These ADRs typically range from mild to moderate, but excessive toxicity can occur, especially at higher doses, resulting in dose interruptions, dose reductions, and sometimes treatment discontinuation.
Imatinib is also associated with various cutaneous adverse effects (for example, photosensitivity, Stevens-Johnson syndrome, psoriasis, acute neutrophilic dermatosis)
- Macdonald J.B.
- Macdonald B.
- Golitz L.E.
- LoRusso P.
- Sekulic A.
and is not devoid of oral adverse effects.
- Poulopoulos A.
- Papadopoulos P.
- Andreadis D.
Oral lichenoid reactions,
- Poulopoulos A.
- Papadopoulos P.
- Andreadis D.
,
- Vigarios E.
- Epstein J.B.
- Sibaud V.
blue-gray asymptomatic hyperpigmentation of the hard palate,
- Vigarios E.
- Epstein J.B.
- Sibaud V.
,
oral melanosis,
- Yu Y.H.
- Shere Y.
- Vigneswaran N.
stomatitis,
- Cristofanilli M.
- Morandi P.
- Krishnamurthy S.
- et al.
,
- Li J.
- Wang M.
- Zhang B.
- et al.
Chinese consensus on management of tyrosine kinase inhibitor-associated side effects in gastrointestinal stromal tumors.
,
- Linga V.G.
- Ganta R.R.
- Kalpathi K.I.
- et al.
and taste disturbances
- van der Werf A.
- Rovithi M.
- Langius J.A.E.
- de van der Schueren M.A.E.
- Verheul H.M.W.
have all been reported. Imatinib can also disturb bone and mineral homeostasis, which is putatively a mechanism by means of which it causes osteonecrosis of the jaw.
- Nicolatou-Galitis O.
- Razis E.
- Galiti D.
- Vardas E.
- Tzerbos S.
- Labropoulous S.
,
- Okubo-Sato M.
- Yamagata K.
- Fukuzawa S.
- et al.
,
- Viviano M.
- Rossi M.
- Cocca S.
- Ronicke M.
- Erfurt-Berge C.
and cause wound disruption
(Table), although more definitive clinical studies are needed to confirm these findings. In another case report, discontinuation of imatinib before oral surgery may have improved surgical outcomes (Table), although the outcomes after no discontinuation of imatinib were not compared in this case report.
To our best knowledge, there are no published case reports on delayed gingival healing secondary to long-term imatinib therapy. We report an uncommon but potentially serious oral ADR likely related to imatinib therapy and discuss the clinical manifestation of a case with delayed gingival healing.
TableCase reports on imatinib’s interplay with wound healing.
Case Report
We report the case of a 58-year-old man who sought treatment in December 2020 at a prosthodontic clinic with a dislodged crown and core buildup and multiple recementations of tooth no. 19. The patient had a medical history of a gastrointestinal stromal tumor, which was surgically removed in 2019. He received no chemotherapy or radiation therapy afterward, but his oncologist prescribed 400 mg of imatinib orally daily. He was compliant with drug therapy for 16 months at the day he came to the dental clinic. No other medications or systemic conditions were noted.
Tooth no. 19 was treated endodontically, and the mesial root was ankylosed. The crown of tooth no. 19 had been dislodged several times. The patient consented to have the crown removed to determine restorability. The entire crown with core and cement were dislodged easily with no dentine ferrule. These findings were explained to the patient and a discussion of treatment options followed, including crown lengthening, post and core, and crown; implant; removable partial denture or overdenture; and no treatment. The advantages and disadvantages of each option were discussed at length. The patient consented for extraction of tooth no. 19, ridge preservation, and future implant placement.
Tooth no. 19 was surgically extracted in December 2020. The procedure included local anesthetic (mandibular nerve block and local infiltration) administered as 2% lidocaine with 1:100,000 epinephrine, intrasulcular incision at tooth no. 19, raised limited extent full-thickness flaps, and extraction of tooth no. 19 using Piezotome (Acteon), elevator, and forceps. The socket was curetted and irrigated with sterile water. The ridge was preserved with particulate allogenic bone graft (a mixture of mineralized and demineralized cortical bone; LifeNet Health), and the bone graft was covered with a Cytoplast (Osteogenics Biomedical) membrane. The flaps were sutured with 4.0 Cytoplast polytetrafluoroethylene sutures (Osteogenics Biomedical). Postoperative instructions were given, along with a prescription for 875 mg of amoxicillin and clavulanic acid (Augmentin; GlaxoSmithKline) orally twice per day and 15 mL of chlorhexidine mouthrinse to be used gently for 30 seconds twice per day. For pain, the patient was instructed to take 600 mg of ibuprofen every 6 hours as needed.
At the 1-week postoperative appointment, the patient reported no pain during the initial few days after surgery. However, he stopped taking amoxicillin and clavulanic acid 3 days after the surgery because he could not tolerate it due to severe diarrhea. He started feeling dull pain at tooth no. 19 after stopping antibiotic therapy. Intraoral examination revealed that the surgical site had no exudate and all sutures and the membrane were in place. However, soft tissue at the tooth no. 19 site was red and painful during palpation. The patient was prescribed a course of 500 mg of amoxicillin orally 3 times per day, which he tolerated well. After taking amoxicillin for 3 days, the patient began experiencing the same degree of dull pain at the surgical site and reported a “decay” taste. Intraoral examination revealed findings similar to those at the 7-day postoperative examination. To exclude the possibility of soft-tissue irritation from the Cytoplast membrane, the sutures and membrane were removed 10 days after extraction and ridge preservation. No exudate was observed from the bone graft within the socket. The bone graft was irrigated once with chlorhexidine and then multiple times with sterile water. A BioXclude (Snoasis Medical) membrane was placed to cover the bone graft, and the soft tissue was then sutured with 4.0 Cytoplast polytetrafluoroethylene sutures.
Figure 1Periapical radiograph 5 weeks after extraction and ridge preservation.
Revision surgery of ridge preservation at tooth no. 19 site was performed 8 weeks after extraction owing to loss of the coronal portion of the bone graft. After local anesthesia with 2% lidocaine with 1:100,000 epinephrine, a midridge incision at tooth no. 18 through tooth no. 19 and an intrasulcular incision at tooth no. 20 were made, full-thickness flaps were reflected, and the ridge height at tooth no. 19 was enhanced with a mixture of mineralized and demineralized cortical bone particulates and a DynaMatrix membrane (Keystone Dental Group), followed by reposition of the flaps and suture with 5.0 Cytoplast polytetrafluoroethylene sutures. Primary closure was achieved. The patient was prescribed another course of 500 mg of amoxicillin orally 3 times per day and 15 mL chlorhexidine mouthrinse to be used gently for 30 seconds twice per day. For pain, the patient was instructed to take 600 mg of ibuprofen every 6 hours as needed.

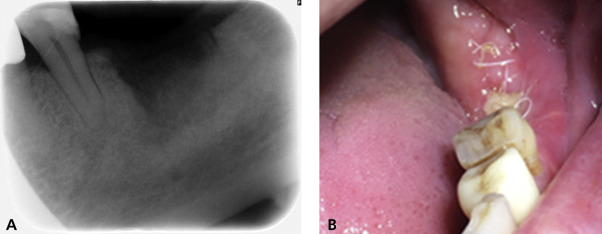
Figure 2Clinical photographs 1 week (A) and 2 weeks (B) after the revision surgery. Membrane exposure and gingival inflammation are shown.
The patient’s oncologist was consulted, citing concerns that imatinib was interfering with the healing process. The oncologist agreed that the patient could discontinue imatinib, and the patient stopped taking it 12 days after the revision surgery.

Figure 3At 4 weeks after revision surgery. A. Periapical radiograph. B. Clinical photograph indicating soft-tissue healing and decrease of gingival inflammation.

Figure 4Clinical presentation 6 weeks after revision surgery. A. Periapical radiograph indicating the loss of coronal portion of the bone graft. B. Clinical photograph showing healed soft tissue.

Figure 5At 28 weeks after revision surgery. A. Clinical photograph (occlusal view) showing that soft tissue healed completely and the previous indentation at tooth 19 no. site was filled. B. Periapical radiograph revealing bone loss was still present.
Discussion
Safety of Medicines: A Guide to Detecting and Reporting Adverse Drug Reactions.
When evaluating potential ADRs in humans, the Naranjo Adverse Drug Reaction Probability Scale is used frequently to assess causality when ruling out potential confounding variables.
- Naranjo C.A.
- Busto U.
- Sellers E.M.
- et al.
In our patient’s case, the Naranjo scale ranks this ADR as probable due to imatinib therapy. Supporting facts for this ranking are that delayed gingival healing resolved after discontinuing imatinib therapy, and no alternative causes could explain the ADR. In addition, the ADR was confirmed with objective clinical evidence. At the time of this writing, the patient continues to take imatinib, but because no additional oral surgical procedures have been performed, we cannot assess for reoccurrence of the ADR.
- Shah D.R.
- Dholakia S.
- Shah R.R.
However, these warnings are based on a precautionary principle and generally lack formal clinical trial data.
- Shah D.R.
- Dholakia S.
- Shah R.R.
There are 2 case reports, summarized in the table, in which investigators reported that imatinib can delay healing of leg ulcers
- Ronicke M.
- Erfurt-Berge C.
and cause wound disruption.
In both of these reports, the ADR subsided after discontinuing imatinib (Table).
- Ronicke M.
- Erfurt-Berge C.
,
In another study, investigators reported that discontinuation of imatinib before dental surgery facilitates early implant results (Table).
The mechanism behind these findings and the imatinib-induced delay in gingival healing in our case is unknown at this time. Some researchers have suggested a mechanism of PDGF-receptor inhibition because activity of PDGF-AA, an isoform of PDGF, is associated with wound healing.
- Ronicke M.
- Erfurt-Berge C.
,
- Mwaura B.
- Mahendran B.
- Hynes N.
- et al.
Furthermore, in mice, a reduction in PDGF-AA expression is associated with impaired wound healing.
- Beer H.D.
- Longaker M.T.
- Werner S.
Imatinib also impaired the onset of cutaneous wound healing and collagen biosynthesis in transgenic mice, believed to be a consequence of PDGF-receptor inhibition.
- Rajkumar V.S.
- Shiwen X.
- Bostrom M.
- et al.
Neutropenia is another putative explanation for the delayed gingival healing observed in our patient. Neutropenia is a known ADR of imatinib.
- Zhu J.
- Yang Y.
- Zhou L.
- Jiang M.
- Hou M.
Neutrophils play a role in tissue repair,
and patients with neutropenia can have impaired wound healing.
Finally, imatinib’s downregulation of collagen proteins (Col1A1, Col3A1) and metalloproteinases was reported to explain delayed healing after bowel surgery in rats.
- Lee J.C.
- Chen C.H.
- Chen T.C.
- Yeh C.N.
- Yeh T.S.