Abstract
Background
Primary cutaneous cluster of differentiation 30–positive (CD30+) T-cell lymphoproliferative
disorders are the second most common type of skin T-cell lymphoma. The lesions exhibit
an indolent course, with a morphology resembling high-grade T-cell lymphoma.
Case Description
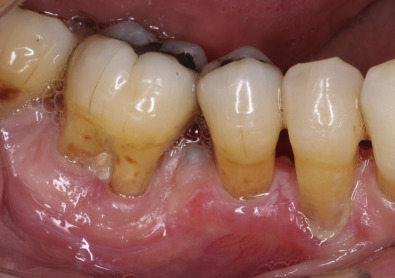
A 67-year-old healthy man sought treatment for a large nonhealing ulcer on the buccal
gingiva of the mandibular right premolars. He reported a history of recurrent cutaneous
lesions, for which he was seen 1 year earlier at a hospital. Results of incisional
biopsy showed a dense lymphoid cell infiltrate composed of atypical CD30+ T-cells
intermixed with eosinophils. The diagnosis was updated to CD30+ T-cell lymphoproliferative
disorder, which was similar to the cutaneous lesion diagnosis. The lesion area healed
completely, and there were no signs of recurrence at 18-month follow-up.
Practical Implications
Oral CD30+ T-cell lymphoproliferative disorder has a favorable outcome, but it is
commonly misdiagnosed. Biopsy is crucial and should be combined with clinical examination
to avoid chemotherapeutic treatments intended for high-grade lymphoma.
Key Words
Abbreviation Key:
CD (Cluster of differeniation), EBER (Epstein-Barr virus–encoded small nuclear RNA), IHC (Immunohistochemistry), LyP (Lymphomatoid papulosis), NA (Not applicable), pcALCL (Primary cutaneous anaplastic large-cell lymphoma), pcCD30+ T-LPD (Primary cutaneous cluster of differentiation 30–positive T-cell lymphoproliferative
disorder), TCR (T-cell receptor)
To read this article in full you will need to make a payment
References
CD30-positive lymphoproliferative disorders.
Cancer Treat Res. 2019; 176: 249-268
A new era for cutaneous CD30-positive T-cell lymphoproliferative disorders.
Semin Diagn Pathol. 2017; 34: 22-35
Primary mucosal CD30-positive T-cell lymphoproliferative disorders of the head and neck rarely involving epiglottis: clinicopathological, immunohistomchemical and genetic features of a case.
Int J Clin Exp Pathol. 2015; 8: 11685-11690
WHO-EORTC classification for cutaneous lymphomas.
Blood. 2005; 105: 3768-3785
Lymphomatoid papulosis: treatment response and associated lymphomas in a study of 180 patients.
J Am Acad Dermatol. 2016; 74: 59-67
Applicability and prognostic value of the new TNM classification system in 135 patients with primary cutaneous anaplastic large cell lymphoma.
Arch Dermatol. 2009; 145: 1399-1404
CD30+ cutaneous lymphoproliferative disorders: the Stanford experience in lymphomatoid papulosis and primary cutaneous anaplastic large cell lymphoma.
J Am Acad Dermatol. 2003; 49: 1049-1058
CD30-positive T-cell lymphoproliferative disorder of the oral mucosa: an indolent lesion—report of 4 cases.
Int J Surg Pathol. 2008; 16: 286-290
The spectrum of CD30+ T cell lymphoproliferative disorders in the skin.
Chin Clin Oncol. 2019; 8: 3
Traumatic ulcerative granuloma with stromal eosinophilia: clinical case report, literature review, and differential diagnosis.
World J Surg Oncol. 2019; 17: 184
Eosinophil-rich CD30+ lymphoproliferative disorder of the oral mucosa: a form of “traumatic eosinophilic granuloma.”.
Am J Clin Pathol. 2004; 121: 43-50
Traumatic eosinophilic granuloma of the oral mucosa: a CD30+(Ki-1) lymphoproliferative disorder?.
Oral Oncol. 1997; 33: 375-379
Oral involvement in lymphomatoid papulosis: report of two cases and review of the literature.
Dermatology. 2005; 210: 53-57
Lymphomatoid papulosis type A: clinical, morphologic, and immunophenotypic study.
Int J Dermatol. 1997; 36: 514-517
Mucosal CD30-positive T-cell lymphoproliferative disorder arising in the oral cavity following dental implants: report of the first case.
Int J Surg Pathol. 2015; 23: 656-661
Involvement of tongue by lymphomatoid papulosis.
Am J Dermatopathol. 1998; 20: 522-526
Mucosal involvement in a patient with lymphomatoid papulosis.
J Am Acad Dermatol. 2001; 44: 339-341
Critical review of lymphomatoid papulosis of the oral cavity with case report.
Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2000; 90: 195-204
Afectación de la mucosa oral por papulosis linfomatoide.
Actas Dermosifiliogr. 2007; 98: 265-267
Solitary oral ulceration as the first appearance of lymphomatoid papulosis: a diagnostic challenge.
Clin Exp Dermatol. 2010; 35: 165-168
Necrotic mucosal CD30-positive ulcer on the oral mucosa: a self-healing lymphoma.
Br J Oral Maxillofac Surg. 2017; 55: 859-860
A new classification scheme for periodontal and peri-implant diseases and conditions: introduction and key changes from the 1999 classification.
J Periodontol. 2018; 89: S1-S8
- Swerdlow S.H. Campo E. Harris N.L. WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues. Revised 4th edition. International Agency for Research on Cancer,
2017 Mucosal CD30-positive T-cell lymphoproliferations of the head and neck show a clinicopathologic spectrum similar to cutaneous CD30-positive T-cell lymphoproliferative disorders.
Mod Pathol. 2012; 25: 983-992
Primary and secondary cutaneous CD30+ lymphoproliferative disorders: a report from the Dutch Cutaneous Lymphoma Group on the long-term follow-up data of 219 patients and guidelines for diagnosis and treatment.
Blood. 2000; 95: 3653-3661
Biography
Dr. Nguyen is a dental student, Professional Program for International Dentists, Section of Periodontics, UCLA School of Dentistry, Los Angeles, CA.
Biography
Dr. Yaghsezian is a postgraduate resident, Section of Periodontics, UCLA School of Dentistry, Los Angeles, CA.
Biography
Dr. Lin is an associate professor, Section of Oral and Maxillofacial Pathology, UCLA School of Dentistry, Los Angeles, CA.
Biography
Dr. Klokkevold is a professor of clinical dentistry and residency program director, Section of Periodontics, UCLA School of Dentistry, Los Angeles, CA.
Article Info
Publication History
Published online: October 28, 2021
Publication stage
In Press Corrected Proof
Footnotes
Disclosure. None of the authors reported any disclosures.
The authors are grateful to all of the members of sections of periodontics and oral and maxillofacial pathology, UCLA School of Dentistry, for their help and support for the completion of the case.
Identification
DOI: https://doi.org/10.1016/j.adaj.2021.07.015
Copyright
© 2021 American Dental Association. All rights reserved.
ScienceDirect
Access this article on ScienceDirect