previously published studies5,8,17, the first three axes represented more than half [58.5%] of the total variation found in the sample, essentially referring to the description of sagittal and vertical parameters, while others5,8,17 also represented the position of the lower incisor in the first half of the variation derived from the involvement of dental variables in the formation of PCs. Most of the parameters that represent sagittal and vertical measurements in our PC1 (26.6% of variation), PC2 (19.6% of variation), and PC3 (12.3% of variation) are equivalent to the parameters of PC1 (23.7% and 20.6%) and PC2 (17.3% and 19.34%) in other studies5,8, while PC1 in another study17 is more like PC4 (9.3%) and PC5 (6.5%) (ANB, facial angle, and Pg-N perp) in the present research, despite the fact that the same sagittal and vertical parameters were included in these aforementioned components. The observed differences might be at least partially explained by the type of class III patients included and their distribution, essentially based on distinct ethnic origin and growing stage of the included subjects.
The 10 main models enabled the subsequent generation of skeletal class III malocclusion sub-phenotypes or clusters. According to the dendrogram analysis, potential construction with three or six skeletal clusters was possible (Fig. 2). Nevertheless, a six-cluster skeletal model was selected, since we observed substantial loss of representation of clearly detailed sub-phenotypes in the three-cluster model, such as C2 representing a vertical cluster with bimaxillary retrusion, or C4 representing maxillary hypoplasia with a prognathic mandible. The number of clusters found in previous studies that also used cluster analysis focusing on class III malocclusion classification varied between 48 and 7 clusters2, very close to the number of clusters established in the present research. Despite this, we also observed in the literature other studies with even more clusters than those found in our study, varying between 33,6,7 and 14 clusters4, which might provide high variation in coverage but completely lose efficiency in terms of practical utility in clinical settings. Other authors3,4,6,7 used a diffuse cluster analysis when establishing a three-cluster model6,7, implying that the elements of analysis may belong to more than one cluster, while others used a hierarchical cluster analysis3 instead of the mixed cluster analysis used in the present research.
However, with respect to 14 different clusters4, the increased number of clusters could be derived, at least in part, from the inclusion of class III dental malocclusions as well as skeletal class III malocclusions, and the classification was also used to evaluate the effects of treatment4, which required large numbers in order to provide enough patients in each sub-group, while at the same time ensuring potentially higher homogeneity in intersubject characteristics in each of the constructed groups.
With respect to the skeletal clusters generated in the present research, the cluster representing the highest percentage of the sample was C3, at 33%. This cluster was characterized by a mesofacial pattern (y-axis: 66.7 ± 2.1, SN-GoGn: 29.0 ± 3.2, and NBa-PtGn: 90.1 ± 2.7) with slight maxillary retrusion (convexity: − 2.1 ± 1.4) and a slight anterior mandibular position (PgN perp: 5.4 ± 4.1) but with decreased total mandibular size (GoGn: 79.4 ± 3.9, GoPg: 69.8 ± 3.4, and CoGn: 114.4 ± 5.1) than the rest of the clusters. The characteristics of this cluster were similar to those found in C2 clusters in previous studies5, which was one of the most representative clusters in their sample. In the same research5 and a previous study17, the group with the highest number of subjects was represented by a group characterized by a retrusive jaw (C5 and C3, respectively). In our study, the retrusive jaw model was the second most representative model in the sample (C2), representing 18.8% of the total sample. In another study, on the other hand, the model with maxillary deficiency alone, but without mandibular compromise, was not represented8. Interestingly, this must have derived from the ethnic origin of the sample population, since in studies that analyzed Caucasian subjects5 and even a mixed sample with the highest percentage of subjects being of Caucasian origin17, this type of cluster was represented, as in the present research. In contrast, clusters generated from samples of Asiatic origin did not generate this type of sub-phenotype8, which clearly demonstrates the morphological differences between ethnic groups11,18,19 and even between different populations of the same ethnic group when it comes to analyzing class III malocclusion sub-phenotypes.
In our study, the soft tissue, dental, and airway variables were excluded to avoid an inadequate interpretation of the generated groups, since it has been observed that soft tissues do not closely follow bone structures12. Despite this, several common characteristics related to the skeletal parts and soft tissues were observed.
In this respect, the soft tissue of the chin continued the underlying bone structure in the 6 sub-phenotypes found. Similarly, lower facial height in soft tissues (Sn’-Me’) and hard tissues (ANS-Me) coincided in 4 (C1, C3, C4, and C6) of the 6 clusters. Conversely, skeletal facial height in C2 (69.89 ± 5.30) was 0.09 mm higher than in C5 (69.80 ± 3.45), but facial height in soft tissues (72.23 ± 5.06) was 0.73 mm lower than in C5 (72.96 ± 3.78). Despite this slight difference, our results agree with previous observations12, which concluded that the soft tissue of the lower facial third continues the skeletal profile, but not in the labial region12. In this study, as observed in previous ones20,21,22, a more significant relationship was found between the labial tissue and the position of the incisors.
The position of the lower lip with respect to the lower incisor was analyzed in several studies that found a close relationship between the two23,24, even observing a more significant relationship in the position of the lower incisor with respect to the lower lip compared to the relationship between the upper incisor and the upper lip23. This study found that in 5 of the 6 sub-groups, the position of the lower lip coincided with the position of the lower incisor. In the case of C6, the most retruded position of the lower incisor was observed with both the NB line (1.1 ± 2.3) and A-Pg (0.84 ± 2.62), coinciding with the most retruded position of the lower lip with respect to the S line (− 2.62 ± 2.22) and E line (− 5.29 ± 2.43). The relationship between the position of the lower incisor with the NB plane or A-Pg plane with respect to the position of the lower lip with the S line and/or E line was observed in C5, C4, C3, and C2, but not in C1. Individual characteristics may lead to different soft tissue behaviors with respect to the bones and/or teeth23,24,25, with different correlations between the two components. The method used for the analysis of soft tissues should also be taken into account, since recent studies support the need to conduct this analysis using facial photographs, since skeletal cephalometry and soft tissue cephalometry lead to different diagnoses of the patient’s facial characteristics23.
Due to the considerable variations, caution must be taken when analyzing the soft profile, especially at the labial level. Parameters such as labial thickness or nasal size, which can vary widely in each individual25 and do not follow a skeletal pattern26, cannot be ignored. These variations, not only individual, but also soft tissue variations between genders25, can lead to a distortion of the final labial position.
In previously published articles3,5,6,7,8,17 that conducted this type of classification of skeletal class III malocclusion, the samples contained similar gender percentages to our own sample: 40.8% were males and 58.6% were females. In other studies, the gender mix in the total sample ranged from 40.2%8 to 48.7%3 for males, and between 51.3%3 and 59.7%8 for females. Only one of the aforementioned studies8 mentioned the gender percentage in each of the clusters found: two of the groups found in that study (C3 and C4) had substantially higher distributions of women than men. In our study, we observed another 3 clusters in which the difference in the female/male ratio was greater than 40% (C1: 14.3/85.7, C3: 74.3/25.7, and C5: 20.6/79.4). Although both clusters followed a similar trend in terms of gender distribution, a thorough analysis of the cluster characteristics found some differences in the configuration of skeletal structures derived from ethnicity of Asiatic and Caucasian origin18,27,28.
Beyond differences in ethnicity and gender, skeletal class III malocclusion is strongly linked to genetic components and environmental factors29. Current phenotype and genotype studies of this malocclusion30,31,32,33 have been reported in the literature to develop preventive and therapeutic advances in these patients34,35. Recent studies in the field of medicine focus on the search for preventive measures and individualized treatments based on the patient’s morphological and genetic components34,36,37,38. However, this will require future research, larger samples, and collaborative multicenter studies5 to better understand the differences between regions and environmental factors involved. To reach this point, and bearing in mind that the distribution and frequencies of some specific genetic variations can differ substantially between different populations39, it is imperative to obtain an accurate and precise classification in the sub-phenotype diagnosis of each population and/or ethnic group. The present research offers significant data on skeletal class III malocclusion sub-phenotyping in subjects of southern European origin. To the best of our knowledge, this is the first scientific evidence in the field of skeletal clusters of subjects of European origin affected by class III malocclusion.