Abstract
Background
Low-income adults delay oral health care due to cost more than any other health care service. These delays lead to caries, periodontal disease, and tooth loss. Expanding Medicaid dental coverage has increased dental visits, but the potential impact on previously unmet oral health needs is not well understood.
Methods
In this analysis, the authors estimated the association between Medicaid dental expansion and tooth loss. Data on self-reported tooth loss among adults below 138% federal poverty guideline were obtained from the Behavioral Risk Factor Surveillance System. A difference-in-differences regression was estimated. Additional analyses stratified according to age and separated extensive and limited dental benefits.
Results
Expanding Medicaid dental coverage is associated with increased probability of total tooth loss of 1 percentage point in the total sample, representing a 20% relative increase from the pre-expansion rate. This increase was concentrated in states offering extensive dental benefits and was largest (2.5-percentage-point greater likelihood) among adults aged 55 through 64 years for whom both extensive and limited dental benefits were associated with total tooth loss.
Conclusions
Medicaid expansion with extensive dental benefits was associated with increased total tooth loss among low-income adults. This finding suggests that greater access to oral health care addressed previously unmet oral health needs for this population.
Practical Implications
As public dental coverage continues to expand, dental care professionals may find themselves treating a greater number of patients with substantial, previously unmet, oral health needs. Additional research to understand the long-term effects of Medicaid dental insurance for adults on their oral health is needed.
Key Words
Abbreviation Key:
ACA (Patient Protection and Affordable Care Act), BRFSS (Behavioral Risk Factors Surveillance System)
- Vujicic M.
- Buchmueller T.
- Klein R.
Delaying or forgoing oral health care can allow periodontal disease and caries to progress, which can eventually lead to increased tooth loss. Adult tooth loss diminishes health and well-being, as well as overall quality of life and employment opportunities.
- Friedman P.K.
- Kaufman L.B.
- Karpas S.L.
,
- Huang D.L.
- Chan K.C.G.
- Young B.A.
Low-income adults bear the greatest burden of tooth loss; 60% of low-income adults aged 25 through 64 years have lost a permanent tooth (compared with 40% of higher-income adults) and 1 in 10 low-income adults have no remaining teeth by the age of 65 years.
- Vujicic M.
- Buchmueller T.
- Klein R.
,
- Dye B.A.
- Li X.
- Beltran-Aguilar E.D.
,
- Dye B.A.
- Thornton-Evans G.
- Li X.
- Iafolla T.J.
,
Total tooth loss among persons aged > or =65 years: selected states, 1995-1997.
Dental care expenditures and insurance.
,
MACPAC. Medicaid and CHIP Payment and Access Commission. June 2016.
,
Kaiser Family Foundation.
Yet, the federal government does not require Medicaid plans to cover adult dental services, so Medicaid dental programs vary among states.
- Wehby G.L.
- Lyu W.
- Shane D.M.
In 2018, 4 states did not cover any adult Medicaid dental services and 15 states reimbursed providers for emergency dental treatment only.
MACPAC. Medicaid and CHIP Payment and Access Commission. June 2016.
Even among states covering nonemergency dental services, Medicaid plans differ across states in benefits and services covered.
MACPAC. Medicaid and CHIP Payment and Access Commission. June 2016.
In addition, state Medicaid eligibility also varies. The Patient Protection and Affordable Care Act (ACA)
Patient Protection and Affordable Care Act, Pub L No. 111-148, 124 Stat 119 (2010).
expanded Medicaid by means of raising the income-based eligibility threshold to 138% of the federal poverty guideline. However, low-income adults living in states that have not yet opted to expand Medicaid, or those that do not cover nonemergency dental services, continue to lack access to dental insurance. Differences in dental coverage availability and Medicaid eligibility have resulted in a public dental system rife with inequity, inconsistency, and coverage gaps.
- Wehby G.L.
- Lyu W.
- Shane D.M.
,
Patient Protection and Affordable Care Act, Pub L No. 111-148, 124 Stat 119 (2010).
,
,
,
- Vujicic M.
- Yarbrough C.
- Nasseh K.
The pre-ACA Medicaid expansion in Oregon was associated with reduced unmet dental needs among adults gaining new dental coverage.
- Baicker K.
- Allen H.L.
- Wright B.J.
- Taubman S.L.
- Finkelstein A.N.
,
,
- Mitchell J.B.
- Haber S.G.
- Khatutsky G.
- Donoghue S.
There is evidence of increased use of dental services in states that expanded Medicaid under the ACA and offered dental benefits.
- Lyu W.
- Shane D.M.
- Wehby G.L.
,
- Cawley J.
- Soni A.
- Simon K.
,
- Farietta T.P.
- Lu B.
- Tumin R.
Furthermore, there is evidence of larger effects of ACA Medicaid expansion on dental services use with more generous dental benefits.
- Wehby G.L.
- Lyu W.
- Shane D.M.
,
- Lyu W.
- Shane D.M.
- Wehby G.L.
Building on the evidence that Medicaid dental expansions increased oral health care use, we hypothesized that new access to dental coverage could affect oral health outcomes.
In another study, researchers reported that ACA Medicaid expansion was associated with greater likelihood of edentulism (total tooth loss).
- Elani H.W.
- Sommers B.D.
- Kawachi I.
However, when categorizing states according to whether they offered dental benefits to Medicaid adults, those researchers reported an opposite, small, and statistically nonsignificant association between total tooth loss and expansion with dental benefits. Furthermore, those researchers did not include any other levels of tooth loss or extraction (only edentulism). Finally, in another study, investigators reported no association between state Medicaid dental benefits and tooth loss in low-income adults 65 years and older.
- Singhal A.
- Alofi A.
- Garcia R.I.
- Sabik L.M.
Methods
Data
Each year, BRFSS includes a new cross-sectional sample in each state. During even years, BRFSS administers an oral health module that includes a measure of self-reported tooth loss up to the interview date. The questionnaire specifically asks for the number of teeth extracted due to caries or periodontal disease, excluding third molars unless they were extracted due to caries or disease.
BRFSS categorizes that measure as 0 tooth loss; losing 5 or fewer teeth; losing 6 or more, but not all, teeth; and losing all teeth. We included data from 2 years before the Medicaid expansion (2010, 2012) and 3 years after the 2014 expansions (2014, 2016, 2018). BRFSS also obtains data on demographic and socioeconomic characteristics.
Sample
,
State treatment and control group assignment
MACPAC. Medicaid and CHIP Payment and Access Commission. June 2016.
,
Kaiser Family Foundation.
,
- Semprini J.
- Lyu W.
- Shane D.M.
- Wehby G.L.
,
Kaiser Family Foundation.
,
Respondents in states that did not expand Medicaid under the ACA from 2014 through 2018 were assigned to the control group. We excluded respondents in Medicaid expansion states that did not cover dental benefits beyond emergency services for adults. This left respondents in 19 states that expanded Medicaid from 2014 through 2018 and whose Medicaid programs covered more than emergency-only dental benefits. Nine Medicaid expansion states offered extensive dental benefits, covering more services with higher or nonexistent annual caps.
The other 10 expansion states offered limited dental benefits, defined as lower annual cap on benefits and fewer services covered.
Statistical analysis
,
To distinguish between the levels of Medicaid dental benefits, we estimated an additional model that separated expansion states into those offering extensive benefits and those offering limited benefits. For all analyses, standard errors were clustered at the state level.
The regression models were estimated for each of the 4 tooth loss categories, 1 at a time, relative to the other 3 categories using a linear probability model and sampling weights from BRFSS. Specifically, we estimated the association of Medicaid expansion and the likelihood of 0 tooth loss; losing 5 or fewer teeth; losing 6 or more, but not all, teeth; and losing all teeth, each relative to the other categories combined, in a separate regression for each outcome. In addition to estimating the average effect in the total sample, we estimated effects for subgroups stratified according to 10-year age categories from 25 through 34 years to 55 through 64 years because age is associated with greater prevalence of tooth loss and more accumulated unmet oral health care needs.
Results
Values are weighted rates (%) for all outcome variables (binary measures of tooth loss) and (binary) control variables, unless otherwise indicated.
of outcome and control variables according to year for Medicaid expansion
Expansion group includes all states that expanded Medicaid under the Patient Protection and Affordable Care Act11 from 2014 through 2018 and cover nonemergency dental benefits under Medicaid.
and nonexpansion
Nonexpansion group includes all states that did not expand Medicaid under the Patient Protection and Affordable Care Act during the study period.
states.
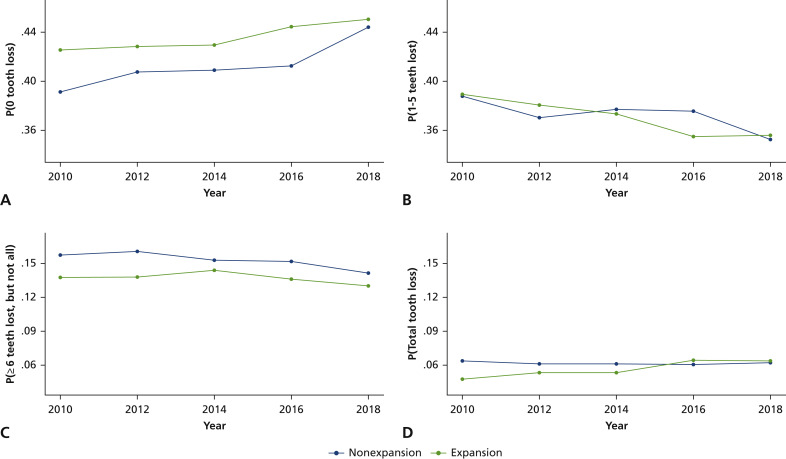
FigureWeighted mean tooth loss rates, according to Medicaid expansion and nonexpansion states. Year-by-year, weighted mean tooth loss rates for states that expanded Medicaid dental coverage (and states that did not expand Medicaid). Expansion states include states that expanded in 2014, as well as states that expanded after 2014 but before 2018. A. Zero teeth lost. B. One through 5 teeth lost. C. Six or more (not all) teeth lost. D. Total tooth loss.
Association between Medicaid expansion and tooth loss
Estimates from model 1 of effect of expanding Medicaid dental coverage on each probability of tooth loss category. Robust standard errors (SE) are clustered at the state level.
of Medicaid dental expansion on likelihood of tooth loss.
Associations according to level of dental benefits
Estimates from model 2 of effect of expanding extensive Medicaid dental coverage and limited Medicaid dental coverage on each probability of tooth loss category. Extensive and limited benefits were estimated by separate regressions. Robust standard errors (SE) are clustered at the state level.
of Medicaid dental expansion on likelihood of tooth loss according to level of coverage.
Estimates according to age groups
Estimates from models 1 and 2 of effect of expanding Medicaid dental coverage on each probability of tooth loss category, by 10-year age groups. The overall effect, extensive coverage, and limited coverage were estimated by separate regressions. Robust standard errors (SE) are clustered at the state level. Sample size ranges from 29,500 through 60,963. Each outcome is measured as a binary 0/1 variable, and so the effect estimates represent a change in the outcome probability on a 0 through 1 scale.
of Medicaid dental expansion on tooth loss according to age groups.
Discussion
- Wehby G.L.
- Lyu W.
- Shane D.M.
,
Patient Protection and Affordable Care Act, Pub L No. 111-148, 124 Stat 119 (2010).
,
- Baicker K.
- Allen H.L.
- Wright B.J.
- Taubman S.L.
- Finkelstein A.N.
Researchers investigating dental treatment use also reported that Medicaid expansion was associated with increasing likelihood of major dental treatments 4 percentage points and caries treatment 9 percentage points.
,
- Lyu W.
- Shane D.M.
- Wehby G.L.
Our finding that the Medicaid expansion was associated with a 1.1-percentage-point increase in total tooth loss is consistent overall with findings from prior studies and indicates that low-income adults responded to new access to dental coverage via addressing previously unmet dental needs.
With new dental coverage, adults enrolled in Medicaid programs that offered extensive dental benefits (covering more services and higher annual spending caps per beneficiary) may face fewer financial barriers to accessing dental services, increasing the likelihood of receiving care for previously untreated caries and periodontal disease. This result suggests that low-income adults without Medicaid dental coverage face barriers and delays in getting necessary dental treatments, which ultimately lead to tooth loss. Low-income adults in nonexpansion states and expansion states that do not offer extensive dental benefits are particularly vulnerable to these risks.
- Semprini J.
- Ulrich F.
- Mueller K.
,
People below 100% of the federal poverty guideline generally continue to be eligible for Medicaid. However, results of a 2021 study showed no associations between state Medicaid dental benefits and tooth loss for low-income adults 65 years or older using BRFSS data from 2014 through 2018.
- Singhal A.
- Alofi A.
- Garcia R.I.
- Sabik L.M.
One possible explanation is that changes in tooth loss occurred before age 65 years, as our study results suggested.
Our study results represent several contributions to the literature on Medicaid dental benefits and oral health. Our study is among the first to examine the associations between Medicaid expansions involving different levels of dental benefits under the ACA and tooth loss of low-income nonolder adults. Moreover, we examined the severity of tooth loss on the basis of the number of teeth extracted and not just total tooth loss. By means of examining different ranges of tooth loss, we shed light on associations of different levels of previously unmet oral health needs and new access to oral health care. For some, new access was associated with more teeth extracted due to high previously unmet needs. For others, access might prevent the need for additional tooth loss. Finally, we evaluated differences according to age, providing a more comprehensive understanding of the oral health needs of adults eligible for Medicaid. As more states expand Medicaid eligibility and dental benefits, more work is needed to understand the effects of Medicaid dental coverage expansions on oral health equity. Such future research could examine how new access to dental coverage affects unmet dental needs across demographic and geographic factors. Furthermore, as younger adults gain dental coverage, understanding how long-term access to coverage affects periodontitis, caries, and tooth loss prevention remains important.
One limitation of our study was a lack of data on changes in oral health over time for the same people. Without such data, we could not definitively assess how people transition between the different categories of tooth loss over time. Instead, we evaluated changes in the probabilities of each category to infer this flow. The middle categories (≤ 5 and ≥ 6, but not all, teeth lost) may have opposite changes in transition that could offset each other. However, this limitation had little effect on our main inference on the likelihood of total tooth loss and the likelihood of 0 tooth loss.
Conclusions
Medicaid dental coverage expansions revealed large previously unmet oral health needs among low-income adults, reflected in an increase in total tooth loss likely due to needed extractions. This result was concentrated in states offering extensive dental benefits and for adults aged 55 through 64 years. Consistent with prior studies, these findings indicate that low-income adults gained access to needed oral health care after ACA Medicaid expansions that offer generous dental benefits.
Supplemental Data
References
Dental care presents the highest level of financial barriers, compared to other types of health care services.
Health Aff (Millwood). 2016; 35: 2176-2182
Oral health disparity in older adults: dental decay and tooth loss.
Dent Clin North Am. 2014; 58: 757-770
Poor oral health and quality of life in U.S. older adults with diabetes.
J Am Geriatr Soc. 2013; 61
Selected oral health indicators in the United States, 2005-2008.
NCHS Data Brief. 2012; 96: 1-8
Dental caries and tooth loss in adults in the United States, 2011–2012.
NCHS Data Brief. 2015; 197
Total tooth loss among persons aged > or =65 years: selected states, 1995-1997.
MMWR Morb Mortal Wkly Rep. 1999; 48: 206-210
Dental care expenditures and insurance.
in: Public Policy Options for Better Dental Health: Report of a Study. National Academies Press,
1980: 73-92MACPAC. Medicaid and CHIP Payment and Access Commission. June 2016.
Kaiser Family Foundation.
The impact of the ACA Medicaid expansions on dental visits by dental coverage generosity and dentist supply.
Med Care. 2019; 57: 781
Patient Protection and Affordable Care Act, Pub L No. 111-148, 124 Stat 119 (2010).
Do Medicaid benefit expansions have teeth? The effect of Medicaid adult dental coverage on the use of dental services and oral health.
J Health Econ. 2015; 44: 212-225
More Rhode Island adults have dental coverage after the Medicaid expansion: did more adults receive dental services? Did more dentists provide services?.
R I Med J (2013). 2017; 100: 51-53
The effect of the Affordable Care Act’s expanded coverage policy on access to dental care.
Med Care. 2014; 52: 715-719
The effect of Medicaid on dental care of poor adults: evidence from the Oregon Health Insurance Experiment.
Health Serv Res. 2018; 53: 2147-2164
Impact of Oregon’s priority list on Medicaid beneficiaries.
Med Care Res Rev. 2000; 57: 216-234
Impact of the Oregon Health Plan on access and satisfaction of adults with low income.
Health Serv Res. 2002; 37: 11-31
Effects of the recent Medicaid expansions on dental preventive services and treatments.
Med Care. 2020; 58: 749-755
Third year of survey data shows continuing benefits of Medicaid expansions for low-income childless adults in the U.S.
J Gen Intern Med. 2018; 33: 1495-1497
Ohio’s Medicaid expansion and unmet health needs among low-income women of reproductive age.
Matern Child Health J. 2018; 22: 1771-1779
Changes in coverage and access to dental care five years after ACA.
Health Aff (Millwood). 2020; 39: 1900-1908
Medicaid adult dental benefits and oral health of low-income older adults.
JADA. 2021; 152: 551-559.e1
2018 BRFSS Survey Data and Documentation. Centers for Disease Control and Prevention.
Were Patient Protection and Affordable Care Act spillover gains to private dental coverage for dependents widely shared? An analysis using Medical Expenditure Panel Survey data.
JADA. 2020; 151: 182-189
Did the Affordable Care Act’s dependent coverage mandate increase premiums?.
J Health Econ. 2015; 41: 1-14
The effects of ACA Medicaid expansions on health after 5 years.
Med Care Res Rev. 2022; 79: 28-35
Kaiser Family Foundation.
Compendium: states’ Medicaid fee-for-service adult dental services coverage policies: trends in Medicaid spending. MACPAC. Medicaid and CHIP Payment and Access Commission. January 2021.
Oral health in North Carolina relationship with general health and behavioral risk factors.
N C Med J. 2015; 76: 142-147
Do socioeconomic conditions explain ethnic inequalities in tooth loss among US adults?.
Ethn Dis. 2018; 28: 201-206
A practitioner’s guide to cluster-robust inference.
J Hum Resour. 2015; 50: 317-372
2019 Availability of supplemental benefits in Medicare advantage plans in rural and urban areas. RUPRI Center for Rural Health Policy Analysis. Rural Policy Brief. February 2021.
The high coverage of dental, vision, and hearing benefits among Medicare Advantage enrollees.
Inquiry. 2019; 56 ()
Biography
Mr. Semprini is a PhD candidate, Department of Health Management and Policy, College of Public Health, and a research fellow, College of Dentistry, University of Iowa, Iowa City, IA.
Dr. Wehby is a professor and the John W. Colloton Chair, Departments of Health Management and Policy, Economics, and Preventive and Community Dentistry, and Public Policy Center, Director of Graduate Studies, Department of Health Management and Policy, University of Iowa, Iowa City, IA, and a research associate, National Bureau of Economic Research, Cambridge, MA.
Article Info
Publication History
Published online: May 03, 2022
Publication stage
In Press Corrected Proof
Footnotes
Disclosures. Mr. Semprini and Dr. Wehby did not report any disclosures.
This study was funded by grants T90 DE023520-08 and 1R03 DE02804101 from the National Institute of Dental and Craniofacial Research, National Institutes of Health.
Identification
DOI: https://doi.org/10.1016/j.adaj.2022.03.003
Copyright
© 2022 American Dental Association. All rights reserved.
ScienceDirect
Access this article on ScienceDirect