Abstract
Background
Oral health is influenced by social determinants of health (SDH), predisposing people and communities to greater risk of developing caries. This study evaluated the association between caries risk in adults and SDH such as ZIP Codes, systemic diseases, payment methods, and race or ethnicity.
Methods
The BigMouth Dental Data Repository (n = 57,211) was used to extract clinical and SDH data from patients’ dental electronic health records for 2019. Caries risk categories were used as ZIP Code data was merged with the Social Deprivation Index, a composite measure of area-level deprivation based on 7 demographic characteristics collected in the American Community Survey.
Results
The results showed that the odds of being in the high caries risk group were higher for people in the 49- to 64-year age group (adjusted odds ratio [aOR], 2.24; 95% CI, 2.08 to 2.40; P ≤ .001), men (aOR, 1.19; 95% CI, 1.13 to 1.25; P ≤ .001), people who had comorbidities (diabetes: aOR, 1.16; 95% CI, 1.08 to 1.24; P ≤ .001; cardiovascular disease: aOR, 1.40; 95% CI, 1.32 to 1.50), and people with an Social Deprivation Index score above the 75th percentile (aOR, 2.39; 95% CI, 2.21 to 2.58; P ≤ .001). In addition, Hispanic and Black people had higher odds of being at high caries risk than other races or ethnicities (Hispanic: aOR, 3.05; 95% CI, 2.32 to 4.00; Black: aOR, 2.05; 95% CI, 1.02 to 4.01).
Conclusions
This study shows the association of caries risk with higher social deprivation, reinforcing the role of structural and upstream factors in oral health. This study is unique in using recorded ZIP Code information and assessing caries risk levels for those regions.
Practical Implications
The physical and structural environment should be considered contributors to caries risk in people.
- Lang W.P.
- Borgnakke W.S.
- Taylor G.W.
- Woolfolk M.W.
- Ronis D.L.
- Nyquist L.V.
and is a complex chronic disease influenced by biological and environmental factors.
,
Improving Access to Oral Health Care for Vulnerable and Underserved Populations.
,
Adults with advanced-stage caries experience severe tooth pain, dental infection, and tooth loss.
,
- Zero D.T.
- Fontana M.
- Martínez-Mier E.A.
- et al.
,
- Featherstone J.D.B.
- Chaffee B.W.
Complications in oral health reduce the quality of life because of pain, reduced nutritional intake, and social ramifications.
- Schwendicke F.
- Dörfer C.E.
- Schlattmann P.
- Foster Page L.
- Thomson W.M.
- Paris S.
Pain and associated complications caused by caries can affect the performance of daily life and work-related tasks.
- Patrick D.L.
- Lee R.S.
- Nucci M.
- Grembowski D.
- Jolles C.Z.
- Milgrom P.
- Patrick D.L.
- Lee R.S.
- Nucci M.
- Grembowski D.
- Jolles C.Z.
- Milgrom P.
Social determinants of health (SDH) such as income, race or ethnicity, and education level have been shown to predict oral health status and risk of caries.
- Schwendicke F.
- Dörfer C.E.
- Schlattmann P.
- Foster Page L.
- Thomson W.M.
- Paris S.
,
- Singh A.
- Peres M.A.
- Watt R.G.
People with household and individual income levels below the federal poverty level have increased odds ratios of poor oral health and prevalence of caries than people with higher incomes.
- Singh A.
- Peres M.A.
- Watt R.G.
Likewise, race or ethnicity and education level are established predictors of caries, oral health status, and systemic health complications leading to poor quality of life.
Historically underserved populations in the United States, such as Hispanics, Latinos, and Blacks, are at greater risk of caries and other oral health–related diseases because of inequities and inequalities.
- Wu B.
- Liang J.
- Plassman B.L.
- Remle R.C.
- Bai L.
,
- Splieth C.H.
- Christiansen J.
- Foster Page L.A.
,
- Henshaw M.M.
- Garcia R.I.
- Weintraub J.A.
,
,
- Jamieson L.
- Peres M.A.
- Guarnizo-Herreño C.C.
- Bastos J.L.
Oral health inequities and inequalities are environmental influences that increase the risk of developing caries.
- Schwendicke F.
- Dörfer C.E.
- Schlattmann P.
- Foster Page L.
- Thomson W.M.
- Paris S.
Similarly, low education levels are associated with reduced access to dental care, resulting in higher frequency and severity of dental disease.
- Costa S.M.
- Martins C.C.
- Bonfim Mde. L.
- et al.
,
- Duijster D.
- van Loveren C.
- Dusseldorp E.
- Verrips G.H.
Socioeconomic position follows a similar pattern; lower socioeconomic position is associated with a higher prevalence of poor oral health and caries.
- Schwendicke F.
- Dörfer C.E.
- Schlattmann P.
- Foster Page L.
- Thomson W.M.
- Paris S.
- Fontana M.
- Carrasco-Labra A.
- Spallek H.
- Eckert G.
- Katz B.
Caries risk assessments take into consideration disease indicators, biological risk factors, and host protective factors. The Caries Management by Risk Assessment procedure and its philosophy has been the leading caries risk assessment tool since its conception in the early 2000s.
It is an appropriate predictor of caries risk at an individual level; however, there is room for further development, and Fontana and colleagues
- Fontana M.
- Carrasco-Labra A.
- Spallek H.
- Eckert G.
- Katz B.
urged the establishment of a better caries risk predictive model. SDH such as ZIP Code, race or ethnicity, systemic comorbidities, and lack of adequate insurance coverage or dental insurance type can add a layer of predictors for caries risk at the population level that can be added to improve the Caries Management by Risk Assessment procedure.
- Henshaw M.M.
- Garcia R.I.
- Weintraub J.A.
For example, community and neighborhood-level factors, including ZIP Code, have been shown to be a predictor of caries risk in Black people.
- Ismail A.I.
- Sohn W.
- Tellez M.
- Willem J.M.
- Betz J.
- Lepkowski J.
SDH can be used to determine people’s access to healthy foods and health care and even to determine life expectancy.
- Singh G.K.
- Daus G.P.
- Allender M.
- et al.
Comparatively, SDH could be used to aid in predicting caries risk levels. This study is the first step to connect SDH and caries risk to understand the potential relationships between SDH and caries risk at the population level.
- Butler D.C.
- Petterson S.
- Phillips R.L.
- Bazemore A.W.
This study examines the association of caries risk and specific SDH, including the Social Deprivation Index (SDI),
as a composite measure of area-level deprivation.
Methods
Overview
This cross-sectional, retrospective study was reviewed by and provided with exempt status by the Colorado Multiple Institutional Review Board. The BigMouth Consortium for Oral Health Research and Informatics clinical review committee, consisting of participating institutions, also reviewed and approved the study.
Data source
- Walji M.F.
- Kalenderian E.
- Stark P.C.
- et al.
,
- Bhardwaj A.
- Ramoni R.
- Kalenderian E.
- et al.
,
- Walji M.F.
- Spallek H.
- Kookal K.K.
- et al.
The repository was developed using partially deidentified EHR data and consists of more than 3 million medical and dental records from 11 dental schools. The repository is referred to as partially deidentified because it contains ZIP Code data, which is an identifying component of patient history according to the Health Insurance Portability and Accountability Act.
EHR data are entered during clinical appointments by both dental students and faculty oral health care providers. The repository houses data on demographic variables, dental procedure codes, procedures, medication history, and self-reported overall patient health, thus making it one of the largest repositories of oral and systemic health information. Data extraction was completed after obtaining approval from the BigMouth dental data review committee and the Colorado Multiple Institutional Review Board.
- Butler D.C.
- Petterson S.
- Phillips R.L.
- Bazemore A.W.
,
- Phillips R.L.
- Liaw W.
- Crampton P.
- et al.
,
- Liaw W.
- Krist A.H.
- Tong S.T.
- et al.
SDI is a composite measure of area-level deprivation and is used to quantify socioeconomic variation in health outcomes.
- Butler D.C.
- Petterson S.
- Phillips R.L.
- Bazemore A.W.
SDI is based on 7 demographic characteristics collected in the American Community Survey
: percentage of people living in poverty, percentage of people with less than 12 years of education, percentage of single-parent households, percentage of people living in rented housing units, percentage of people living in overcrowded housing units, percentage of households without a car, and percentage of unemployed adults younger than 65 years. These data are from the 2015 SDI files.
Dependent variable
- American Dental Association.
This study used CDT codes as a filtering mechanism to identify the population of interest. We defined multiple dependent variables using CDT codes for dental procedures and nomenclature for caries risk assessment and documentation, using codes for low risk (D0601), moderate risk (D0602), and high risk (D0603).
- American Dental Association.
We categorized the variables as low vs medium caries risk, low vs high caries risk, and medium vs high caries risk.
Primary independent variable
The primary independent variable was defined by categorizing SDI scores into 4 categories: the 25th percentile or less, within the 26th through 50th percentiles, within the 51st through 75th percentiles, and more than the 75th percentile.
Covariates
- ▪
age categorized as 21 through 33 years, 34 through 48 years, 49 through 64 years, and 65 through 80 years (only adults aged ≥ 21 years were included in this study)
- ▪
sex categorized as female, male, or other
- ▪
race or ethnicity categorized as White, Black, Asian, Hispanic, or American Indian, Alaskan Native, Pacific Islander, multiple, or other
- ▪
insurance coded as private, public, or other
- ▪
existing diabetes or cardiovascular disease diagnosis coded as no vs yes
Data analyses
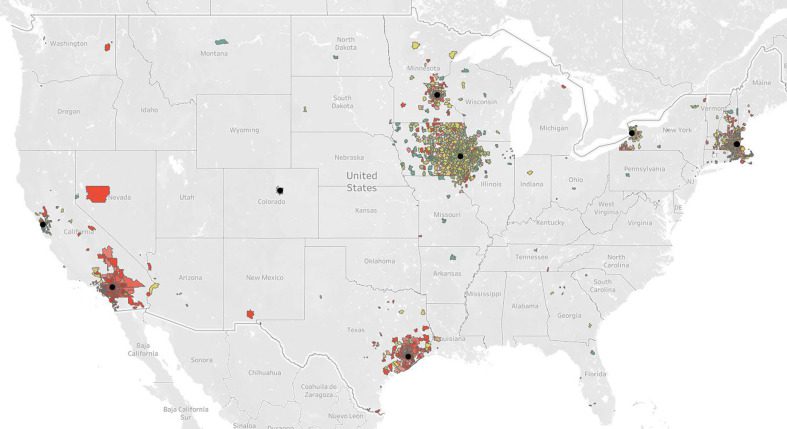
Descriptive analyses were conducted, stratified by low, medium, and high caries risk, to summarize frequencies and proportions for each of the independent and confounding variables. To illustrate the proportion of caries risk by ZIP Code, a map was created to visualize the distribution of caries risk on a spectrum from low through high based on ZIP Code. Multivariable logistic regression models were used to examine associations between neighborhood-level SDI and caries risk categories after adjusting for age, sex, and the presence of diabetes and cardiovascular disease. Data quality was assessed in several ways. Data were reviewed to ensure that all values fell within reasonable value ranges or the range of possible response options. Patterns of missing data were evaluated to ensure that the data did not need to be imputed. Patterns of CDT code use, especially in risk scores, were determined to be not overly biased by school or clinician effects that would need to be accounted for in the model. Statistical model assumptions were tested using a common statistical diagnoses test and outlier analysis was performed to ensure that the statistically significant findings were not driven by the presence of outliers.
We ran 2 separate regression models to examine the dependent variables of low vs high caries risk and medium vs high caries risk. Two separate regression models were run to test interaction variables (race or ethnicity and SDI interaction and age and SDI interaction). The logistic regression models produce adjusted odds ratios (aORs), which account for the other predictors in the model. When evaluating an odds ratio adjusted for our study, an aOR greater than 1 indicates higher adjusted odds of outcome, whereas an aOR less than 1 indicates lower adjusted odds of the outcome. All analyses were performed with Stata 16.0 (StataCorp), and a P value less than .05 was deemed to be statistically significant.
Results
All variables were pulled from dental electronic health records. Social Deprivation Index data were merged with ZIP Code information provided in dental records.
Furthermore, when stratified on the basis of SDI percentile, 56.2% of patients residing in ZIP Codes at the 25th percentile or less of SDI scores, 55.9% of patients in the 26th through 50th percentiles, 55.6% of patients in the 51st through 75th percentiles, and 75.4% of patients in greater than the 75% percentile were assessed as being at high caries risk. Correspondingly, fewer patients who resided in ZIP Codes with SDI scores were assessed as being at medium caries risk.
- American Dental Association.
ZIP Code zones in red have the highest proportion of high caries risk; areas in yellow have a greater proportion of medium caries risk; and areas in green have a greater proportion of low caries risk. Black dots represent anchor ZIP Codes where charting information was obtained.
Caries risk level was pulled from dental charts based on clinical diagnosis and extracted for comparison based on designated caries risk level Current Dental Terminology codes in dental electronic health records. All other variables were also pulled from dental electronic health records.
Caries risk level was pulled from dental charts based clinical diagnosis and extracted for comparison based on designated caries risk level Current Dental Terminology code in dental electronic health records. All other variables were also pulled from dental electronic health records.
An interaction between race or ethnicity and SDI score was evaluated using a logistic model (n = 16,995) for low vs high caries risk. Hispanic people above the 75th SDI percentile were 3.05 times more likely to be at high caries risk. In addition, Black people above the 75th SDI percentile were 2.05 times more likely to be diagnosed with high caries risk (Hispanic: aOR, 3.05; 95% CI, 2.32 to 4.00; Black: aOR, 2.05; 95% CI, 1.02 to 4.01).
An interaction between age and SDI score was evaluated using a logistic model (n = 42,079) for low vs high caries risk. People aged 49 through 64 years and in the 51st through 75th SDI percentile were 1.5 times more likely to be at high caries risk. In addition, people aged 65 through 80 years and in the 51st through 75th SDI percentile, and those aged 65 through 80 years and above the 75th SDI percentile were more likely to be diagnosed with high caries risk (49-64 years in the 51st-75th SDI percentile: aOR, 1.5; 95% CI, 1.3 to 1.9; 65-80 years in the 51st-75th SDI percentile: aOR, 1.8; 95% CI, 1.6 to 2.9; 65-80 years above the 75th SDI percentile: aOR, 1.5; 95% CI, 1.3 to 1.9).
Discussion
- Schwendicke F.
- Dörfer C.E.
- Schlattmann P.
- Foster Page L.
- Thomson W.M.
- Paris S.
,
- Singh A.
- Peres M.A.
- Watt R.G.
Assessing the association between caries risk and SDI of the ZIP Code in which the patient resides provides a unique insight into the association of social deprivation with higher caries risk.
Dental schools often provide lower-cost dental services and thus attract patients of lower socioeconomic status, who in turn often have higher caries risk.
The results showed, in both multivariate analyses, that people with an SDI score greater than 75th percentile showed significantly higher odds of being evaluated as having high caries risk. These results are, of course, not determinative, but instead show that patients residing in ZIP Codes with higher social deprivation scores are more likely to be assessed as having high caries risk, adjusting for all the other variables in the model.
The age and SDI interaction showed that older adults (≥ 65 years) living in greater social deprivation had higher caries risk. About 15% of older adults (≥ 65 years) live in poverty,
- Cubanski J.
- Koma W.
- Damico A.
- Neuman T.
and oral health disparities persist in older adults living in poverty.
These interactions highlight how upstream variables, in this case lower socioeconomic position, can be significant predictors of higher caries risk.
In addition, the latest Oral Health in America report indicates that working-aged adults have the highest prevalence of caries of all adults, which sets the stage for caries as a highly prevalent chronic disease throughout adulthood.
The odds ratio in our study decreases somewhat between the 49- through 64-year and 65- through 80-year age groups. This could be due to the loss of dentition for the oldest adults in the high caries risk category.
- Lipsky M.S.
- Su S.
- Crespo C.J.
- Hung M.
- Mauri-Obradors E.
- Estrugo-Devesa A.
- Jané-Salas E.
- Viñas M.
- López-López J.
,
- Almusawi M.A.
- Gosadi I.
- Abidia R.
- Almasawi M.
- Khan H.A.
,
- Beukers N.
- Su N.
- Loos B.G.
- van der Heijden G.
A higher percentage of patients with these self-reported systemic comorbidities were in the high caries risk category than in the low and medium caries risk categories. Caries has been found to be an independent risk factor for the development of atherosclerosis.
- Glodny B.
- Nasseri P.
- Crismani A.
- et al.
One study that analyzed the relationship between caries risk and cardiovascular disease concluded that patients who had advanced or severe caries were at greater risk of cardiovascular disease.
- Kim K.
- Choi S.
- Chang J.
- et al.
This study further showed a dose-dependent relationship with the number of visits for severe or advanced caries and risk of cardiovascular disease. Diabetes also was associated with caries risk in this study. Diabetes can increase a person’s level of caries risk because of reduced salivary flow.
- Mauri-Obradors E.
- Estrugo-Devesa A.
- Jané-Salas E.
- Viñas M.
- López-López J.
Changes in salivary flow affect the host’s ability to prevent microbial growth in the form of dental plaque, the primary etiology for caries.
,
Few reports indicate a relationship between diabetes and caries.
- Mauri-Obradors E.
- Estrugo-Devesa A.
- Jané-Salas E.
- Viñas M.
- López-López J.
,
- Almusawi M.A.
- Gosadi I.
- Abidia R.
- Almasawi M.
- Khan H.A.
However, well-documented oral health complications associated with diabetes include periodontal disease.
- Verhulst M.J.L.
- Loos B.G.
- Gerdes V.E.A.
- Teeuw W.J.
Oral manifestations in patients with diabetes can potentially increase their caries risk, but a causal relationship remains elusive and further research is needed in this area.
Our study has a few limitations to consider. The data found within the BigMouth Dental Data Repository are not intended for research purposes; rather, they were collected for record keeping in a clinical setting. Thus, these data were extracted from EHRs and repurposed, based on the desired variables, as previously described. The data set is not representative of the entire US population and is collected from US dental schools that have participated in creating the BigMouth Dental Data Repository. The data set was skewed toward patients at high caries risk because the data were collected from dental schools, which may act as safety nets for people with greater dental needs. The study used a cross-sectional design, which does not allow examination of trends over time.
The merger of ZIP Code data with SDI provides a spotlight on the relationship of caries risk with social deprivation and highlights oral health care disparities in adults associated with SDH, a fact that is well known but is rarely examined. Further longitudinal research is warranted to gain a deeper understanding of this association.
Conclusions
This study shows the association of caries risk with higher social deprivation, thereby reinforcing the role of structural and upstream factors in oral health.