Abstract
Background
Patient–provider cost conversations can minimize cost-related barriers to health, while improving treatment adherence and patient satisfaction. The authors sought to identify factors associated with the occurrence of cost conversations in dentistry.
Methods
This was a cross-sectional study using data from an online, self-administered survey of US adults who had seen a dentist within the past 24 months at the time of the survey. Multivariable hierarchical logistic regression analysis was used to identify patient and provider characteristics associated with the occurrence of cost conversations.
Results
Of the 370 respondents, approximately two-thirds (68%) reported having a cost conversation with their dental provider during their last dental visit. Cost conversations were more likely for patients aged 25 through 34 years (odds ratio [OR], 2.84; 95% CI, 1.54 to 5.24), 35 through 44 years (OR, 3.35; 95% CI, 1.50 to 7.51), and 55 through 64 years (OR, 3.39; 95% CI, 1.38 to 8.28) than patients aged 18 through 24 years. Cost conversations were less likely to occur during visits with dental hygienists than during visits with general or family dentists (OR, 0.25; 95% CI, 0.11 to 0.58). In addition, respondents from the South (OR, 1.90; 95% CI, 1.04 to 3.48) and those screened for financial hardship were more likely to report having cost conversations with their dental providers (OR, 6.70; 95% CI, 2.69 to 16.71).
Conclusions
Within the study sample, cost conversations were common and were facilitated via financial hardship screening.
Practical Implications
Modifying oral health care delivery processes to incorporate financial hardship screening may be an effective way to facilitate cost conversations and provision of patient-centered care.
Key Words
Abbreviation Key:
NA (Not applicable)
- Vujicic M.
- Buchmueller T.
- Klein R.
and in 2015, more than 10% of the US population across all income levels avoided or delayed oral health care due to cost.
- Vujicic M.
- Buchmueller T.
- Klein R.
As medical and dental expenses in the United States increase rapidly, patients are left with a considerable financial burden—a trend that calls for increased consideration and sensitivity to patients’ cost concerns from medical and oral health care providers.
- Brick D.J.
- Scherr K.A.
- Ubel P.A.
,
- Pisu M.
- Schoenberger Y.-M.
- Herbey I.
- et al.
One way to accomplish this is to prioritize cost conversations between patients and their health care providers as part of a shared decision-making process. Such conversations can allow health care providers to identify the sources and magnitude of financial stress for patients and, in partnership with patients, tailor the care plan in a manner that minimizes the cost concerns of patients.
- Pisu M.
- Schoenberger Y.-M.
- Herbey I.
- et al.
- Carpenter E.
- Seidman J.
- Ganesan N.
- AyoVaughn M.
- Bardin R.
The concept of cost conversations is being explored increasingly in medical care, particularly in oncology and other high-cost medical specialties.
- Bradham D.D.
- Garcia D.
- Galván A.
- Erb C.
Guidelines for effective cost conversations in the clinical settings include making such conversations routine and for all patients, providing patients with resources to understand their health care costs and address cost concerns, and tailoring treatment plans in a manner that is responsive to patients’ cost concerns.
- Fiscella K.
- Fox K.
- Gill L.
- et al.
,
- Erwin K.
- Fitzpatrick V.
- Gill L.
- et al.
Researchers have reported that patients prefer having cost conversations with their physicians and that such conversations indicate that physicians have the patients’ best interests in mind.
- Brick D.J.
- Scherr K.A.
- Ubel P.A.
Despite the importance of cost conversations and patients’ desire for such conversations, they occur rarely, due to provider-related barriers such as provider discomfort with having these conversations, fear of damaging patient–provider relationships, lack of time, and lack of role clarity.
- Brick D.J.
- Scherr K.A.
- Ubel P.A.
Although few researchers have characterized patient-related barriers to cost conversations, there is evidence to suggest that factors such as fear and discomfort with discussing cost issues with medical providers may prevent patients from initiating cost discussions with their providers.
- Dine C.J.
- Masi D.
- Smith C.D.
Within dentistry, little is known about the extent to which cost conversations occur, despite the considerable cost-related barriers to oral health care. Specifically, to the best of our knowledge, there has been no empirical examination of whether and how cost conversations are happening within the oral health care setting. We sought to examine the factors associated with the occurrence of cost conversations between patients and oral health care providers.
Methods
Setting, population, and sample
- Kranz A.M.
- Chen A.
- Gahlon G.
- Stein B.D.
Our research team partnered with Qualtrics to recruit 500 participants to complete a self-administered online survey. Sample size determination is less straightforward for nonprobability samples, and there is no widely accepted guideline. A probability-based sample of 385 would provide sufficient power for a prevalence estimation precision rate of plus or minus 5% at a 95% confidence level. Using this as a reference point, a sample size of 500 was identified as adequate for balancing the power to detect medium differences with survey cost and providing some cushion for nonresponse.
- Lutfiyya M.N.
- Gross A.J.
- Soffe B.
- Lipsky M.S.
Adults aged 18 through 44 years were overrepresented in the study sample (67.4% vs 45.4% previously reported national estimate).
- Lutfiyya M.N.
- Gross A.J.
- Soffe B.
- Lipsky M.S.
Recruitment
Qualtrics relies on actively managed opt-in market panels for study recruitment, including niche panels for specialized recruitment campaigns. Potential participants are invited to participate via email and are incentivized via Qualtrics. Internet protocol address tracking and digital fingerprinting technology are leveraged to prevent duplication.
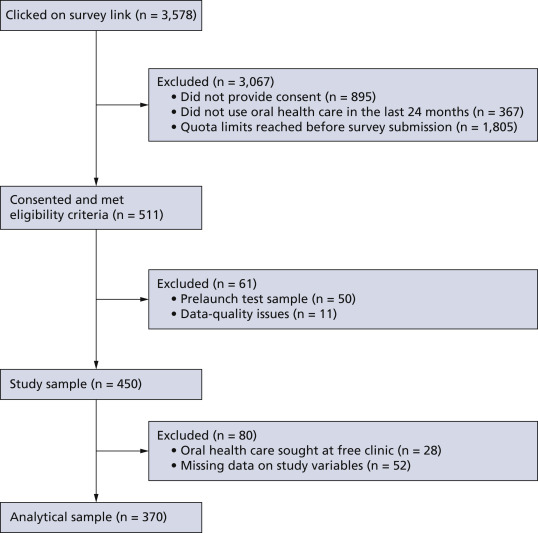
FigureSample recruitment flowchart.
Data collection
- ▪
The race and ethnicity question (previously combined into 1 question) was split into 2 (that is, race and then ethnicity) to allow for ease of quota determination; Qualtrics requested this change.
- ▪
Additional questions were included about site of dental visits (public, private, free clinic) and overall satisfaction with the dental visit.
Data were collected using an online self-administered survey developed by researchers on the basis of a review of the cost conversations literature. The survey was developed specifically for our study and, as such, had not been validated previously. To minimize survey fatigue and obtain trustworthy answers, the survey was designed to be short (facilitated using skip patterns where applicable); average completion time was 6 minutes.
- ▪
“For our research, careful attention to the survey questions is critical” (participants had to select “I understand”; participants selecting “I do not understand” were excluded).
- ▪“People are very busy these days and many do not have time to follow what goes on in their communities or countries. We are testing whether people read questions. To show that you’ve read this much, answer both “extremely interested” and “very interested” (participants selecting options other than the 2 specified options were excluded, n = 11).14Characteristics of participants and satisficing tendency in online surveys using a sample provider. Psyarxiv.
To ensure data quality, Qualtrics’ internal processes facilitate checks for evidence of satisficing, including short completion times and straightlining in questions using matrix style. Such observations are excluded and do not count toward the contractual final sample determination. For our study, there was 1 such observation. However, this respondent also responded inaccurately to the attention checks and was already accounted for in the surveys that had been deleted for data quality issues, as described previously.
Informed Consent
Participants had to consent to participating in our study before beginning the survey and after being presented with information about our study’s purpose and expectations of participants. Voluntary participation was stressed. The institutional review board at Georgia Southern University reviewed and approved the study protocol and survey.
Measures
Responses to these 2 statements were combined into a single binary measure (yes, no) of cost conversation. Participants responding in the affirmative to either of these statements were deemed to have had a cost conversation during their last dental visit. Participants responding in the negative for both statements were deemed not to have had a cost conversation.
Assessed covariates included patient demographic and provider information. Demographic information included gender (female, male, nonbinary), age (18-24 years, 25-34 years, 35-44 years, 45-54 years, 55-64 years, ≥ 65 years), race or ethnicity (non-Hispanic White, non-Hispanic Black, non-Hispanic other, Hispanic), personal income (< $25,000, $25,000 through $49,999, $50,000 through $74,999, $75,000 through $99,000, ≥ $100,000), location of residence (county with population of < 50,000, county with population of ≥ 50,000), dental insurance coverage (yes, no), experience of financial hardship (yes, no), and when the dental visit occurred (within 6 months, 7-12 months ago, 13-24 months ago). Provider characteristics included the type of practice in which the visit occurred (public, private), type of provider seen (general dentist, specialist dentist, dental hygienist or other), and whether the patient was screened for financial hardship during the visit (yes, no).
Data analysis
Participants who reported obtaining care from a free clinic (n = 28) were excluded for the purposes of our study owing to its focus on cost. After the exclusion of observations with missing data on the study variables, the final analytical sample for our study was 370, slightly fewer than the anticipated 385. However, had this been a probability-based study, the sample size of 370 would provide sufficient power for a prevalence estimation precision rate of plus or minus 5.1% at a 95% confidence level, just a little over the 5% margin of error estimated for a sample of 385.
Variables were described using frequencies. Bivariable associations were assessed using χ2 tests. Multivariable logistic regression was used to identify the patient and provider characteristics independently associated with the occurrence of cost conversations. A hierarchical model building approach was adopted in which patient characteristics, provider characteristics, and financial hardship screening information were added in blocks sequentially (models 1-3, respectively). Statistical significance was assessed at the P < .05 level using 2-tailed tests. Robust SEs were obtained and clustered at the state level. All analyses were performed using STATA, Version 16 (StataCorp).
Results
Characteristics of survey respondents
Table 1Sociodemographic characteristics of participants (n = 370).
Occurrence of cost conversations in the dental setting
Factors associated with cost conversations in the dental setting
Table 2Factors associated with cost conversations in the oral health care setting (n = 370).
Patient Characteristics
Age was found to be statistically associated with cost conversations, even after adjusting for patient and provider characteristics and financial hardship screening. Findings from model 3 indicate that cost conversations with dental providers were more likely to occur for patients aged 25 through 34 years (odds ratio [OR], 2.84; 95% CI, 1.54 to 5.24; P = .001), 35 through 44 years (OR, 3.35; 95% CI , 1.50 to 7.51; P = .003), and 55 through 64 years (OR, 3.39; 95% CI, 1.38 to 8.28; P = .008) than for patients aged 18 through 24 years. Hispanics were approximately 2 times more likely to have cost conversations with their dental providers, after adjusting for patient and provider characteristics (OR, 2.01; 95% CI, 1.08 to 3.73; P = .027). However, this association was no longer statistically significant at the P < .05 level, after adjusting for screening for financial hardship in model 3 (OR, 1.93; 95% CI, 0.90 to 4.13; P = .092).
Provider Characteristics
Financial Hardship Screening
Discussion
Our aim was to identify the factors associated with the occurrence of patient–dental provider cost conversations. Approximately two-thirds of survey respondents reported having a cost conversation with a dentist or clinical staff member during their last dental visit. In multivariable regression analysis, factors found to be independently associated with cost conversations included patient’s age, experience of financial hardship, region of residence, type of dental provider seen, and financial hardship screening. Screening for financial hardship was found to be the most important factor associated with the occurrence of cost conversations in our study.
- Alexander G.C.
- Casalino L.P.
- Meltzer D.O.
,
- Hunter W.G.
- Hesson A.
- Davis J.K.
- et al.
,
- Brown G.D.
- Hunter W.G.
- Hesson A.
- et al.
,
- Tipirneni R.
- Patel M.R.
- Kirch M.A.
- Goold S.D.
,
- Skaljic M.
- Patel I.H.
- Pellegrini A.M.
- Castro V.M.
- Perlis R.H.
- Gordon D.D.
,
- Warsame R.
- Kennedy C.C.
- Kumbamu A.
- et al.
,
- Harrington N.G.
- Scott A.M.
- Spencer E.A.
although in a 2021 study, investigators reported a cost conversation rate as high as 77% among patients with atrial fibrillation.
- Kamath C.C.
- Giblon R.
- Kunneman M.
- et al.
Cost conversations about anticoagulation between patients with atrial fibrillation and their clinicians: a secondary analysis of a randomized clinical trial.
We propose 3 possible explanations for this finding. On the one hand, differences in reported estimates may be due to variations in how cost conversation is defined and measured. On the other hand, our use of a nonprobability sampling approach may have biased the estimates. Online opt-in panel samples have previously been reported to yield higher estimates on nondemographic questions than nationally representative benchmark samples; reported estimates of the differences ranged from 2% through 14%.
- Brüggen E.
- van den Brakel J.A.
- Krosnick J.
,
- Yeager D.S.
- Krosnick J.A.
- Chang L.
- et al.
,
- Lehdonvirta V.
- Oksanen A.
- Räsänen P.
- Blank G.
However, in previous studies, researchers have also reported that the magnitude of these differences tended to be considerably lower with Qualtrics’ online panels, especially those using a quota sampling approach (as was done in our study) than other online survey sampling options.
- Lehdonvirta V.
- Oksanen A.
- Räsänen P.
- Blank G.
,
- Zack E.S.
- Kennedy J.
- Long J.S.
,
- Boas T.C.
- Christenson D.P.
- Glick D.M.
However, assuming the cost conversation rate estimated from our study is close to the true national estimate, it would suggest that cost conversations may be a relatively routine practice in dentistry. It is possible that dental providers are more cost-responsive compared with their medical counterparts due to the relatively higher price elasticity and out-of-pocket burden associated with oral health care.,
- Manning Jr., W.G.
- Phelps C.E.
Additional research using probability-based samples is needed to accurately estimate the frequency of cost conversations in both medical and dental settings before comparisons can be made.
- Harrington N.G.
- Scott A.M.
- Spencer E.A.
The literature has identified insurance coverage, income, and financial and resource needs as facilitators of cost conversations.
- Harrington N.G.
- Scott A.M.
- Spencer E.A.
,
- Kamath C.C.
- Giblon R.
- Kunneman M.
- et al.
Cost conversations about anticoagulation between patients with atrial fibrillation and their clinicians: a secondary analysis of a randomized clinical trial.
In our study, age, region of residence, Hispanic ethnicity, reported financial hardship, and specialist dental visits were all found to be positively associated with cost conversations. Hispanic ethnicity, age, and South region have previously been associated with higher unmet need for oral health care or a higher likelihood of reported cost-related barriers to oral health care use.
- Vujicic M.
- Buchmueller T.
- Klein R.
,,
- Chrisopoulos S.
- Luzzi L.
- Brennan D.S.
,
Consumer Survey of Barriers to and Facilitators of Access to Oral Health Service.
Positive associations between reported financial hardship and Hispanic ethnicity and cost conversations were no longer statistically significant after adjusting for financial hardship screening, suggestive of higher financial hardship screening rates among these populations. Similarly, financial hardship screening appeared to mediate the positive relationship between specialist dental visits and cost conversations, also suggesting higher financial hardship screening rates in such settings. Dental subspecialty services tend to be more expensive, perhaps explaining the higher financial hardship screening rates and incidence of cost conversations. This is corroborated by the finding of a lower occurrence of cost discussions during dental hygienist visits, when the preventative services provided tend to be more affordable.
- Yabroff K.R.
- Bradley C.
- Shih Y.C.T.
Given that a subset of people, including those who experience financial hardship, may be hesitant to have cost conversations,
- Dine C.J.
- Masi D.
- Smith C.D.
making financial hardship screening routine can be a helpful approach for identifying patient financial stress and ensuring the delivery of cost-responsive, quality, patient-centered, oral health care to all patients.
Limitations
Our study was a cross-sectional study, and therefore we cannot assert causal associations between each of the assessed correlates of cost conversations and the occurrence of cost conversations. Furthermore, we recruited participants using a nonprobability sampling approach from an opt-in market panel, resulting in potential selection and voluntary response bias. The extent to which the findings may be generalized to the broader population, especially older adults, may be considerably limited.
There were also some limitations with the survey instrument used in our study, including lack of previous validation. Participants could have also responded to questions related to cost conversations with different frames of reference, leading to potential bias. In addition, the questions used in assessing cost conversations focused on discussions related solely to medical costs. Furthermore, the quality checks used in the survey were placed at the beginning rather than interspersed within the survey, which allowed us to immediately exclude those who did not have serious intentions about the survey from the start. However, given the brevity of the survey, we believe quality issues due to survey fatigue were of limited concern. Collectively, these survey-related factors could have potentially influenced the validity of the responses and our resulting estimates.
In addition, we may not have accounted for all potential correlates of cost conversations, including patients’ education or employment and providers’ attitudes and beliefs toward cost conversations. In addition, detailed information on the type of dental visit the patient had (for example, diagnostic visit, preventive or hygiene visits, treatment visits, or reviews) or the site of care (including whether care was received in a hospital-based or dental education institution–based dental facility) were not obtained.
- Lutfiyya M.N.
- Gross A.J.
- Soffe B.
- Lipsky M.S.
The 24-month period allowed for adequate sampling and afforded the opportunity to account for the potential impact of the pandemic on oral health care experiences. We included a variable in the regression model measuring when the last dental visit took place. The lack of statistically significant association of this variable with cost conversations suggests that the pandemic and time-related recall bias may have had a minimal effect on estimates.
Despite these limitations, our study represents one of the only attempts to our knowledge to examine cost conversations within the dental setting. Because we took an empirical approach, our study results add to a cost conversation evidence base that has mostly been dominated by qualitative studies. In future studies, researchers can extend this exploratory study using nationally representative and probability-based sampling approaches to confirm the broad applicability of our study’s findings. Furthermore, additional studies are needed to develop valid measurement instruments for assessing the occurrence and quality of cost conversations.
Conclusions
Our aim was to fill a gap in the literature via examining the factors associated with patient–dental provider cost conversations. Taken together, the findings suggest that patient–dental provider cost conversations, partly facilitated by financial hardship screening, may be occurring for financially vulnerable populations and in high-cost oral health care settings. The findings also support the need for routine financial hardship screening in oral health care settings to identify and address patients’ cost concerns and to facilitate the delivery of quality, patient-centered, and cost-responsive oral health care.
References
Wall T, Guay A. The per-patient cost of dental care, 2013: a look under the hood. Health Policy Institute research brief. American Dental Association. Accessed September 10, 2021. https://www.ada.org/-/media/project/ada-organization/ada/ada-org/files/resources/research/hpi/hpibrief_0316_4.pdf
Reversible Decay: Oral Health Is a Public Health Problem We Can Solve. DentaQuest. 2019. Accessed September 10, 2021. https://dentaquest.com/pdfs/reports/reversible-decay.pdf
Dental care presents the highest level of financial barriers, compared to other types of health care services.
Health Aff (Millwood). 2016; 35: 2176
The impact of cost conversations on the patient-physician relationship.
Health Commun. 2019; 34: 65-73
Perspectives on conversations about costs of cancer care of breast cancer survivors and cancer center staff: a qualitative study.
Ann Intern Med. 2019; 170: S54-S61
Measuring the effectiveness of cost-of-care conversations.
Avalere. September 22, 2020. 2020;
Cost-of-care conversations during clinical visits in federally qualified health centers: an observational study.
Ann Intern Med. 2019; 170: S87-S92
How to welcome cost-of-care conversations in your practice.
Avalere. 2018;
Considerations for facilitating cost-of-care conversations with vulnerable patients.
Avalere. 2018;
A review of cost communication in oncology: patient attitude, provider acceptance, and outcome assessment.
Cancer. 2017; 123: 928-939
Tools to help overcome barriers to cost-of-care conversations.
Ann Intern Med. 2019; 170: S36-S38
2020 Trends in dental office visits during the COVID-19 pandemic.
JADA. 2021; 152: 535-541.e1
Dental care utilization: examining the associations between health services deficits and not having a dental visit in past 12 months.
BMC Public Health. 2019; 19: 1-13
Characteristics of participants and satisficing tendency in online surveys using a sample provider. Psyarxiv.
Patient-physician communication about out-of-pocket costs.
JAMA. 2003; 290: 953-958
Patient-physician discussions about costs: definitions and impact on cost conversation incidence estimates.
BMC Health Serv Res. 2016; 16: 1-12
Discussing out-of-pocket expenses during clinical appointments: an observational study of patient-psychiatrist interactions.
Psychiatr Serv. 2017; 68: 610-617
Cost conversations between primary care providers and patients with expanded Medicaid coverage.
J Gen Intern Med. 2018; 33: 1845-1847
Prevalence of financial considerations documented in primary care encounters as identified by natural language processing methods.
JAMA Netw Open. 2019; 2e1910399
Conversations about financial issues in routine oncology practices: a multicenter study.
J Oncol Pract. 2019; 15: e690-e703
Working toward evidence-based guidelines for cost-of-care conversations between patients and physicians: a systematic review of the literature.
Soc Sci Med. 2020; 258
Cost conversations about anticoagulation between patients with atrial fibrillation and their clinicians: a secondary analysis of a randomized clinical trial.
JAMA Netw Open. 2021; 4e2116009
Establishing the Accuracy of Online Panels for Survey Research.
Statistics Netherlands,
2016Comparing the accuracy of RDD telephone surveys and internet surveys conducted with probability and non-probability samples.
Public Opin Q. 2011; 75: 709-747
Social media, web, and panel surveys: using non-probability samples in social and policy research.
Policy Internet. 2021; 13: 134-155
Can nonprobability samples be used for social science research?: a cautionary tale.
Surv Res Methods. 2019; 13: 215-227
Recruiting large online samples in the United States and India: Facebook, Mechanical Turk, and Qualtrics.
Political Sci Res Methods. 2020; 8: 232-250
The demand for dental care.
The Bell J Econ. 1979 Oct 1; : 503-525
Cost Barriers to Dental Care Among the U.S. Population, by Race and Ethnicity. Health Policy Institute. American Dental Association. Accessed September 10, 2021. https://www.ada.org/-/media/project/ada-organization/ada/ada-org/files/resources/research/hpi/hpigraphic_0421_3.pdf
Trends in dental visiting avoidance due to cost in Australia, 1994 to 2010: an age-period-cohort analysis.
BMC Health Serv Res. 2013; 13: 1-8
Consumer Survey of Barriers to and Facilitators of Access to Oral Health Service.
Cost Matters. Delta Dental. Accessed September 10, 2021. https://www.deltadental.com/us/en/member/cost-estimator.html
Understanding financial hardship among cancer survivors in the United States: strategies for prevention and mitigation.
J Clin Oncol. 2020; 38: 292
Biography
Ms. Brown is an undergraduate student and a McNair Scholar, Department of Health Policy and Community Health, Jiann-Ping Hsu College of Public Health, Georgia Southern University, Statesboro, GA.
Dr. Apenteng is an associate professor, Department of Health Policy and Community Health, Jiann-Ping Hsu College of Public Health, Georgia Southern University, Statesboro, GA.
Dr. Opoku is an associate professor, Department of Health Policy and Community Health, Jiann-Ping Hsu College of Public Health, Georgia Southern University, Statesboro, GA.
Article Info
Publication History
Published online: May 16, 2022
Publication stage
In Press Corrected Proof
Footnotes
Disclosures. None of the authors reported any disclosures.
This study was conducted with funding support from the Georgia Southern University McNair Scholars Program and Department of Health Policy and Community Health at the Jiann-Ping Hsu College of Public Health , Georgia Southern University . The Georgia Southern University institutional review board reviewed and approved this study.
Identification
DOI: https://doi.org/10.1016/j.adaj.2022.04.003
Copyright
© 2022 American Dental Association. All rights reserved.
ScienceDirect
Access this article on ScienceDirect