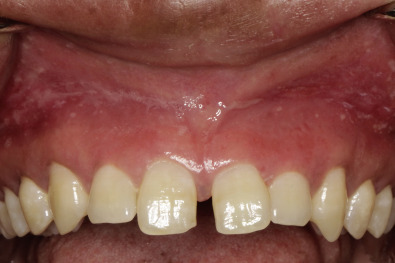
Dermatology, Dwight David Eisenhower Army Medical Center, having developed allergic
responses to multiple foods and persistent firm swelling of the lips. The patient
had moved to Augusta, Georgia, in July 2018 and was completely well at that time.
He reported no history of systemic disease and had never smoked. Social and family
histories were noncontributory. The patient denied having any relative diagnosed with
inflammatory bowel disease. With the exception of an elevated eosinophil fraction
(9.4%), results of the patient’s complete blood cell count with differential and comprehensive
metabolic panel were normal. Allergen-specific serum immunoglobulin E testing revealed
allergies to an extensive list of foods, plants, and other substances (Table 1). Table 2 presents additional laboratory values. On chest radiographs (posteroanterior and
lateral views), the cardiomediastinal silhouette and pulmonary vasculature were unremarkable,
with no acute osseous or soft-tissue abnormalities. The patient received a full evaluation
in the Department of Gastroenterology. Colonoscopy did not reveal any abnormal findings,
and the patient’s fecal calprotectin level, a marker for intestinal inflammation,
was only mildly elevated (62 micrograms per gram).
Table 1Allergen-specific serum immunoglobulin E values for the presented case.
| SERUM IMMUNOGLOBULIN E ANTIBODY | VALUE (KILOUNITS PER LITER) ∗ ∗ Scale: < 0.35, negative; 0.35-0.70, low positive; 0.71-3.50, moderate positive; 3.50-16.99, |
|---|---|
| Trees | |
| Cottonwood | 5.54 |
| Elm | 9.55 |
| Oak | 5.96 |
| Sycamore | 6.72 |
| Boxelder | 4.82 |
| Australian pine | 5.72 |
| Walnut | 9.28 |
| White ash | 17.60 |
| Birch | 5.39 |
| Sweetgum | 2.91 |
| Hackberry | 2.87 |
| Hickory | 2.52 |
| Willow | 3.84 |
| Mulberry | 4.36 |
| Grass | |
| Bahia grass | 18.10 |
| Bermuda grass | 10.50 |
| Johnson grass | 15.70 |
| Kentucky blue grass | 20.50 |
| Perennial rye grass | 14.10 |
| Timothy grass | 11.50 |
| Weeds | |
| Cocklebur | 9.77 |
| Lamb’s-quarter | 2.96 |
| Ragweed | 12.80 |
| Mugwort | 10.70 |
| Elder marsh rough | 5.66 |
| Pigweed rough | 3.45 |
| English plantain | 4.72 |
| Russian thistle | 5.36 |
| Nettle | 2.62 |
| Lenscale | 3.45 |
| Sheep sorrel | 3.51 |
| Firebush | 2.61 |
| Molds | |
| Alternaria alternata | 26.70 |
| Curvularia lunata | 10.90 |
| Aspergillus fumigatus | 9.04 |
| Cladosporium herbarum | 7.41 |
| Epicoccum purpurascens | 28.00 |
| Helminthosporium halodes | 29.50 |
| Mucor racemosus | 1.23 |
| Penicillium chrysogenum | 3.50 |
| Foods | |
| Wheat | 5.16 |
| Oat | 5.88 |
| Rice | 7.62 |
| Apple | 6.42 |
| Peach | 3.37 |
| Orange | 1.83 |
| Chocolate | < 0.10 |
| Milk | 2.40 |
| Egg | 0.50 |
| Soy | 3.17 |
| Corn | 4.18 |
| Peanut | 7.48 |
| Almond | 4.41 |
| Brazil nut | 0.84 |
| Cashew | 0.78 |
| Hazel nut | 4.20 |
| Pecan | 0.67 |
| Pistachio | 3.79 |
| Sesame seed | 10.60 |
| Sunflower seed | 2.61 |
| Walnut | 8.99 |
| Nutmeg | < 0.10 |
| Codfish | 0.38 |
| Salmon | 0.77 |
| Tilapia | 0.50 |
| Tuna | 0.25 |
| Shrimp | 21.00 |
| Crab | 27.90 |
| Lobster | 16.60 |
| Clam | 0.70 |
| Oyster | 1.85 |
| Chicken meat | 0.23 |
| Pork | 0.18 |
| Turkey meat | 0.22 |
| Other | |
| Dermatophagoides | 3.57 |
| Cat dander | 15.40 |
| Cockroach | 22.20 |
| Dog dander | 19.10 |
∗ Scale: < 0.35, negative; 0.35-0.70, low positive; 0.71-3.50, moderate positive; 3.50-16.99,
high positive; > 17.00, very high positive.
Table 2Laboratory values for the presented case.
| TEST | SPECIMEN TYPE | VALUE (NORMAL RANGE) | INTERPRETATION |
|---|---|---|---|
| Angiotensin-converting enzyme | Serum | 40 (14-82) kilounits per liter | Normal |
| Coccidioides | Serum | Negative | Normal |
| Histoplasma capsulatum | Serum | Negative | Normal |
| Treponema pallidum (rapid plasma reagin titer) | Serum | Nonreactive | Normal |
| Immunoglobulin E | Serum | 1,702 (0-127) kU/L | High |
| Immunoglobulin G | Serum | 1,330 (700-1,600) milligrams per deciliter | Normal |
| Immunoglobulin G subclass 1 | Serum | 805 (248-810) mg/dL | Normal |
| Immunoglobulin G subclass 2 | Serum | 299 (130-555) mg/dL | Normal |
| Immunoglobulin G subclass 3 | Serum | 59 (59-102) mg/dL | Normal |
| Immunoglobulin G subclass 4 | Serum | 69 (2-96) mg/dL | Normal |
| Nuclear antibody screen | Serum | Negative | Normal |
| C-reactive protein | Serum | 0.4 (0.2-8.0) mg/liter | Normal |
| Erythrocyte sedimentation rate | Serum | 12 (0-15) millimeters per hour | Normal |
| Antineutrophil cystoplasmic antibodies vasculitides, proteinase 3 antibody | Serum | < 3.5 (0.0-3.5) units per milliliter | Normal |
| Antineutrophil cytoplasmic antibodies vasculitides, myeloperoxidase antibody | Serum | < 9 (0.0-9.0) U/mL | Normal |
| Complement C1q | Serum | 12.6 (11.8-23.8) mg/dL | Normal |
| Complement C1 esterase inhibitor | Serum | 26 (21-39) mg/dL | Normal |
| Complement C1 esterase inhibitor functional | Serum | > 109 (> 67) mg/dL | Normal |
| Tryptase | Serum | 4.7 (2.2-13.2) micrograms per liter | Normal |
| Chronic Urticaria Index | Serum | < 2.5 (< 10) | Normal |
| Calprotectin | Stool | 62 (10-60) micrograms per gram | Marginally elevated |
To read this article in full you will need to make a payment
References
Orofacial granulomatosis: clinical study of 20 patients.
Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2012; 113: e12-e17
Oral Crohn’s disease: is it a separable disease from orofacial granulomatosis? A review.
J Crohns Colitis. 2012; 6: 135-142
Distinguishing orofacial granulomatosis from Crohn’s disease: two separate disease entities?.
Inflamm Bowel Dis. 2011; 17: 2109-2115
Orofacial granulomatosis: review on aetiology and pathogenesis.
J Oral Pathol Med. 2008; 37: 191-195
Clinical evidence for allergy in orofacial granulomatosis and inflammatory bowel disease.
Clin Transl Allergy. 2013; 3: 26
Patch testing for food-associated allergies in orofacial granulomatosis.
J Oral Pathol Med. 2011; 40: 10-13
Contact orofacial granulomatosis caused by delayed hypersensitivity to gold and mercury.
J Am Acad Dermatol. 2003; 49: 1117-1120
The diagnosis of sarcoidosis.
Clin Chest Med. 2008; 29: 415-427
Etiologies of sarcoidosis.
Clin Rev Allergy Immunol. 2015; 49: 6-18
Sarcoidosis: a comprehensive review and update for the dermatologist, part I—cutaneous disease.
J Am Acad Dermatol. 2012; 66: 699.e1-699.e18
Atopic status in patients with sarcoidosis.
Allergy Asthma Proc. 2005; 26: 121-124
Unravelling the pathogenesis of inflammatory bowel disease.
Nature. 2007; 448: 427-434
Oral and upper gastrointestinal Crohn’s disease.
J Gastroenterol Hepatol. 2018; 33: 355-364
Mycobacterium tuberculosis pathogenesis and molecular determinants of virulence.
Clin Microbiol Rev. 2003; 16: 463-496
Syphilis: review with emphasis on clinical, epidemiologic, and some biologic features.
Clin Microbiol Rev. 1999; 12: 187-209
Chronic granulomatous disease.
Clin Rev Allergy Immunol. 2010; 38: 3-10
Foreign body-type multinucleated giant cell formation is potently induced by α-tocopherol and prevented by the diacylglycerol kinase inhibitor R59022.
Am J Pathol. 2003; 163: 1147-1156
IgE-mediated food allergy: extensive review of the literature.
Acta Clin Belg. 2001; 56: 234-247
Angioedema.
J Am Acad Dermatol. 2005; 53: 373-388
International consensus on hereditary and acquired angioedema.
Ann Allergy Asthma Immunol. 2012; 109: 395-402
Perioral angioedema associated with angiotensin-converting enzyme inhibitor.
J Periodontol. 2005; 76: 651-654
Biography
Dr. Bunting is a resident, Department of Periodontics, Army Postgraduate Dental School, Uniformed Services University of the Health Sciences, Fort Gordon, GA.
Biography
Dr. Hawie is an assistant professor, Department of Oral Pathology, Army Postgraduate Dental School, Uniformed Services University of the Health Sciences, Fort Gordon, GA.
Biography
Dr. Lancaster is an associate professor, Department of Periodontics, Army Postgraduate Dental School, Uniformed Services University of the Health Sciences, Fort Gordon, GA.
Biography
Dr. Johnson is a professor, Department of Periodontics, Army Postgraduate Dental School, Uniformed Services University of the Health Sciences, 228 E Hospital Rd, Fort Gordon, GA 30905.
Article Info
Publication History
Published online: April 08, 2021
Accepted:
January 31,
2021
Received in revised form:
January 15,
2021
Received:
August 31,
2020
Publication stage
In Press Corrected Proof
Footnotes
Disclosure. None of the authors reported any disclosures.
Disclaimer. The US Army funded the treatment in the presented case. No extramural funding was associated with this report. The views and opinions expressed are solely those of the authors and do not reflect the official policy or position of the Dwight David Eisenhower Army Medical Center, the US Army, the Uniformed Services University of the Health Sciences, the Department of Defense, or the US government. The authors deny any conflicts of interest related to this study.
Diagnostic Challenge is published in collaboration with the American Academy of Oral and Maxillofacial Pathology and the American Academy of Oral Medicine.
ORCID Numbers. Megan E. Bunting: http://orcid.org/0000-0002-2463-3799. Jennifer B. Hawie: http://orcid.org/0000-0003-2091-1306. Douglas D. Lancaster: http://orcid.org/0000-0003-2231-0504. Thomas M. Johnson: http://orcid.org/0000-0001-8325-0803.
Identification
DOI: https://doi.org/10.1016/j.adaj.2021.01.015
Copyright
© 2021 Published by Elsevier Inc. on behalf of the American Dental Association.
ScienceDirect
Access this article on ScienceDirect